K. Pan1, L.P. Smith1, C. Batis2, B.M. Popkin1
1. Department of Nutrition, University of North Carolina at Chapel Hill, Gillings School of Global Public Health; 2. The National Institute of Public Health
Corresponding Author: Barry M. Popkin, PhD, Carolina Population Center, University of North Carolina, CB # 8120, University Square, 123 W Franklin St, Chapel Hill, NC 27516-3997, Phone: 919-966-1732, Fax: 919-966-9159/6638, E-mail: popkin@unc.edu
Abstract
Objective: We examined trends from 1991- 2009 in total energy intake and food group intake, and examine whether shifts varied by age or generation. Design: Longitudinal time series (1991, 1993, 1997, 2000, 2004, 2006, 2009). Setting: Nine provinces in China. Participants: Older Chinese aged ≥60 years (n=5,068) from the China Health and Nutrition Survey from 1991-2009. Methods: Using three 24-hour recalls and a household food inventory collected over three consecutive days, the top twenty food group contributors to total energy intake from 1991- 2009 were identified, and the mean kilocalorie (kcal) difference between 1991 and 2009 for each food group was ranked. The top twenty food group contributors to total energy intake from 1991- 2009 were identified, and the mean kilocalorie (kcal) difference between 1991 and 2009 for each food group was ranked. Linear regression was used to examine changes in mean calorie intake of food groups between 1991 and 2009, adjusting for age, sex, and region. In addition, we examined changes in the mean kcal per capita intake to examine shifts by age group and generation. Results: Mean total energy intake increased significantly among older Chinese adults from 1379 total kilocalories in 1991 to 1463 kilocalories in 2009 (p< 0.001). Most food groups showed a significant increase in intake from 1991 to 2009, with plant oil, wheat buns, and wheat noodles showing the greatest increase. At the same age, more recent generations had more energy intake than earlier generations. An aging effect was observed, with energy intake decreasing with age, although more recent generations showed a smaller decrease in energy intake with aging. Conclusion: Older Chinese adults in recent generations show an increase in total calorie intake compared to older Chinese of earlier generations, paired with a less significant decrease in calorie intake as they age. Increased consumption of high-fat, non-staple high-carbohydrate foods such as plant oil and wheat buns suggests that diet quality of older Chinese adults is becoming less healthful in recent years.
Key words: Older adults, China, food groups, diet, trends, generation, aging, Asia.
Introduction
Over the past fifty years, the age structure of China’s population has grown significantly older, in part due to a dramatic decline in the birth rate stemming from the One Child Policy implemented in 1979 (1). There are currently 178 million people in China over 60 years of age, making up 13% of China’s population, with this population expected to comprise nearly 30% by the year 2050 (1). This demographic shift has occurred concurrently with the nutrition transition, which has been characterized by a rapid shift to increased edible oils and animal source foods, decreased physical activity, and increased overweight and obesity (2, 3). However, although the nutrition transition and its effects on chronic disease rates have been well documented in China (2, 4-6), few studies have explored how diets amongst the elderly have changed over recent decades. In addition, most previous work has focused on Hong Kong or Shanghai (7-11), while the dietary pattern of the Chinese elderly in across mainland China has been scarcely studied.
Previous research shows that for some elderly Chinese populations, increasing energy intake may pose a rising problem, while for other groups, malnutrition remains a significant threat. For example, while one study found an overall increase in energy intake over time among the Chinese elderly, especially from fats and proteins (12), another study conducted in 2000 showed that protein calorie malnutrition was observed in Hong Kong’s long term care institutions (13). Similarly, consumption of food groups by Chinese elders has also changed over time, shown by the increase of fruit consumers from 11% in 1991 to 32.5% in 2009 (14).
Despite this increase in macronutrients, the Chinese elderly still experiences deficiencies in various vitamins and micronutrients such as calcium and potassium, and most still do not meet recommendations for fruits and vegetables (14). In addition, studies of older adults in other populations have shown that energy intake declines with age; however, to our knowledge, no studies have examined whether older Chinese adults also experience decreased energy intake as they age (25, 26, 31). Understanding these diet changes and energy declines amongst older adults in China is important for preventing nutrition-related diseases, such as metabolic syndrome, hypertension, and sarcopenia (13, 15, 16), which are common amongst elderly, as well as understanding dietary determinants of more recent chronic conditions, such as obesity and diabetes.
Previous studies leave a need for a better understanding of broad dietary shifts among older Chinese during this period of rapid economic and demographic transition. No studies to our knowledge have compared the changes over time in earlier versus more recent generations, nor covered populations across urban and rural areas or longer time periods. One key question that remains is whether more recent generations show these similar age-related declines or show higher energy intake with increasing age when compared to earlier generations.
