C. Jeandel1, T. Hanh2
1. Département de Gériatrie; CHU de Montpellier 34295 cedex. Université de Montpellier; 2. nutritionist doctor, Paris
Corresponding Author: Claude Jeandel, Département de Gériatrie. CHU de Montpellier 34295 cedex. Université de Montpellier, c-jeandel@chu-montpellier.fr
J Aging Res & Lifestyle 2022;11:26-30
Published online July 8, 2022, http://dx.doi.org/10.14283/jarlife.2022.5
Abstract
Background: No investigation has assessed frailty in the clinical setting of thermal/spa facilities, which often receive older patients with osteo-articular and musculoskeletal conditions. Objective: To examine the prevalence of frailty in older adults receiving thermal/spa treatment and to gather preliminary evidence about the feasibility of integrating geriatric assessments, including frailty, in the routine clinical consultations in spa facilities. Methods: Mixed design, with a quantitative cross-sectional investigation performed among 197 volunteer patients (mean age 73.2 ± 6.4 years-old; 82.2% women) of seven French thermal/spa facilities and a qualitative investigation (semi-structured interviews) with the nine physicians working in the participating facilities. Frailty was defined according to a modified Fried frailty phenotype based on six self-reported criteria (including mobility impairment, nutritional status, and fatigue): individuals meeting ≥3 criteria were considered frail; 1-2 criteria, pre-frail; no criterion, robust. Interviews with the participating physicians on the feasibility of integrating geriatric assessments in routine clinical consultations at spa facilities were recorded and their content, analyzed. Results: Frailty was detected in 112 individuals (56.9%), 26 (13.2%) were considered pre-frail, and 59 (29.9%), robust. Regarding the interviews, three physicians indicated the geriatric assessments could be integrated in the routine spa consultations; two, in the consultations of specific/targeted patients, but not in routine; two, only in the context of health education; two, in the context of research protocols. The content of interviews highlighted geriatric assessments provided a better overview of the health/clinical status of the patients. Conclusion: Frailty is very prevalent in older patients of spa facilities. Such facilities may constitute an interesting clinical setting for screening for frailty through the implementation of geriatric assessments.
Key words: Frailty, spa therapy, older adults, geriatric assessment.
Introduction
Frailty is a geriatric syndrome characterized by reduced physiological reserves, with a consequent increased vulnerability to adverse health outcomes, including diseases, disability and mortality (1). Furthermore, frailty can moderate the effects of interventions on clinical outcomes, such as disease treatments (2) and surgery (3). Therefore, identifying this syndrome in the context of the treatment of other health conditions may be crucial to adapt the intervention and increase its effectiveness.
Thermal/spa treatments, specially water immersion, have shown to benefit cardiovascular and neuromuscular systems(4). Its use has shown to be beneficial for healthy older adults (5) as well as older people with different conditions, including Parkinson’s disease (6), and constipation (7), but thermal/spa therapy are the most often used for the treatment of osteoarticular diseases in older adults (8–11). A randomized controlled trial (10) showed spa therapy (including balneotherapy and jet shower), compared to etodolac treatment, improved pain, anxiety, and quality of life in older adults with generalized osteoarthritis. Improvements in joint pain and function after balneotherapy may be mediated by its potential anti-inflammatory effects (12, 13). Osteoarticular diseases, which are very prevalent in older patients receiving thermal/spa treatments, are often associated to frailty in old adulthood (14–16). However, to the best of our knowledge, no study has examined the prevalence of frailty in patients receiving thermal/spa therapy.
The objectives of this study were two-fold: to investigate the prevalence of frailty in a sample of older people receiving thermal/spa therapy; and to study the feasibility of implementing geriatric assessments, including frailty, in the routine clinical consultations in thermal/spa facilities.
