A. Vanderbilt1, W.K. Barsoum2, A. Kumar3, L. Capone4, C.R. Szubski2, B.J. Messinger-Rapport5
Nursing Excellence, Cleveland Clinic, Cleveland, OH, USA; 2. Department of Orthopaedic Surgery, Orthopaedic and Rheumatologic Institute, Cleveland Clinic, Cleveland, CT, USA; 3. Chief of Medicine, Department of Medicine, Hartford Hospital, Hartford, CT, USA; 4. Certified Nurse Practitioner, Center for Connected Care, Cleveland Clinic, Cleveland, OH, USA; 5. Center for Geriatric Medicine, Cleveland Clinic, Cleveland, OH, USA
Corresponding Author: Barbara J. Messinger-Rapport, MD, PhD, Directer, Center for Geriatric Medicine, 9500 Euclid Ave, X-10, Cleveland Clinic, Cleveland, OH 44195, rapporb@ccf.org
Abstract
Objective: Post-surgical nursing interventions can reduce but not eliminate the risk of delirium. A preoperative screen for delirium risk which discriminates between those persons at lower versus higher risk of delirium may help future research efforts develop a subject pool for intensive interventions to reduce delirium incidence. The aim of this study is to assess the ability of a previously developed and tested delirium screening tool, the Cleveland Clinic Confusion Score (CCCS), to predict delirium in a select population. Design: Prospective, observational study. Setting/Participants: Convenience sample of 111 adults aged 50 years or older presenting to a preoperative orthopedic clinic. Intervention: We integrated the CCCS into the preoperative evaluation for elective hip and knee surgery. Postoperatively, clinical care nurses screened patients for delirium twice daily using the Nursing Delirium Screening Scale (Nu-DESC). Research nurses gathered additional data regarding postoperative confusion from the chart and family after discharge. Measurements: Primary outcome was the predictive value of the CCCS for delirium. Results: Of the 111 subjects, a positive preoperative CCCS screen was recorded in 31 individuals (27.9%) and postoperative delirium was identified in 12 individuals (10.8%). CCCS assessment in this population had a positive predictive value of 29% and a negative predictive value of 96%. Conclusion: When a delirium screening tool is incorporated into the preoperative process and coupled with a nursing tool for delirium detection, clinicians can identify a subset of older elective orthopedic surgery patients unlikely to develop postoperative delirium. Preoperative delirium screening may help clinicians focus perioperative interventions on higher risk individuals to further reduce delirium risk beyond current, postoperative nursing interventions.
Key words: Delirium, risk stratification, elective orthopedic surgery.
Introduction
Postoperative delirium (POD) following elective orthopedic surgery is common, affecting up to 28% of elective orthopedic patients (1). POD is associated with psychological distress, prolonged hospital stay, greater admission costs, and increased risk of falls, nursing home placement, and mortality (2-4). Furthermore, hospitalized patients with Alzheimer’s disease who develop delirium have an increased risk of cognitive decline, institutionalization, and death (5).
Although delirium is a common and serious consequence of surgery, it is often unrecognized and untreated (4). Additionally, the complete pathophsiology of delirium is still unclear (6). One reason for lack of recognition is that the presentation of delirium is heterogeneous, and may appear as hypoactive, hyperactive, mixed, or subsyndromal. Delirium, particularly the hypoactive form, may be mistaken for dementia or depression. There are many known risk factors for delirium: advanced age, dementia, medical illness, polypharmacy, alcohol abuse, male gender, poor functional status, depression, pain, increased blood urea nitrogen/creatinine (BUN/Cr) ratio, and sensory impairment (7). Medical risk factors, particularly cognitive impairment at admission, are also predictors of post-operative delirium in elderly hip-surgery patients (8).
A variety of interventions after admission have been reported to reduce the incidence of delirium in medical and surgical patients by 25-40% (9, 10). The interventions described in these studies consisted of tailoring nursing care to typical problems of the older individual, including promoting nutrition and mobility, removing bladder catheters early and facilitating bowel regularity, reducing disruptions in sleep, reducing sensory deficits with adaptive equipment where appropriate, and promoting temporal and geographical orientation (9, 10). Unfortunately, hospital nursing interventions reduce delirium risk, but do not eliminate it. There are pharmacological interventions in pilot studies which suggest that prophylactic antipsychotic drugs may reduce delirium risk (11-13). However, unlike delirium-specific nursing interventions, antipsychotics and other proposed pharmacological agents have potential adverse effects, and the data is limited.