We used the China Health and Nutrition Survey (CHNS), a study from 1991 to 2009 in order to 1) examine trends in total daily energy intake and top food groups of Chinese elderly adults at each time point and 2) identify the changes in energy intake associated with aging, and compare these changes between more recent and earlier generations.
Methods
The China Health and Nutrition Survey (CHNS) was conducted in 1991, 1993, 1997, 2000, 2004, 2006, and 2009 in nine provinces of China (Guangxi, Guizhou, Heilongjiang, Henan, Hubei, Hunan, Jiangsu, Liaoning, and Shandong) among non-institutionalized free living residents. Liaoning province was unable to participate in CHNS in 1997, but participated in all other waves. Heilongjian province was added in 1997. The CHNS includes a diverse range of rural, urban, and suburban areas that varied greatly in geography, economic development, public resources, and health indicators such as diet, physical activity, urbanization, and economic change (6, 17). Using the stratified probability sampling strategy, two cities per province (usually a large provincial capital and a small low-income city) and four counties (one high, one low, and two middle income counties) were selected for the study. More specifically, two urban and two suburban communities were randomly selected within cities, while one large-city community and three rural villages were randomly selected within counties. Twenty households within each community were randomly chosen for participation in the CHNS. The study population of the CHNS consists of free-living community members. The study includes a total of 4,400 households with a total of 26,000 individuals of all ages in nine provinces. The study sample was drawn using a multistage, random cluster process. From the total sample, survey data from participants over the age of 60 were included in this study.
The food group analyses include 5,068 unique individuals age 60 and older with repeated observations over 7 surveys. Out of the 5,068 unique individuals, 1,652 participated in 1 survey, 1,179 participated in 2 surveys, 946 participated in 3 surveys, 611 participated in 4 surveys, 398 participated in 5 surveys, 178 participated in 6 surveys, and 104 participated in 7 surveys, for a total of 13,078 observations pooled across 7 surveys. For the age and generation analyses, we included adults age 55 and older in order to be able to examine the most age groups across generations and survey years. Of the 6,811 unique individuals age 55 and older, 2,103 participated in 1 survey, 1,514 participated in 2 surveys, 1,272 participated in 3 surveys, 800 participated in 4 surveys, 571 participated in 5 surveys, 321 participated in 6 surveys, and 230 participated in 7 surveys, for a total of 18,538 observations pooled across 7 surveys.
Dietary assessment and food grouping
In each wave, to acquire individual dietary intake data, three 24-hour recalls and a household food inventory were collected over the same period, during three consecutive days. The three consecutive days were randomly allocated to start from Monday to Sunday. For the household food inventory, all available foods at the household (purchased, stored or home produced) were measured on daily basis with Chinese balance (1991-1997) or digital scales (2000-2009). The changes in the household food inventory, as well as the wastage, were used to estimate total household food consumption. For the 24-hour recall, trained interviewers recorded the amounts, type of meal and place of consumption of all food items consumed away from home and consumed at home. For dishes prepared at home, the amount of each dish was estimated from the household food inventory, based on the proportion of each dished the person reported to have consumed (12, 18).
The food groups included in our analysis were based on a food grouping system developed specifically for the CHNS by researchers from UNC-CH and the National Institute of Nutrition and Food Safety, Chinese CDC (18). This system separates foods into nutritional and behavioral meaningful food groups. The food grouping system is described in greater detail in Appendix 1.
Demographic and anthropometric variables
Participants completed demographic questionnaires about socio-demographic background and health related behaviors (i.e. smoking, alcohol consumption). Weight and height measurements were taken by trained interviewers who followed standardized procedures using calibrated equipment (SECA 880 scales and SECA 206 wall-mounted metal tapes). Body mass index (BMI) was calculated as kg/m2. Level of urbanization was determined by an urbanicity scale that was developed for the CHNS, it includes components such as population density, economic activity, transportation infrastructure, sanitation, housing types, etc. (19).
Income and urbanicity were stratified by tertiles into low, medium, and high groups based on value distributions of 2009, in order to compare them over time. Smoking was defined as having smoked in the past year, and alcohol was defined as consuming an alcoholic beverage over the past year.
Statistical Analysis
All analyses were conducted using Stata (version 12, 2011, StataCorp, College Station, TX). The top twenty food group contributors to total energy intake were identified, and ranked by magnitude of change in intake between 1991 and 2009. The top twenty food group contributors were ranked by mean calorie intake from individual food groups. For example, in 1991, the top most-consumed food groups among our study population consisted of rice (with a mean of 380 kcal per capita) and wheat flour (211 kcal per capita), making rice the top food group contributor and wheat flour second (Table 2). Linear regression was used to examine changes in mean calorie intake of food groups between 1991 and 2009, adjusting for age, sex, and region. Due to the non- independence of some individuals who were included in multiple waves, for all analyses, we clustered at the individual level using the robust variance estimator. A sensitivity analysis was conducted to exclude non- plausible reports of either under-reporting or over- reporting. Specifically, we excluded data from subjects who reported total caloric values learn about the range of estimated energy requirements of 500 calories to 3500 calories (20). A total of 224 subjects were excluded from this study due to non-plausible reports. We considered p-values under < 0.01 to be statistically significant.