Methods
This study has a mixed design, with a quantitative cross-sectional investigation performed among patients of seven French thermal/spa facilities that volunteered to participate in this study and a qualitative investigation with the nine physicians working in the participating facilities. Spa therapy in France is prescribed by a physician and involves three mandatory consultations, performed about eight days apart from each other. In the quantitative cross-sectional study, geriatric assessments were undertaken in the context of these three consultations, with the first consultation used to enroll participants (ie, study presentation, checking participants eligibility); the second consultation was used to make the geriatric assessments, including frailty; the third consultation was used to provide the results of the assessments to the participants – a summary of such results were also sent to the participants’ general practitioner. The nine physicians working in the participating thermal/spa facilities who recruited patients for the current study were then interviewed (semi-structure interviews) about the feasibility of integrating the geriatric assessments in the thermal/spa consultations.
This study followed the principles of the Declaration of Helsinki for medical research in humans. Geriatric assessments were integrated into the usual mandatory clinical consultations of spa facilities. The study protocol was approved by the Consultative Committee for the Treatment of Research Information on Health (CCTIRS; registration number: 11 221). Participants received written information about the study; those who volunteered, signed the informed consent, and met the eligibility criteria were enrolled in the study and received the geriatric assessments.
Study Population
Participants of both sexes were eligible if they were ≥ 60 years and had been prescribed a spa therapy for 21 days, regardless of the reason for the thermal treatment; participants were excluded if they had any contraindication for spa therapy, if they had insufficient fluency in French impeding them to respond to the study questions/assessments, or if they were participating in another clinical study at the same time. On Mondays morning, between June and September 2013, consecutive patients fulfilling the eligibility criteria and who volunteered to participate in the study were enrolled. Two-hundred people were recruited, with exploitable data available for 197 individuals.
Nine physicians working in the participating spa facilities accepted to enroll patients in this study and were interviewed (qualitative part) about the feasibility of undertaking geriatric assessments, providing the results to the patients and a summary to the patient’s general practitioner, in routine spa therapy consultations. Interviews occurred on October 2013 and were recorded and transcribed.
Outcome measures
Frailty assessment
Frailty was operationalized based on the frailty phenotype (17) from the following self-reported items: frequent locomotion difficulties for going from one place to another; weight loss during the past few months; difficulty to climb one flight of stairs; difficulty to walk briskly one hundred meters; loss of interest or unexplained tiredness; difference between maximum weight during adulthood and current weight ≥ 4.5kg. Individuals meeting ≥3 criteria were considered frail; 1 or 2 criteria, pre-frail; 0 criterion, robust.
Feasibility of geriatric assessments
Semi-structured, recorded interviews were performed with the participating physicians. Topics approached during the interviews involved: the usefulness of questionnaires and geriatric assessments performed for facilitating the care of thermal/spa patients; and the extension in the consultation time length compared to the traditional thermal/spa consultation. Physicians, then, indicated whether they thought the geriatric assessments should be: a) integrated in the routine spa consultations; b) integrated in the consultations of specific/targeted patients, but not in routine; c) only in the context of health education, but not in patients’ consultation; d) only in the context of research protocols (not in the care of patients). The geriatric assessments undertaken were: mini-nutritional assessment (short form), instrumental activities of daily living (4-item scale), mini-geriatric depression scale (4-item scale), five-word test, and the clock-drawing test.
Other variables
Patients participating in the study completed a self-reported questionnaire informing on several health aspects, including perceived health and quality of life, sleep-related aspects, and prevalence of hypertension, type 2 diabetes, depression, and cardiovascular diseases (other than hypertension).
Data Analysis
Descriptive statistics, including frailty prevalence, of the thermal/spa therapy patients are presented as mean (SD) or median (interquartile range) and frequencies, as appropriate. Semi-structured interviews performed with nine participating physicians were transcribed for content analysis.
Results
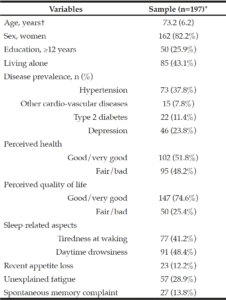
Table 1 presents the health characteristics of the study population. The 197 participants were aged in average 73.2 (6.2) years-old; 162 were women (82.2%). Hypertension was found in more than one third of patients and depression in almost one forth. More than half and nearly 75% of the population considered their overall health and quality of life as good/very good, respectively. Sleep problems were frequent.
