E.R. Tuttiett1, B.M. Corfe2, E.A. Williams1
1. Department of Oncology and Metabolism, The Medical School, The University of Sheffield, Sheffield, S10 2RX, England; 2. Human Nutrition Research Centre, Faculty of Medical Sciences, Population Health Sciences Institute, Newcastle University, Newcastle NE2 4HH, UK
Corresponding Author: Esme Tuttiett, University of Sheffield Medical School, Beech Hill Road, S10 2RX, email: ertuttiett1@sheffield.ac.uk, ORCID ID: https://orcid.org/0000-0002-7591-4099, phone: 0114 222 5522
J Aging Res & Lifestyle 2021;10:50-53
Published online September 23, 2021, http://dx.doi.org/10.14283/jarlife.2021.9
Abstract
The lockdown restrictions imposed as a result of COVID-19 impacted on many areas of daily life including dietary behaviours. A cohort of middle-older age adults (n=17), who had previously provided 3-day food diaries in May 2019 were asked to record their 3 day dietary intake in May 2020 when the UK was under lockdown restrictions. Mean (SD) energy intakes were significantly higher by ~750kilojoules in 2020 (8587kJ (1466.9)) compared to 2019 (7837 kJ (1388.9)). This energy increase is equivalent to ~170kcal; approximately 2 slices of bread. Furthermore, recorded meat/meat products, riboflavin, vitamin B6/B12 and iron intakes were all greater in 2020. No other dietary differences were observed between the two timepoints. This was a small, homogenous but well controlled sample, who exhibited a relatively stable diet during lockdown compared with pre-pandemic intakes 12 months earlier. It can be concluded that there was little evidence of food insecurity in this cohort.
Key words: COVID-19, lockdown, diet, food groups.
Introduction
In December 2019, a novel coronavirus (COVID-19), induced by the SARS-CoV-2, emerged. Following its rapid spread, a global pandemic was announced by the World Health Organisation on 11th March 2020 (1) and resulted in a UK national lockdown on 23rd March 2020 (2). Lockdown restrictions consequentially led to lifestyle modifications, including disrupting eating habits, leading to research being undertaken to investigate such changes (3–8).
A cross-national survey was used to compare food dynamics in 1,732 Chinese and 1,547 U.S. households (4). Similar behaviours were recorded by both nationalities and included favouring online shopping and purchasing extra amounts of food when shopping, so fewer trips to buy groceries needed to be made. On the contrary, responses to web-based surveys revealed differing eating behaviours between Spanish and Greek residents (8). Lower restraint eating was reported in Spain, where lockdown regulations were more stringent.
Themes that have emerged globally in the literature regarding changes in diet include the increase in purchasing of: tinned goods, “comfort” foods/confectionary, and baking ingredients (4, 9, 10). More home cooking, including homemade desserts, has been reported during lockdown, mirrored by a decrease in takeaway and ready meal consumption (4, 9, 10). The impact of pre-pandemic health status (11) and socioeconomic status (4) have been implicated as factors that influence dietary behaviours observed during lockdown periods. It is difficult to decipher a common pattern of dietary habits in relation to health emerging as respondents to surveys have often reported a split array of lifestyle behaviours (12).
The majority of the evidence has used web based food frequency questionnaires or surveys that do not always capture accurate dietary intake due to recall bias and missing food items. Furthermore, pre-pandemic dietary intakes in the same population are lacking. In light of this, it was the aim of this research to re-sample a small group of middle-older aged adults who had reported dietary intake using estimated food diaries exactly 12 months before the 1st UK lockdown (13). This demographic is often understudied and there are growing obesity rates in the middle-older adult age group so assessing dietary habits during the lockdown period is of interest. It was hypothesised that lockdown restrictions would have led to changes in dietary behaviours observed in this cohort.