Given the high incidence, morbidity, and mortality associated with POD, a preoperative risk stratification that helps predict POD in surgical patients may allow the clinical care team to more appropriately allocate interventions and resources to help reduce POD risk before occurrence. This study addressed the feasibility of incorporating risk screening preoperatively, and identifying delirium postoperatively, in a busy, volume-driving clinical setting.
Purpose
The primary objective of this study was to implement a validated risk assessment tool, the Cleveland Clinic Confusion Score (CCCS) (14), in the preoperative elective orthopedic surgery workflow and couple it with a hospital nursing screening tool, to establish the feasibility of identifying a subgroup more likely to develop POD.
Methods
The hospital Institutional Review Board approved the study and the informed consent. Elective hip and knee orthopedic surgery patients 50 years of age or older were consented during their preoperative visit (within 30 days of surgery) and administered the CCCS. The CCCS ranges from 0 to 7, with higher values indicating greater risk of POD. The CCCS includes age, prior history of delirium, self-reported impact cymbalta cost of alcohol use, preoperative narcotic use, type of surgery (neurosurgery, specifically, adds to the risk score), and baseline cognition measured by a proprietary cognitive test called the Telephone Interview for Cognitive Status (TICS) (15). Internal funding was utilized to purchase rights to use the TICS and for the time of the research nurses.
The CCCS was validated previously by Litaker et al. (14) in a general medicine/surgery population. A cutoff of ≥2 points was found to have a sensitivity of 74% and specificity of 74% for stratifying risk of POD, and outperformed the Brigham and Women’s clomid ovulation Delirium (BWD) scoring system in the studied population (14). This 2-point threshold was used to assign patients in this study a preoperative positive (≥2 points) or negative (<2) screen for POD.
When the patient was admitted to the regular orthopedic nursing floor after surgery, the orthopedic nurses used the Nursing Delirium Screening Scale (Nu-DESC) (16) twice daily to screen for delirium. The Nu-DESC is a validated, delirium assessment tool with sensitivity of 85.7% and specificity of 86.8% (16). We chose the Nu-DESC because the limited data available comparing screening tools in the post-operative population suggested it had the higher sensitivity and comparable specificity to the Confusion Assessment Method (17). Education of the nurses, linkage to a care pathway, and verification of compliance and accuracy was completed prior to study initiation. Although in a clinical setting the Nu-DESC alone might be used to identify delirium, we established a practical definition of delirium for this study in an effort to capture delirium that may have been missed by the Nu-DESC. POD was defined for testing memory more certain.
this study as (1) a positive Nu-DESC result, (2) a retrospective chart review positive for POD, using elements of a validated chart review tool,18 and/or (3) a postoperative phone call to patient or family consistent with POD symptoms.
Study data were collected and managed using REDCap electronic data capture tools hosted at our institution. REDCap (Research Electronic Data Capture) is a secure, web-based application designed to support data capture for research studies (19). Data were analyzed using JMP 9 statistical package (SAS Institute Inc., Cary, NC).
Results
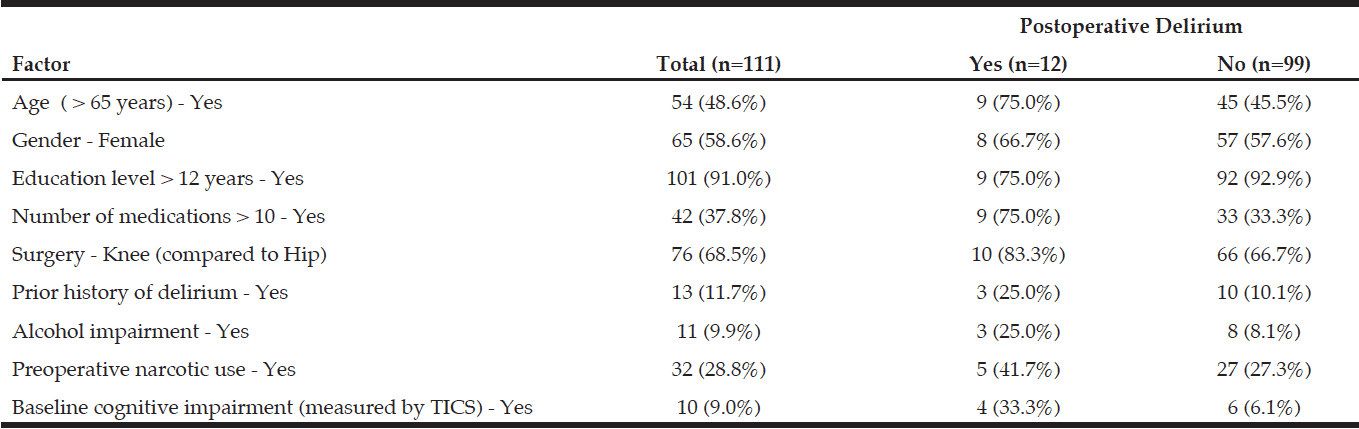
A total of 114 subjects consented and were administered the CCCS preoperatively. Results are presented on those 111 who completed surgery within 30 days. The study cohort (n=111) had a mean age of 65.3 years (range, 50-88 years) and included 65 (58.6%) females. The average education level was 14.7 years (range, 8-23 years) and race was predominantly Caucasian (n=104/111, 93.7%). Knee replacement was the most common surgery performed (n=76, 68.5%). The mean number of medications was 10.3 (range, 1-30). Table 1 presents the frequency of various characteristics for the study population.