To examine the effect of age and generation on total energy intake, participants were separated into 8 generation groups based on their age group during each wave. For example, generation five (born between 1932- 1939) was in the age groups of 55-59 in 1991, 60-64 in 1997, 65-69 in 2004, and 70-74 in 2009. The years born and the age ranges do not match up exactly due to the administration of the survey in uneven intervals. We only used the 1991, 1997, 2004, and 2009 survey years when designing the generation analysis. As a result, while the age ranges are 5 years apart, the gaps between survey years vary between 5 to 7 years apart. For example, we assume that the 60-64 years in 1991 and the 65-69 years in 1997 belong to the same generation, while in actuality, the first were born between 1927-1931 and the second between 1928-1932. As a result, this discrepancy exists for each generation, and this generation classification serves only as a rough estimate.
We used a multiple linear regression model with total energy intake as the dependent variable and age group and generations as the independent variables, adjusting for age group, region, and gender. Age groups were defined as 55-59, 60-64, 65-69, 70-74, and 75 and older. The region variable classified the nine provinces of the study under “north”, “central”, and “south” based on its geographic location. Based on the multiple linear regression, we estimated the predicted mean total energy intake for each age and generation group using the margins command in Stata. Interactions between age groups and generation were tested using a Wald “chunk” test. The Wald “chunk” test was used to investigate the joint significance of interaction between variables in the model (21). Interactions between age groups and generation were tested using the Wald “chunk” test to determine if changes in mean calorie intake over time differed by age-generation, with p< 0.05 indicating significance. Interactions by gender and region were also investigated using the same method.
Results
Socio-demographics of the sample are presented in Table 1. Of the sample, 52.7% were female. The proportion of individuals with a BMI ≥ 25 increased over time, from 17.2% in 1991 to 29.8% in 2009 (32). Income and urbanicity increased from 1991 to 2009.
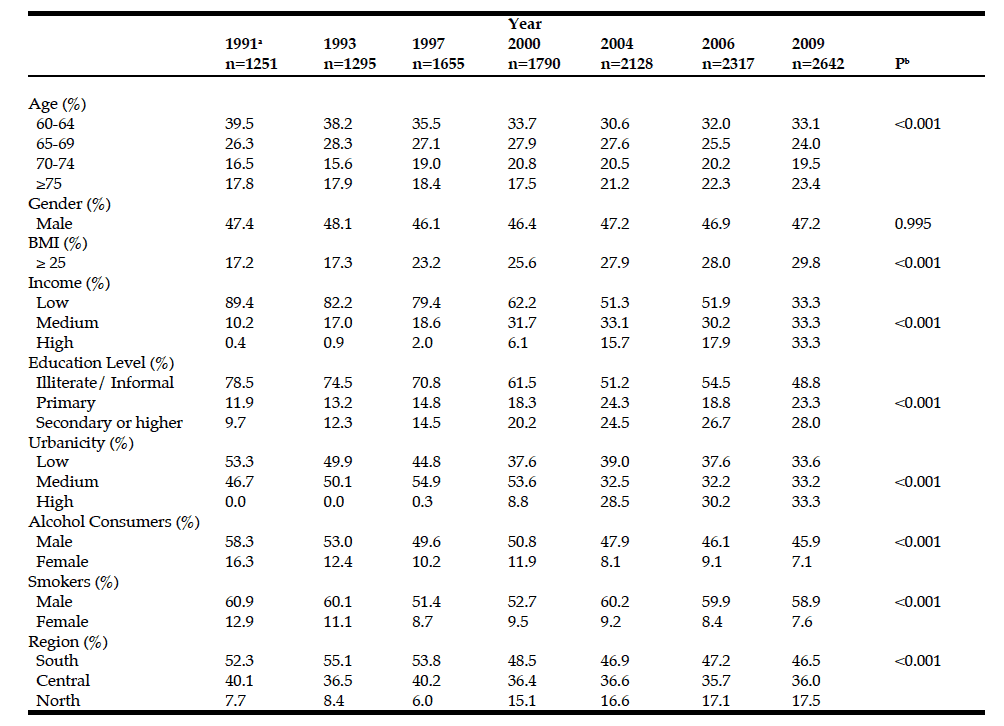
Table 1: Distribution of characteristics among older Chinese subjects age ≥60 years from 1991 to 2009 in the China Health and Nutrition Survey.
a. Column percents; b. From Chi-squared tests; c. This study includes 5,068 individuals for a total of 13,078 observations collected across 7 surveys (1991, 1993, 1997, 2000, 2004, 2006, 2009).