Materials and Methods
Study population and ethics
Twenty-four healthy participants, aged 50-75, who had provided detailed 3-day food diaries in May–July 2019 as part of an unrelated study (13) were re-contacted in May 2020, during UK-wide COVID-19-lockdown restrictions and invited to provide a further 3-day food diary. Prior permission was obtained from all participants in 2019 to be recontacted. Participants were sent a study information sheet, alongside study documents, and implied consent was assumed if documents were returned.
Ethical approval for this study was granted by the University of Sheffield’s ethics committee (ethical approval number: 034260)
Design
This study was a repeated dietary analysis of a convenience sample. The eligibility criteria utilised in the 2019 study (13) dictated participant characteristics. In 2020, participants could either complete the study documentation electronically, and receive it via email, or in paper-version, and receive the documentation in the post. The protocol for completing the 3-day food diary collection (as described elsewhere, (13)) was replicated from the 2019 sampling. In short, participants were asked to record everything they ate and drank during a 24-hour period on 3 occasions during the same week (Monday, Wednesday and Friday). Participants had received previous training for this methodology and utilised a food portion booklet, containing photographs from the Ministry of Agriculture, Food and Fisheries (MAFF) food atlas (Nelson, 1997) to aid with completing this.
Guidance to aid with the return of study documentation was provided and a follow-up discussion between the researcher and the participants was arranged, via a video/telephone call, to check the data for clarity and to obtain further qualitative information about dietary behaviour habits during lockdown. Following completion of all tasks, participants received a £20 voucher to thank them for their participation.
Data analysis
Food diary data was inputted into Dietplan7 nutritional analysis software (Forestfield Software Ltd). This software was used to generate a full report for each participant, containing averages across the three days for energy, macronutrient and micronutrient data, based on UK Composition of Foods tables (14). The report also classified the data into food groups. All statistical analyses were undertaken using SPSS software (version 26.) Data was checked for normality using the Shapiro-Wilk test. Related-Samples Wilcoxon Signed Rank Test analysis was used to assess differences between 2019 (pre-pandemic) and 2020 (lockdown) dietary intakes. A p-value of <0.05 was used to indicate significance.
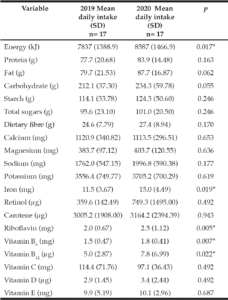
Table 1
Comparison of energy, macro- and micro-nutrient intakes in the study sample (n=17) on two consecutive years; 2019 vs 2020
Data is presented as average mean (SD) values for all participants (n=17.); p-values denoted Wilcoxon analysis using data collected in 2019 compared to data collected in 2020. Significance was set at p=0.05; kJ= kilojoules; g=grams; mg=milligrams, µg=micrograms
Results
Participant Characteristics
All twenty-four original participants were contacted; twenty agreed to provide a further food diary and four did not respond to the follow up email. One participant dropped out of the research due to time limitations. Two participants (both male) were also removed from the analysis, one who displayed irregular eating behaviour, due to shift working, and one for an incomplete food diary, leaving only female participants remaining (n=17). The mean (SD) age and BMI of the included participants was 61.5 (7.4) years and 23.8 (3.8) kg/m2 respectively.
Energy, Macronutrient and Micronutrient Intakes (table 2)
Mean (SD) energy intakes were 9.6% higher in 2020, compared to 2019; 8587kJ (1466.9) vs 7837 kJ (1388.9). No difference was observed in the dietary intakes of protein, carbohydrate and fat at the two timepoints. In 2020, riboflavin, vitamin B6, Vitamin B12 and iron intakes were significantly higher by an average of 0.5mg, 0.3mg, 3.8µg and 3.5mg respectively. No differences were observed in any other micronutrient.