*Sample size slightly varied due to missing data for some variables †Mean (SD); SD, standard deviation
Frailty was detected in 112 individuals (56.9%), 26 (13.2%) were considered pre-frail, and 59 (29.9%), robust. Table 2 provides the prevalence of each frailty criterion: prevalence varied from 33% for “difficulty to walk briskly one hundred meters” to 15.2% for “difficulty for going from one place to another”. Table 3 displays the results of the geriatric assessments performed.
*Sample size slightly varied due to missing data for some variables
*Sample size slightly varied due to missing data for some variables
Regarding the feasibility of integrating geriatric assessments to thermal/spa consultations, among the nine physicians, three indicated the geriatric assessments could be integrated in the routine spa consultations; two indicated the assessments could be integrated in the consultations of specific/targeted patients, but not in routine; two other, only in the context of health education, but not in patients’ consultation; and the last two suggested the assessments could only be used in the context of research protocols (not in the care of patients). The content of the interviews mainly highlighted that the geriatric assessments provided a better overview of the health status of the patients, with a clinical appraisal of several elements, such as malnutrition, mobility problems, and cognitive impairment.
Discussion
The present study is pioneer in investigating frailty among older adults receiving treatment in the thermal/spa setting. It was observed that frailty, as measured by a modified Fried frailty phenotype (17), is very prevalent, with more than half of older adults being classified as frail. Furthermore, more than half of the thermal/spa physicians involved in the implementation of geriatric assessments in the spa clinical consultations indicated such assessments could be integrated in clinical consultations in spa facilities at least for specific/targeted clinical older patients.
The very high prevalence of frailty found in this study was surprising given the relatively young age of the participants (aged in average 73.2 years old). This prevalence is higher than that found among nursing home residents, a population characterized by very old ages, multimorbidity and polymedication (18), and hospital patients observed in a meta-analysis (19). Indeed, that meta-analysis (19) found a frailty prevalence of 51.5% and 29.8% among nursing home residents aged in average 86 years-old and hospital patients aged in average 80 years, respectively. The high prevalence of frailty may be explained by the high prevalence of osteo-articular (8–11) and musculoskeletal (20) conditions in thermal/spa populations, given the important associations of osteo-muscular conditions and frailty (14–16, 21). However, we cannot exclude the possibility that our findings on frailty prevalence was partly influenced by the assessment tool used, which was composed of subjectively measured criteria/items focusing mostly on mobility-related aspects (eg, mobility difficulties, climbing stairs, walking briskly); mobility is often impaired in people with osteo-articular and musculoskeletal diseases.
With regards to the feasibility of implementing geriatric assessments in the routine clinical consultations of thermal/spa settings, the results were mixed. However, it is worth noting that the majority of the nine physicians interviewed indicated that the integration of geriatric assessments should be implemented at least for specific/targeted subpopulations of spa therapy patients. Furthermore, the content of the interviews revealed that geriatric assessments improved the physician’s clinical appraisal of the patient, what may ameliorate the care provided. These elements suggest that geriatric assessments should be considered in thermal/spa settings, especially for targeted individuals aged 65 and over with impaired mobility.
Taken together, the findings of the present work suggest that thermal/spa facilities may be an interesting clinical setting for screening for frailty and then for initiating timely preventive/therapeutic strategies, such as exercise and nutritional interventions. Such interventions may be implemented in addition to the traditional spa treatments (eg, balneotherapy). Although our study did not investigate frailty evolution over time during the spa therapy period, it is possible to think that the anti-inflammatory effects of spa treatments (12, 13) could reduce frailty severity. As one of the basic mechanisms leading to aging (22), low grade chronic inflammation is involved in the onset and severity of a myriad of age-related conditions (23–26), being an important biological substrate favoring the phenotypic expression of frailty (27, 28). Future investigations, in particular a randomized controlled trial, should examine the effects of spa therapy on frailty severity as well as on other health outcomes (eg, mobility, nutritional status, cognitive function, falls, hospital and nursing home admissions) in frail people.
This is the first study that examined frailty prevalence in the clinical setting of spa. The pragmatic approach, taking advantage of the medical staff working in the spa facilities, for implementing geriatric assessments is also worth mentioning. Nevertheless, some limitations should be recognized: this is a cross-sectional study, what impeded us of examining frailty evolution during the spa therapy period; sample size was relatively small; frailty was operationalized using self-reported criteria, with items that oversized the importance of mobility impairment.