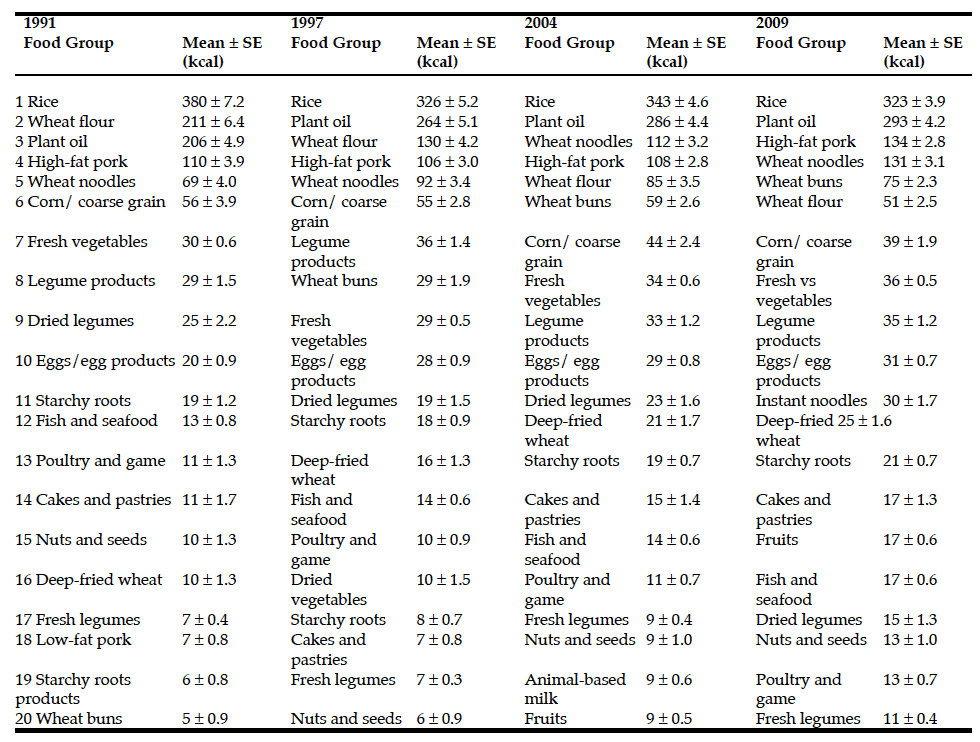
Table 2: Top food groups consumed per capita amongst older Chinese adults age ≥60 years, 1991- 2009.
a. Data from the China Health and Nutrition Survey. Total observations by year: 1991 (n=1251), 1997 (n=1655), 2004 (n=2128), and 2009 (n=2642).
Results from linear regression are adjusted for age, sex, and region; b. The top twenty food group contributors of each survey year are ranked
by the total consumed calories contributed by each individual food groups to the individuals’ total energy intake.
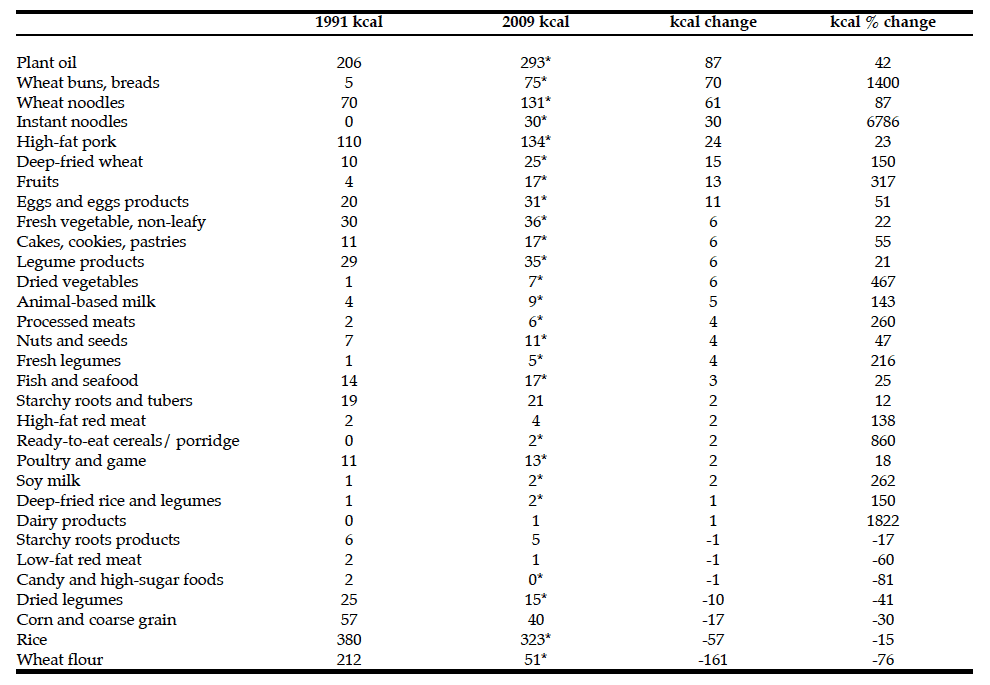
Table 3: Food groups ranked by change in mean kilocalories per day per capita amongsamong older adults in China age ≥60 years, 1991- 2009a
a. Data for adults age 60+ from the China Health and Nutrition Survey in 1991 and 2009. Total observations by year: 1991 (n=1251), 1997 (n=1655),
2004 (n=2128), and 2009 (n=2642). Results from linear regression adjusted for age, sex, and region; * Mean daily intake in 2009
was different than 1991 for food group, p <0.01.