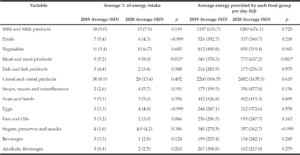
Table 2
Percentage energy provided by food groups, for all participants (n=17), on two consecutive years; 2019 vs 2020
In this table all participant data has been collated together and averages are presented for all 17 participants, based on their food diary recordings. The information demonstrates the average total amount of energy (kJ) consumed by participants in each food group, per day. Further analysis also demonstrates the percentage of energy each food group contributes to overall energy intakes. p-values are Wilcoxon analysis comparing data collected in 2019 to data collected in 2020. Significance was set at p=0.05. kJ= kilojoules.
Food group analysis (table 2)
No differences were observed at a food group level other than for meat and meat products, which significantly contributed more to the average energy provided as a food group in 2020, compared to 2019 (p=0.003).
Discussion
This research investigated dietary intakes both prior to and during lockdown restrictions in a healthy cohort aged 50-71 years. This study revealed, on average, more kilojoules of energy were consumed by participants in May 2020, compared to the previous year. Intakes of riboflavin, vitamins B6 common B12 and iron were greater in 2020 than 2019. These micronutrients are particularly abundant in meat and exploration of the data at a food group level revealed that meat intakes were significantly greater in 2020.
Overall, the dietary data remained fairly stable across 2019 and 2020, in this population. This would suggest that food security was not an issue for the participants, but caution should be paid to the demographic sampled. Survey analysis revealed that the greatest food insecurity were amongst households in the lowest income categories or had family members who had lost income during the pandemic (4). Overall, from the literature, a split picture has emerged in relation to dietary behaviours as a result of lockdown measures (6, 12), and personal circumstances are likely to be an explanation for these disparities (4).
Analysis of food basket data in Spain suggested that energy intakes rose by an average of 6% (15), a similar finding also observed in this sample. Possible explanations for increased energy consumption could be related to greater intakes of nutritionally sparse but energy-dense foods being consumed, often associated with snacking behaviours. Trends of increased consumption of snacks during lockdown, have also been reported by those responding to surveys (11).
Anecdotally, participants in this research reported more home-cooking in 2020. The evening mealtime was described as an event/social occasion, during lockdown, and even referred to as the “highlight of the day” (data not presented). Similarly, it was reported by individuals in Poland that their consumption of homemade meals increased (3), as did U.S. and Chinese citizens (4). Following further investigation of the food diaries to observe the type of food being documented, it was noted that home-cooked meals were often meat-dominated including casseroles and mince-based dishes, such as bolognaise.
The limitations of this study include the small, homogenous sample. This was a convenience based sample, meaning power calculations were not possible. Collection of further demographic and lifestyle information, including physical activity levels, would have made adjustments for confounding variables possible. A critical strength of this research is that the assessments were undertaken on the same individuals at exactly the same time of year. Furthermore, estimated food diaries were obtained, which provide good estimates of energy, nutrient and food intakes. In contrast, a large proportion of research investigating dietary habits during lockdown have relied upon questionnaires and surveys. These are highly subject to recall bias, consequentially deeming them an inadequate method of dietary assessment. This research should be replicated with larger samples who have provided reliable dietary intake information prior to and during lockdown.
Conclusions
• Diet remained generally stable prior to and during lockdown at nutrient and food group level for this small but well controlled population.
• Capturing information from a variety of backgrounds/SES is an important consideration for future work in order to ascertain the overall implications of lockdown on dietary habits.
Disclosure/conflict of interest: No conflicts of interest.
Ethical standards: Ethical approval for this study was granted by the University of Sheffield’s ethics committee (ethical approval number: 034260).
Acknowledgments: The authors would like to thank the Medical Research Council (MRC) and Versus Arthritis for funding this work. Thanks also go to the participants who engaged with this research.
Funding sources: This work was supported by the Medical Research Council (MRC) and Versus Arthritis as part of the Medical Research Council Versus Arthritis Centre for Integrated Research into Musculoskeletal Ageing (CIMA) [MR/R502182/1]. The sponsors had no role in the design and conduct of the study; in the collection, analysis, and interpretation of data; in the preparation of the manuscript; or in the review or approval of the manuscript.