In conclusion, frailty has a high prevalence in older adults receiving treatment in spa facilities. Furthermore, integrating elements of the comprehensive geriatric assessment in the routine clinical consultations of thermal/spa patients is feasible and should target specific clinical populations, such as older adults with possible mobility impairment. Further investigations, in particular using a randomized controlled trial design, are needed to evaluate the evolution of frailty severity during thermal treatment period as well as to test the effects of spa therapy on health outcomes according to the frailty status of patients.
Conflict of interest: No COI.
Acknowledgments: The study sponsor was the Association Française pour la Recherche Thermale (AFRETh). We would like to thank the following investigators: Dr Philippe Guerin (Vichy), Dr Denis Hours (Bourbon-Lancy), Dr Jean Claude Desprès (Vichy), Dr Céline Tabone (Capvern), Dr Michel Palmer (Aix les Bains), Dr Jean Suffran (Barbotan), Dr Agnes Dolci (Vichy), Dr Brigitte EYCHENNE-ENGEL (Barbotan),
Funding sources: This study received funding from the Association Française pour la Recherche Thermale (AFRETh – Grant number: C2010-06).
References
1. Clegg A, Young J, Iliffe S, Rikkert MO, Rockwood K. Frailty in elderly people. Lancet Lond Engl. 2 mars 2013;381(9868):752‑62.
2. Onder G, Vetrano DL, Marengoni A, Bell JS, Johnell K, Palmer K, et al. Accounting for frailty when treating chronic diseases. Eur J Intern Med. oct 2018;56:49‑52.
3. Ferguson R, Prieto-Alhambra D, Peat G, Delmestri A, Jordan KP, Strauss VY, et al. Does pre-existing morbidity influences risks and benefits of total hip replacement for osteoarthritis: a prospective study of 6682 patients from linked national datasets in England. BMJ Open. 23 sept 2021;11(9):e046712.
4. An J, Lee I, Yi Y. The Thermal Effects of Water Immersion on Health Outcomes: An Integrative Review. Int J Environ Res Public Health. 10 avr 2019;16(7):E1280.
5. Latorre-Román PÁ, Rentero-Blanco M, Laredo-Aguilera JA, García-Pinillos F. Effect of a 12-day balneotherapy programme on pain, mood, sleep, and depression in healthy elderly people. Psychogeriatr Off J Jpn Psychogeriatr Soc. mars 2015;15(1):14‑9.
6. Masiero S, Maghini I, Mantovani ME, Bakdounes L, Koutsikos K, Del Felice A, et al. Is the aquatic thermal environment a suitable place for providing rehabilitative treatment for person with Parkinson’s disease? A retrospective study. Int J Biometeorol. janv 2019;63(1):13‑8.
7. Dandinoglu T, Dandin O, Ergin T, Tihan D, Akpak YK, Aydın OU, et al. Can balneotherapy improve the bowel motility in chronically constipated middle-aged and elderly patients? Int J Biometeorol. juin 2017;61(6):1139‑48.
8. Masiero S. Thermal rehabilitation and osteoarticular diseases of the elderly. Aging Clin Exp Res. juin 2008;20(3):189‑94.
9. Gaisberger M, Fuchs J, Riedl M, Edtinger S, Reischl R, Grasmann G, et al. Endogenous anandamide and self-reported pain are significantly reduced after a 2-week multimodal treatment with and without radon therapy in patients with knee osteoarthritis: a pilot study. Int J Biometeorol. juill 2021;65(7):1151‑60.
10. Özkuk K, Uysal B, Ateş Z, Ökmen BM, Sezer R, Dilek G. The effects of inpatient versus outpatient spa therapy on pain, anxiety, and quality of life in elderly patients with generalized osteoarthritis: a pilot study. Int J Biometeorol. oct 2018;62(10):1823‑32.
11. Karagülle M, Kardeş S, Dişçi R, Gürdal H, Karagülle MZ. Spa therapy for elderly: a retrospective study of 239 older patients with osteoarthritis. Int J Biometeorol. oct 2016;60(10):1481‑91.