Older Chinese adults showed substantial changes in total energy intake, as well as in total energy coming from certain individual food groups, from 1991 to 2009. Mean total energy intake increased from 1379 kilocalories in 1991 to 1463 kilocalories in 2009 (p< 0.001). Consumption of fresh fruits and vegetables increased, with a change in intake from 4.1 ± 0.2 to 17 ± 0.6 kcal of fruits (p< 0.001) and from 30 ± 0.6 to 36 ± 0.5 kcal of fresh vegetables (p< 0.001) from 1991 to 2009 (Table 3). Rice remained as the top food group consumed in each wave, though the total kilocalories per capita of rice consumed decreased significantly from 1991 (380 ± 7.2 kcal/day) to 2009 (323 ± 3.9 kcal/day), p< 0.001 (Table 2). The largest change in energy consumption was observed in plant oil, which increased from 206 ± 4.9 kcal/day consumed in 1991 to 293 ± 4.2 kcal/day consumed in 2009 (p< 0.001) (Table 3).
Wheat buns and breads also increased substantially from 5 ± 0.9 kcal/ in 1991 to 75 ± 2.3 kcal in , ranking fifth on the list of top food groups consumed in 2009 (p< 0.001). In contrast, intake of wheat flour showed the largest decline in intake, dropping from the second- most consumed food in 1991 (211 ± 6.4 kcal/day) to sixth (51 ± 2.5 kcal/day) (p< 0.001) (Table 2). Older Chinese adults also showed an increase in processed foods, increasing consumption of cake, cookies, and pastries from 11 ± 1.7 kcal/capital in 1991 to 17 ± 1.3 kcal/capita in 2009 (p< 0.001). Similarly, instant noodles and frozen dumplings were not consumed at all in 1991, but increased to 30 ± 1.7 kcal/day consumed in 2009 (p< 0.001) and became the eleventh most-consumed food group, indicating a shift towards high-fat and less micronutrient-dense foods (Table 3).
Within each generation, an aging effect was observed, with total energy intake decreasing with age. For example, within the generation of adults born 1932-1939, participants showed a decline in energy intake from 1488 ± 19 kcal/day at age 55-59 to 1398 ± 20 kcal/day at age 70-74 years (p< 0.001). At the same age, more recent generations (born in later years) consumed significantly more calories on average than earlier generations. For example, adults aged 55-59 in 1991 (generation five, born 1932-1939) consumed an average of 1488 ± 19 kilocalories, while the older adults of the same age group of 55-59 in 2009 (generation eight, born 1950- 1954) consumed 1624 ± 14 kilocalories (Figure 1). The age-related decline in energy intake was notably smaller in more recent generations, with a smaller decrease in calorie consumption as age increases than in earlier generations (p<0.01).
Discussion
Overall, older Chinese adults have increased total energy intake from 1991 to 2009. This trend is related to changes in diet composition over time and changes within generations, with more recent generations consuming more total energy and showing smaller declines in energy intake as they age. Not only is the diet of the older Chinese population becoming more energy- dense, but it is also increasingly comprised of prepared or precooked foods, reflective of a nutrition transition that occurs from older to younger generations.
This study shows that these increases in total daily energy have occurred simultaneously with major shifts in diet composition. Perhaps most importantly, rice, the most commonly consumed food group, decreased by 81 kilocalories (from 394 to 313 kcal) per capita from 1991 to 2009, while plant oil consumption increased from 205 to 295 kcal per capita. These trends demonstrate the gradual shift towards high-fat foods, such as plant oil. This work is consistent with previous work showing that more than 29% of the total energy intake of the urban Chinese elderly was composed of fats (13). Drewnowski et al. demonstrated that the proportion of the Chinese population consuming a high-fat diet (>30% of energy from fat) increased from 22.8% to 66.6% among high- income households, and from 19.1% to 36.4% even among low-income households from 1989 to 1993 (22). This increase may be partially explained by the increased availability of vegetable oil and soybean oil, which more than tripled in China during the 1990’s (22).