A positive CCCS screen was recorded in 31 subjects (27.9%). Of the 111 subjects, 12 (10.8%) developed POD after elective orthopedic surgery. Ten of these subjects were captured by a positive Nu-DESC, and 2 additional subjects were captured by questioning family members about hospital confusion in the post-discharge phone call. Chart review of physician, advance practice, nursing, and therapy notes did not capture any confusion missed by the Nu-DESC. One subject had a positive Nu-DESC but no confusion was suggested in the clinical notes or the phone call. Comparison of the POD and non-delirium groups showed more individuals in the POD group: were at least 65 years old, reported use of more than10 medications, reported prior delirium, tested positive for potential alcoholism, reported preoperative narcotic use, and had baseline cognitive impairment (as measured by TICS) (Table 1).
Result values are expressed as number of cases ( percentage of column header population in parentheses)
The statistical performance of the CCCS as a preoperative tool for predicting delirium after orthopedic surgery is presented in Table 2. The sensitivity and specificity of the assessment were 75% and 78%, respectively. Given the positive predictive value of 29%, a positive preoperative CCCS result was poor at confirming the presence of POD after elective orthopedic surgery. However, a negative preoperative CCCS result had very good predictive accuracy in identifying those patients who will not have POD (negative predictive value = 96%).
PPV, positive predictive value; NPV, negative predictive value
Discussion
This prospective, observational cohort study demonstrated that the CCCS performed as well in this elective orthopedic surgery cohort as it did in the previously reported general surgery cohort. With a relatively high sensitivity, the CCCS risk stratification correctly identifies a majority of the positive POD cases (~3 out of 4). Acknowledging the small positive predictive value, the preoperative CCCS assessment accurately distinguishes a subgroup of older adults at low risk for delirium following elective hip and knee surgery. Identifying a low-risk group has important clinical applications as it may allow the clinical care team to focus intense, even individualized, perioperative interventions on a smaller subset of patients and more efficiently allocate resources (including medical resources and personnel). Additionally, if perioperative pharmacological interventions with some risk are considered, then individuals at low risk for POD could be excluded from these interventions.
The definition of POD in this study was designed to be both clinical and accurate. It is possible that the one patient identified by the Nu-DESC as positive, but not confirmed by phone call or clinical notes, did not have POD. On the other hand, there was clearly a behavior change that triggered the scale that required some clinician attention. Of interest, 2 patients were identified post-discharge with confusion that were not identified at all during the hospitalization by nursing, advanced practitioners or physician personnel. It is possible that this lack of diagnosis may be present in other medical and surgical settings, and reflects the difficulty of detecting POD. Screening tests for delirium are most likely to miss hypoactive delirium, in particular. Inclusion of these patients with post-discharge confusion into the definition makes it difficult to compare the rate of delirium in this study with other studies, but may improve the accuracy of our ability to detect POD, particularly hypoactive delirium.
In addition to cymbaltaonline-pharmacy noting the predictive performance of the CCCS screen, it is important to acknowledge that it was easily implemented into the preoperative clinical workflow, and its use was not complicated. It is even possible to implement an automated version of the CCCS because the score utilizes information that can be programmed and answered directly by patients via electronic data entry.
Our results demonstrate that preoperative screening using the CCCS identifies a subset of patients at higher risk of POD after orthopedic surgery. Future studies of intensive intervention programs and strategies designed to reduce the development or minimize the symptoms of POD can focus on this group. Perioperative clinicians are in a key position to both design and implement these studies.
Acknowledgments: Rebecca Lieberman, BA for assistance with data acquisition; Gloria Hinkle, RN, BSN for assistance with data acquisition; Lydia Boother, MSN, CNS, RN, BSN for assistance with data acquisition and nursing education.
Funding: Internal funding was used to purchase the Telephone Interview for Cognitive Status, which is proprietary
Conflict of interest: No relevant conflicts of interest.
Ethical standards: No ethical issues.
