J. Min1, Y-C. Yeh2, I.S. Harvey3
1. College of Education and Human Development, Texas A&M University, College Station, TX, USA; 2 Graduate and Professional School, Texas A&M University, College Station, TX, USA; 3 School of Health Professions, University of Missouri-Columbia, Columbia, MO
Corresponding Author: Jungkyung Min, 107 Gilchrist Building, 2929 Research Parkway, College Station, TX 77843-4243 usa. E-mail: jkmin@tamu.edu; Mobile number: 979-450-2091; Fax number: 979-845-3109
J Aging Res & Lifestyle 2022;11:14-19
Published online May 25, 2022, http://dx.doi.org/10.14283/jarlife.2022.3
Abstract
Background: Aging is characterized by the decline in physical health, functional status, and loss of social roles and relationships that can challenge the quality of life. Social well-being may help explain how aging individuals experience declining physical health and social relationships. Despite the high prevalence of chronic conditions among older adults, research exploring the relationship between social well-being and chronic disease is sparse. Objectives: The study aims were to investigate the relationship between social well-being and psychological factors (e.g., perceived control, life satisfaction, self-esteem, active coping, optimism, and religious coping) by chronic condition in older adults. Design: Cross-sectional study. Participants: The current study comprises older adults (N = 1,251, aged ≥ 65 y) who participated in the third wave of the National Survey of Midlife in the United States (i.e., MIDUS). Setting: MIDUS was conducted on a random-digit-dial sample of community-dwelling, English-speaking adults. Measurements: Six instruments representing psychological resources (life satisfaction, perceived control, self-esteem, optimism, active coping, and religious coping) and five dimensions of social well-being (social actualization, social coherence, social acceptance, social contribution, social integration) were measured. An index of chronic disease comprised of self-reported data whether they had received a physician’s diagnosis for any chronic conditions over the past year. Results: The findings indicated that the individuals without chronic conditions had significantly higher social integration, social acceptance, and social contribution scores than the individuals with chronic conditions (t = 2.26, p < 0.05, t = 2.85, p < 0.01, and t = 2.23, p < 0.05, respectively). For individuals diagnosed with more than one chronic condition, perceived control, self-esteem, and optimism were positively related to their social well-being (β = .33, p < .001, β = .17, p < .001, and β = .33, p < .001, respectively). Conclusion: Findings suggested that older adults with multiple chronic conditions have a decrease in social well-being. Chronic disease management programs may help increase social well-being among individuals with multiple chronic conditions.
Key words: Social well-being, chronic disease condition, older adults, quality of life.
Introduction
Incidence rates of chronic diseases tends to become more familiar with age (1). It is known that approximately 80% of older adults have at least one chronic disease (2). Numerous studies have demonstrated healthy aging (interchangeably named by some researches as “active aging” or “successful ageing”) as not suffering from primary chronic disease. However, in light of the higher rate of chronic illness among older adults, it is essential to incorporate different psychological and social well-being dimensions to evaluate the quality of life (3, 4).
Prior studies on older adults’ healthy aging with chronic conditions revealed that several dimensions of social well-being working through various psychological well-being factors that may enhance an individual’s likelihood of restorative processes (4-7). For example, social relationships can improve self-efficacy among individuals actively engaging in health behaviors (e.g., physical activity and smoking cessation) (4).
Although the previous study has highlighted the role of psychological well-being on older adults’ physical health, the gap in the literature is a lack of research on how social well-being contributes to older adults’ well-being based on chronic disease conditions (8, 9). Additionally, inquiring about the relationship between social well-being and psychological factors that contribute to healthy aging is essential to reduce the risk of age-related chronic conditions (4, 7). Therefore, the purpose of this study was to identify the relationship between social well-being and psychological factors by chronic condition in older adults. The objectives of the study are 1) older adults with chronic conditions will report lower levels of social well-being than older adults without chronic conditions, 2) the relationship between social well-being and psychological factors will vary by chronic conditions, and 3) the regression path from psychological factors to social well-being will be inequivalent in older adults with chronic conditions compared to older adults without chronic conditions.
Methods
Samples
The current study is a secondary analysis of data from the third wave of Midlife Development in the United States (MIDUS 3). MIDUS study’s focus was to recruit a sample of adults to follow longitudinally to understand the process of midlife development. Initiated in 1995, the survey of MIDUS comprises a nationally representative random-digit-dial sample of community-dwelling, English-speaking men and women aged 25–89 years residing in the 48 contiguous states. Among the sample of 3,294 respondents, this study included the participants ages 65 years old and older who had fully completed MIDUS 3 and responded to the key variables (social well-being, chronic disease condition, and psychological factors) – this resulted in a final sample size 1,251. More detailed information on MIDUS project can be found elsewhere (10) .
Measure
Measures for this study were compiled in several ways, using well-validated scales. The key outcome variable was social well-being, with explanatory variables being chronic conditions and psychological factors.