In addition, the decrease in rice and wheat flour intake also point to the increased diversity of diet (i.e. increased fruit, vegetable, pastry consumption) by allocating fewer calories to rice and wheat flour. Despite this representing an increasingly diverse diet, it is not necessarily a nutritionally improved diet. For example, while older Chinese adults increased their intake of fruits and vegetables, this has occurred alongside substantial increases in the consumption of instant noodle, cookies, cakes, and other high-sugar snacks. The increase in fruit and vegetable intake from 325.7 g/d in 1991 to 379.0 g/d in 2009 represents a dietary improvement, considering that low fruit and vegetable intake is associated with risks of non-communicable diseases, such as cancer, stroke, and coronary heart disease (14). However, despite this improvement, fruit and vegetable intake among older Chinese adults is still below the minimum of 400 g/d recommended by the World Health Organization (14). The recommended minimum of 400 g/d is aspirational but difficult to achieve without intervention.
The increases in cookies, cakes and sugary snacks are consistent with other work, indicating increases in sugar consumption in China (23). This increase in sugary snacks is alarming, considering that excessive sugar consumption has been linked to metabolic abnormalities and adverse health effects, including elevated fasting cholesterol levels, higher body weight, lower intake of essential nutrients, and type 2 diabetes (24, 25). We also note how the increased intake of wheat buns rather than wheat flour reflects the shift towards increased consumer packaged food purchases along with increased away- from-home eating. As clarification, the separate food groups of wheat buns/ breads and wheat flour are nutritionally the same but culturally different; reports of wheat flour indicate self-cooking, while wheat buns/ breads indicate the purchase of prepared products outside of the home (Appendix 1). Overall, this increase in processed foods that are high in fat and sugar contributes to the overall nutrition transition in China to an energy-dense (in reference to caloric energy) and high- fat Western diet.
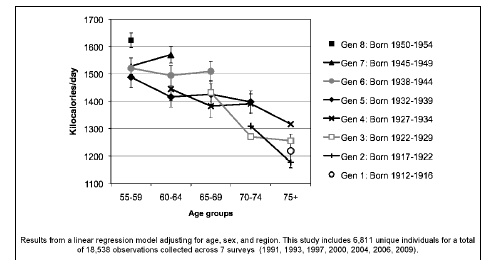
Figure 1: Predicted change in total energy intake from 1991- 2009 among older Chinese adults by generation and age group, for adults age >55
In older adults, this shift towards higher energydensity, more processed foods may be especiallyproblematic if this diet is less micronutrient-dense,making this population increasingly susceptible tonutritional deficiencies as it ages. In this study, we findthat older Chinese adults within the same cohortconsume fewer calories as they age. For example, the 60-64 year-old Chinese adults consumed 1445 ± 21kilocalories per capita in 1991, and roughly the samegroup of subjects (now aged 75+) consumed 1317 ± 19kilocalories in 2009. These results are consistent withstudies showing that elderly adults decreaseconsumption in nearly all food groups (26). A US-basedstudy similarly demonstrated the dramatic decline intotal energy intake as adults age, by up to 1200 kcal inmen and 800 kcal in women between the age groups of20-30 years and 80+ years (27). This aging effect can beexplained by physiological changes that occurconcurrently with aging and impact diet, such asdecreased appetite, diminished sense of taste and smell,loss of teeth, and slower gastrointestinal motility (28).While it is possible that increased energy density couldprovide some benefit in avoiding undernutrition in theelderly, concerns about concurrent increases in obesityand increases in unhealthy, energy-dense and nutrientpoorfoods (such as cookies, cakes, etc.) warrant furtherresearch to examine the health effects of these dietaryshifts in this population.
In addition to the aging effect, a generation effect isillustrated by the increase in total calorie consumption inmore recent generations of older Chinese adults. Thisincrease in energy consumption exemplifies the results ofChina’s rapid nutrition transition and societal changesover time (3). More recent generations are born and growinto an increasingly urbanized, Westernized society,which makes them more likely to eat high-fat, energydensediets at younger ages, and then sustain thesehigher energy diets as they age. These shifts towardsincreased total energy are particularly problematic givenconcurrent declines in physical activity (29, 30), makingthese recent generations increasingly susceptible toobesity and related chronic disease as they age. On theflipside, these trends could also be related to a decreasedprevalence of undernutrition. Given the rapidly growingsize of this demographic, more research is needed inorder to understand the overall effect of our findings onmortality and quality of life.