Cutoff: 2+ points Sensitivity 74%, Specificity 74% (14)
Comments:
Prior history of delirium: historical (from chart, patient, or family)
Alcohol impairment: CAGE- this is an acronym of the following 4 questions which comprise a validated screen for impairment from alcohol:
1. Have you ever felt you needed to Cut down on your drinking?
2. Have people Annoyed you by criticizing your drinking?
3. Have you ever felt Guilty about drinking?
4. Have you ever felt you needed a drink first thing in the morning (Eye-opener) to steady your nerves or to get rid of a hangover?
TICS: Telephone Interview for Cognitive Status. This is a proprietary screening test.
References
1. Bruce AJ, Ritchie CW, Blizard R, Lai R, Raven P. The incidence of delirium associated with orthopedic surgery: a meta-analytic review. Int Psychogeriatr. Apr 2007;19(2):197-214.
2. Leslie DL, Marcantonio ER, Zhang Y, Leo-Summers L, Inouye SK. One-year health care costs associated with delirium in the elderly population. Archives of Internal Medicine. Jan 14 2008;168(1):27-32.
3. Marcantonio ER, Flacker JM, Michaels M, Resnick NM. Delirium is independently associated with poor functional recovery after hip fracture. Journal of the American Geriatrics Society. 2000;48(6):618-624.
4. McCusker J, Cole MG, Dendukuri N, Belzile E. Does delirium increase hospital stay? J Am Geriatr Soc. Nov 2003;51(11):1539-1546.
5. Fong TG, Jones RN, Shi P, et al. Delirium accelerates cognitive decline in Alzheimer disease. Neurology. 2009;72(18):1570-1575.
6. Trzepacz P, van der Mast R. Neuropathophysiology of delirium. In: Lindesay J, Rockwood K, MacDonald A, eds. Delirium in old age. New York: Oxford University Press; 2002:51-100.
7. Inouye SK, Westendorp RG, Saczynski JS. Delirium in elderly people. Lancet. Mar 8 2014;383(9920):911-922.
8. Kalisvaart KJ, Vreeswijk R, de Jonghe JF, van der Ploeg T, van Gool WA, Eikelenboom P. Risk factors and prediction of postoperative delirium in elderly hip-surgery patients: implementation and validation of a medical risk factor model. J Am Geriatr Soc. May 2006;54(5):817-822.
9. Inouye SK, Bogardus ST, Jr., Charpentier PA, et al. A multicomponent intervention to prevent delirium in hospitalized older patients. New England Journal of Medicine. 1999;340(9):669-676.
10. Marcantonio ER, Flacker JM, Wright RJ, Resnick NM. Reducing delirium after hip fracture: a randomized trial. Journal of the American Geriatrics Society. 2001;49(5):516-522.
11. Kalisvaart KJ, de Jonghe JF, Bogaards MJ, et al. Haloperidol prophylaxis for elderly hip-surgery patients at risk for delirium: a randomized placebo-controlled study. J Am Geriatr Soc. Oct 2005;53(10):1658-1666.
12. Prakanrattana U, Prapaitrakool S. Efficacy of risperidone for prevention of postoperative delirium in cardiac surgery. Anaesth Intensive Care. Oct 2007;35(5):714-719.
13. Larsen KA, Kelly SE, Stern TA, et al. Administration of olanzapine to prevent postoperative delirium in elderly joint-replacement patients: a randomized, controlled trial. Psychosomatics. Sep-Oct 2010;51(5):409-418.
14. Litaker D, Locala J, Franco K, Bronson DL, Tannous Z. Preoperative risk factors for postoperative delirium. General Hospital Psychiatry. 2001;23(2):84-89.
15. Brandt J, Spencer M, Folstein M. The telephone interview for cognitive status. . Neuropsychiatry Neuropsychol Behav Neurol. 1988;1:111–117.
16. Gaudreau JD, Gagnon P, Harel F, Tremblay A, Roy MA. Fast, systematic, and continuous delirium assessment in hospitalized patients: the nursing delirium screening scale. J Pain Symptom Manage. Apr 2005;29(4):368-375.
17. Radtke FM, Franck M, Schust S, et al. A comparison of three scores to screen for delirium on the surgical ward. World J Surg. Mar 2010;34(3):487-494.
18. Inouye SK, Leo-Summers L, Zhang Y, Bogardus ST, Jr., Leslie DL, Agostini JV. A chart-based method for identification of delirium: validation compared with interviewer ratings using the confusion assessment method. J Am Geriatr Soc. Feb 2005;53(2):312-318.
19. Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG. Research electronic data capture (REDCap)–a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. Apr 2009;42(2):377-381.