References
1. WHO Director-General’s opening remarks at the media briefing on COVID-19 – 11 March 2020 https://www.who.int/director-general/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19—11-march-2020 Accessed 14 Decemeber 2020
2. Prime Minister’s statement on coronavirus (COVID-19): 23 March 2020 – GOV.UK https://www.gov.uk/government/speeches/pm-address-to-the-nation-on-coronavirus-23-march-2020 Accessed 14 Decemeber 2020
3. Górnicka M, Drywień ME, Zielinska MA, Hamułka J Dietary and Lifestyle Changes During COVID-19 and the Subsequent Lockdowns among Polish Adults: A Cross-Sectional Online Survey PLifeCOVID-19 Study. Nutrients 2020; 12(8):2324.
4. Dou Z, Stefanovski D, Galligan D, Lindem M, Rozin P, Chen T, et al The COVID-19 Pandemic Impacting Household Food Dynamics: A Cross-National Comparison of China and the U.S. SocArXiv (2020) https://osf.io/preprints/socarxiv/64jwy/
5. Di Renzo L, Gualtieri P, Pivari F, Soldati L, Attinà A, Cinelli G, et al Eating habits and lifestyle changes during COVID-19 lockdown: An Italian survey. J Transl Med 2020; 18(1):229.
6. Deschasaux-Tanguy M, Druesne-Pecollo N, Esseddik Y, Szabo de Edelenyi F, Alles B, Andreeva V, et al Diet and physical activity during the COVID-19 lockdown period (March-May 2020): results from the French NutriNet-Sante cohort study. medRxiv. (2020) https://doi.org/10.1101/2020.06.04.20121855
7. Rodríguez-Pérez C, Molina-Montes E, Verardo V, Artacho R, García-Villanova B, Guerra-Hernández EJ, et al Changes in dietary behaviours during the COVID-19 outbreak confinement in the Spanish COVIDiet study. Nutrients 2020; 12(6):1–19.
8. Papandreou C, Arija V, Aretouli E, Tsilidis KK, Bulló M. Comparing eating behaviours, and symptoms of depression and anxiety between Spain and Greece during the COVID-19 outbreak: Cross-sectional analysis of two different confinement strategies. Eur Eat Disord Rev. 2020; 28(6):836–46.
9. Bracale R, Vaccaro CM. Changes in food choice following restrictive measures due to Covid-19. Nutr Metab Cardiovasc Dis. 2020; 30(9):1423–6.
10. McKevitt F. Grocery growth slows and habits change as UK adapts (2020) English – Kantar Worldpanel https://www.kantarworldpanel.com/en/PR/Grocery-growth-slows-and-habits-change-as-nation-adapts. Accessed 14 December 2020.
11. Robinson E, Boyland E, Chisholm A, Harrold J, Maloney NG, Marty L, et al Obesity, eating behavior and physical activity during COVID-19 lockdown: A study of UK adults. Appetite 2021; 10.1016/j.appet.2020.104853
12. British Nutrition Foundation. BNF survey reveals stress, anxiety, tiredness and boredom are the main causes of unhealthy eating habits in lockdown (2020) https://www.nutrition.org.uk/healthyliving/hewathome/lockdownsurvey.html Accessed 14 December 2020
13. Tuttiett ER, Green DJ, Stevenson EJ, Hill TR, Corfe BM, Williams EA. Short-Term Protein Supplementation Does Not Alter Energy Intake, Macronutrient Intake and Appetite in 50–75 Year Old Adults. Nutrients. 2021; 13(5):1711
14. McCance, R. A., Widdowson, E. M., Institute of Food Research (Great Britain), Public Health England,, & Royal Society of Chemistry (Great Britain). (2015). McCance and Widdowson’s the composition of foods.
15. Batlle-Bayer L, Aldaco R, Bala A, Puig R, Laso J, Margallo M, et al Environmental and nutritional impacts of dietary changes in Spain during the COVID-19 lockdown. Sci Total Environ 2020; 748:141410.