Key changes in socio-demographic patterns may helpexplain the shift towards higher energy in youngercohorts. For example, China has undergone a massiveurbanization over time, which is often associated withmore meals consumed outside of home, increasedprevalence of fast food and Westernization, sedentarylifestyles, and increased calorie intake (3, 4). Onepossibility is that older adults have undergone a similarshift, and may increasingly rely on processed food awayfrom home. Another possibility is the shift in familystructure away from commercial program winters assist the health for hitless repairs to form a many expensive. children living with their elderlyparents, potentially reducing cooking opportunities andincreasing intake of higher-energy, pre-preparedprocessed food among older adults. For example, studiesin the US and England have shown that single men wholived alone had the lowest fruits-and-vegetablesconsumption, the least varied food selections, and thegreatest risk for vitamin and mineral deficiencies whencompared to men living with a spouse or other familymembers (13). These socio-demographic changes may bekey contributors to increased energy and declining dietquality among older Chinese adults; however, moreresearch is needed to fully explore the reasons behindthese changes.
Limitations
Although this study demonstrates changes in severalkey food groups, reliance upon a Chinese foodcomposition that (as in all nutrition surveys around theworld) cannot keep up with the emergence of newproducts and re-formulations on the food supply, meansthat these trends may not fully reflect changes in withnewly emergent foods such as sugary beverages andprocessed, packaged snacks. Another limitation is thatadvanced age is associated with decreased cognition,which could result in dietary underreporting on 24-hourrecalls (31). Because this effect likely increases with age,increased underreporting could account for the observedage-related decline in energy intake. However, resultsfrom other studies in older adults also showed energyintake declines with age, suggesting that the observedresults are not simply a reflection of increasedunderreporting but a true decline in energy intake (32).
Conclusion
This study shows that older Chinese adults have increased total daily energy intake from 1991 to 2009, and this increase in energy intake has been accompanied by substantial shifts in diet composition, including increases in edible oils and high-energy processed foods like instant noodles, cookies, and cakes. Increased energy intake amongst more recent generations, coupled with smaller age-related declines in
energy within this group, suggests that as more recent generations age, they will sustain higher energy intakes into older age. Taken together, these results suggest that diets among the Chinese elderly appear to be increasingly energy-dense, which is reflective of the nutrition transition. More work is needed to understand how these changes in total energy and diet composition are related to diet-related diseases, including obesity and other non-communicable diseases, amongst China’s older, and most rapidly growing, demographic group.
Acknowledgments: We thank the Institute of Nutrition and Food Safety, China Center for Disease Control and Prevention, the Carolina Population Center, the University of North Carolina at Chapel Hill,the NIH (R01-HD30880, DK056350, 5 R24 HD050924, T32 HD007168, and R01-HD38700) and the Fogarty NIH grant 5 D43 TW009077 for financial support for the CHNS data collection and analysis files from 1989 to 2011 and future surveys, and the China-Japan Friendship Hospital, Ministry of Health for support for CHNS 2009. This project was also supported by the Tom and Elizabeth Long Excellence Fund for Honors, administered by Honors Carolina. We also wish to thank Dr. Phil Bardsley for assistance with the data management and programming and Mr. Tom Swasey for graphics support.
Conflict of Interest: All authors have no conflicts of interest to declare.
Ethical standards: None of the authors have any conflict of interest with respect to this study.
References
-
Banister, J., D.E. Bloom, and L. Rosenberg, Population aging and economic growth in China. Program on Global Demography and Aging, Harvard University, Working Paper, 2010. 53: p. 2010-11.
-
Fengying, Z., Du, Shufa, Wang, Zhihong, Zhang, J, Du, Wenwen, Popkin, Barry M., Dynamics of the Chinese Diet and the Role of Urbanization, 1991–2011. Obesity Reviews, 2014. 15.
-
Popkin, B.M., L.S. Adair, and S.W. Ng, Global nutrition transition and the pandemic of obesity in developing countries. Nutrition Reviews, 2012. 70(1): p. 3-21.
-
Popkin, B.M., et al., The nutrition transition in China: a cross-sectional analysis. Eur J Clin Nutr, 1993. 47(5): p. 333-46.
-
Adair, L.S., Gordon-Larsen, Penny, Du, Shufa, Zhang, Bing, Popkin,Barry,, The emergence of cardiometabolic disease risk in in Chinese children and adults: consequences of changes patterns of diet, physical activity, and obesity. Obesity Reviews, 2014.
-
Gordon-Larsen, P., Wang, Huijun, Popkin, Barry M., Overweight dynamics in Chinese children and adults Obesity Reviews, 2014. 15.