12. Gálvez I, Torres-Piles S, Ortega E. Innate/inflammatory bioregulation and clinical effectiveness of whole-body hyperthermia (balneotherapy) in elderly patients with osteoarthritis. Int J Hyperth Off J Eur Soc Hyperthermic Oncol North Am Hyperth Group. 2018;35(1):340‑7.
13. Maccarone MC, Magro G, Solimene U, Scanu A, Masiero S. From in vitro research to real life studies: an extensive narrative review of the effects of balneotherapy on human immune response. Sport Sci Health. 2021;17(4):817‑35.
14. Blanco-Reina E, Aguilar-Cano L, García-Merino MR, Ocaña-Riola R, Valdellós J, Bellido-Estévez I, et al. Assessing Prevalence and Factors Related to Frailty in Community-Dwelling Older Adults: A Multinomial Logistic Analysis. J Clin Med. 14 août 2021;10(16):3576.
15. Motta F, Sica A, Selmi C. Frailty in Rheumatic Diseases. Front Immunol. 2020;11:576134.
16. Salaffi F, Farah S, Di Carlo M. Frailty syndrome in rheumatoid arthritis and symptomatic osteoarthritis: an emerging concept in rheumatology. Acta Bio-Medica Atenei Parm. 11 mai 2020;91(2):274‑96.
17. Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. mars 2001;56(3):M146-156.
18. de Souto Barreto P, Lapeyre-Mestre M, Mathieu C, Piau C, Bouget C, Cayla F, et al. A multicentric individually-tailored controlled trial of education and professional support to nursing home staff: research protocol and baseline data of the IQUARE study. J Nutr Health Aging. févr 2013;17(2):173‑8.
19. Veronese N, Custodero C, Cella A, Demurtas J, Zora S, Maggi S, et al. Prevalence of multidimensional frailty and pre-frailty in older people in different settings: A systematic review and meta-analysis. Ageing Res Rev. déc 2021;72:101498.
20. Kamioka H, Nobuoka S, Iiyama J. Overview of Systematic Reviews with Meta-Analysis Based on Randomized Controlled Trials of Balneotherapy and Spa Therapy from 2000 to 2019. Int J Gen Med. 2020;13:429‑42.
21. Laskou F, Fuggle NR, Patel HP, Jameson K, Cooper C, Dennison E. Associations of osteoporosis and sarcopenia with frailty and multimorbidity among participants of the Hertfordshire Cohort Study. J Cachexia Sarcopenia Muscle. févr 2022;13(1):220‑9.
22. López-Otín C, Blasco MA, Partridge L, Serrano M, Kroemer G. The hallmarks of aging. Cell. 6 juin 2013;153(6):1194‑217.
23. Liberale L, Badimon L, Montecucco F, Lüscher TF, Libby P, Camici GG. Inflammation, Aging, and Cardiovascular Disease: JACC Review Topic of the Week. J Am Coll Cardiol. 1 mars 2022;79(8):837‑47.
24. Brahadeeswaran S, Sivagurunathan N, Calivarathan L. Inflammasome Signaling in the Aging Brain and Age-Related Neurodegenerative Diseases. Mol Neurobiol. 23 janv 2022;
25. Müller L, Di Benedetto S. How Immunosenescence and Inflammaging May Contribute to Hyperinflammatory Syndrome in COVID-19. Int J Mol Sci. 21 nov 2021;22(22):12539.
26. Santoro A, Bientinesi E, Monti D. Immunosenescence and inflammaging in the aging process: age-related diseases or longevity? Ageing Res Rev. nov 2021;71:101422.
27. Marcos-Pérez D, Sánchez-Flores M, Proietti S, Bonassi S, Costa S, Teixeira JP, et al. Association of inflammatory mediators with frailty status in older adults: results from a systematic review and meta-analysis. GeroScience. déc 2020;42(6):1451‑73.
28. Picca A, Coelho-Junior HJ, Calvani R, Marzetti E, Vetrano DL. Biomarkers shared by frailty and sarcopenia in older adults: A systematic review and meta-analysis. Ageing Res Rev. janv 2022;73:101530.