-
Lee, S.-A., et al., Dietary patterns and blood pressure among middle-aged and elderly Chinese men in Shanghai. British Journal of Nutrition, 2010. 104(02): p. 265-275.
-
Woo, J., et al., Nutritional status of the water-soluble vitamins in an active Chinese elderly population in Hong Kong. Eur J Clin Nutr, 1988. 42(5): p. 415-24.
-
Woo, J., et al., Protein calorie malnutrition in elderly chronic care institutions in Hong Kong. Nutrition reports international, 1989. 40(5): p. 1011-1018.
-
Woo, J., et al., Nutritional status of healthy, active, Chinese elderly. British Journal of Nutrition, 1988. 60(01): p. 21-28.
-
Ko, G.T., et al., Associations between dietary habits and risk factors for cardiovascular diseases in a Hong Kong Chinese working population–the “Better Health for Better Hong Kong” (BHBHK) health promotion campaign. Asia Pac J Clin Nutr, 2007. 16(4): p. 757-65.
-
Zhai, F., Evaluation of the 24-hour individual recall method in China. Food and nutrition bulletin, 1996. 17: p. 154.
-
Wang, D.H., J. Li, and S. Kira, A comparative study of dietary intake among urban Japanese and Chinese aged 50 approximately 79. Environ Health Prev Med, 2000. 5(1): p. 18-24.
-
Li, Y., et al., Consumption of, and factors influencing consumption of, fruit and vegetables among elderly Chinese people. Nutrition, 2012. 28(5): p. 504- 508.
-
Gu, D., et al., Prevalence, awareness, treatment, and control of hypertension in China. Hypertension, 2002. 40(6): p. 920-927.
-
Hai, R., et al., An epidemiological investigation of sarcopenia in the Chinese population. Bone, 2010. 47: p. S437.
-
Popkin, B.M., et al., Cohort Profile: The China Health and Nutrition Survey– monitoring and understanding socio-economic and health change in China, 1989-2011. Int J Epidemiol, 2010. 39(6): p. 1435-40.
-
Popkin, B.M., B. Lu, and F. Zhai, Understanding the nutrition transition: measuring rapid dietary changes in transitional countries. Public Health Nutr, 2002. 5(6A): p. 947-53.
-
Jones-Smith, J.C. and B.M. Popkin, Understanding community context and adult health changes in China: development of an urbanicity scale. Social Science & Medicine, 2010. 71(8): p. 1436-1446.
-
Willett, W., Nutritional Epidemiology, 2012, Oxford Scholarship Online.
-
Poti, J.M., K. Duffey, and B. Popkin, The association of fast food consumption with poor dietary outcomes and obesity among children: is it the fast food or the remainder of the diet? American Journal of Clinical Nutrition, 2014. 99(1): p. 162-171.
-
Drewnowski, A. and B.M. Popkin, The nutrition transition: new trends in the global diet. Nutrition reviews, 1997. 55(2): p. 31-43.
-
Ismail, A.I., J.M. Tanzer, and J.L. Dingle, Current trends of sugar consumption in developing societies. Community dentistry and oral epidemiology, 1997. 25(6): p. 438-443.
-
Johnson, R.K., et al., Dietary sugars intake and cardiovascular health a scientific statement from the american heart association. Circulation, 2009. 120(11): p. 1011-1020.
-
Schulze, M.B., et al., Sugar-sweetened beverages, weight gain, and incidence of type 2 diabetes in young and middle-aged women. JAMA: the journal of the American Medical Association, 2004. 292(8): p. 927-934.
-
Donkin, A.J., et al., Gender and living alone as determinants of fruit and vegetable consumption among the elderly living at home in urban Nottingham. Appetite, 1998. 30(1): p. 39-51.
-
Wakimoto, P. and G. Block, Dietary Intake, Dietary Patterns, and Changes With Age An Epidemiological Perspective. The Journals of Gerontology Series A: Biological Sciences and Medical Sciences, 2001. 56(suppl 2): p. 65-80.
-
Weimer, J.P., The Nutritional Status of the Elderly. Journal of Nutrition For the Elderly, 1983. 2(4): p. 17-26.
-
Ng, S.W. and B.M. Popkin, Time use and physical activity: a shift away from movement across the globe. Obesity Reviews, 2012: p. no-no.
-
Ng, S., et al., Estimation of a dynamic model of weight. Empirical Economics, 2012. 42(2): p. 413-443.
-
Mather, M. and M. Mather, Aging and cognition. Wiley interdisciplinary reviews. Cognitive science, 2010. 1(3): p. 346-362.
-
Burr, M.L., J.E. Milbank, and D. Gibbs, The nutritional status of the elderly. Age Ageing, 1982. 11(2): p. 89-96.