Social well-being
Social well-being was assessed with Keyes’s validated 14-item scale (α = .78). (6). The scale measured five dimensions of social well-being including social actualization (e.g., “The world is becoming a better place for everyone.”), social coherence (e.g., “The world is too complex for me.”), social acceptance (e.g., “People who do a favor expect nothing in return.”), social contribution (e.g., “I have nothing important to contribute to society.”), social integration (e.g., “I don’t feel I belong to anything I’d call a community.”). Each item under five components was scored on a 7-point Likert scale, from 1= strongly disagree to 7 = strongly agree, with higher scores representing greater social well-being. Negatively worded items were reverse coded prior to all analyses. Scores were computed as the summing of the item scores for each variable.
Chronic disease condition
Participants completed questionnaires comprised of self-reported data whether they had received a physician’s diagnosis for any chronic diseases over the past year. The following conditions were assessed: high blood pressure, diabetes, stroke, asthma/chronic bronchitis/emphysema, tuberculosis, other lung disease, persistent skin problems, lower back pain, urinary/bladder problems, ulcer, bone and joint problems and hernia/rupture.
Psychological factors
The questionnaire included the following six instruments representing psychological resources. The perceived control assessed personal mastery (α = .73) with four items (e.g., “I can do just about anything I really set my mind to”), and perceived constraints (α = .85) with eight items (e.g., “What happens in my life is often beyond my control”) (11). The scores ranged from 1 (strongly agree) to 7 (strongly disagree); negatively worded items were reverse coded so that higher score reflected a greater sense of control. The life satisfaction domain was assessed using six items capturing life satisfaction regarding work, financial situation, health, and relationship with the family. Prenda & Lachman (12) suggested that the five-item life satisfaction scale showed adequate internal consistency (α=.71). Each item was coded from 1 (worst possible) to 10 (best possible), with higher values representing higher life satisfaction. The self-esteem was measured using seven items (e.g., “I am able to do things as well as most people.”) from the Rosenberg’s Self-esteem scale (Rosenberg, 1965). The scores ranged from 1 (strongly agree) to 7 (strongly disagree); negatively worded items were reverse coded such that a higher values indicated better self-esteem (α=.76). Active coping scale (α=.75) was assessed with four items (e.g., “I concentrate my efforts on doing something about it”) (13). The scores ranged from 1 (a lot) to 4 (not at all) and the responses were coded so that higher score reflected a greater usage of coping style. Optimism was measured using the Life Orientation Test-Revised (LOT-R) by a 3-item measure of the tendency to expect positive outcomes (e.g., “I expect more good things to happen to me than bad”) (14) Each item was coded from 1 (disagree a lot) to 5 (agree a lot) with higher scores representing more significant levels of optimism (α =.80). Religious coping (α=.71) was assessed using two items (e.g., “When you have decisions to make in your daily life, how often do you ask yourself what your religious or spiritual beliefs suggest you should do?”) (15). The scores ranged from 1 (often) to 4 (never), which were recoded to have higher scores representing greater sense of religious control.
Statistical analysis
SPSS Statistics version 22.0 (IBM Corp., Armonk, NY, USA, 2013) was used to process the zero-order correlations to understand the strength of the association among psychological factors and different types of social well-being as well as to conduct the t-test analysis to examine the difference between older adults with and without chronic conditions on different types of social well-beings. A structural equation modeling (SEM) was then applied to examine the relations between psychological factors and social well-being. In addition, multiple-group invariance tests were used to examine whether the relations of psychological factors and social well-being were equivalent in the sample of older adults with and without chronic conditions. The models were processed using MPlus (16).
The χ2 statistic, the root means square error of approximation (RMSEA), the comparative fit index (CFI), and the standardized root mean square residual (SRMR) were employed in the goodness-of-fit test. The χ2 statistic is considerably sensitive to sample size; it only presented the χ2 statistic instead of using it as a goodness-of-fit index, as suggested by Jöreskog and Sörbom (17). In a model that fits the data, a value of the RMSEA between 0.05 and 0.08 is indicated as a fair fit and in the range of 0.08 to 0.10 to indicate mediocre fit. A value of the CFI exceeding 0.90 is considered an acceptable model, and the SRMR ≤ 0.08 is adopted as the criteria for a well-specified model. The chi-square difference (Δχ2) of the constrained and unconstrained models was analyzed to test the multi-group model for the relationship between older adults with or without chronic conditions; we noted the change in relationship when older adults reported more than one chronic condition.
Results
Demographic information
Participants’ ages ranged from 65 to 86 years (M=70.85, SD=7.66), with 54.4% identified as female. Furthermore, 89.7% of participants identified as White, 3.4% Black, and 6.9% others. Additionally, 84.4% of participants reported having at least one chronic disease at the survey time. In terms of chronic conditions, anxiety and depression (81.1%) were the most reported chronic conditions, followed by diabetes (80.9%), stomach trouble (80.8%), joint bone disease (65.9%), and hypertension (52.9%).
In comparison, the sample not included in the analysis, the percentage of the respondents among midlife adults (ages between 42 to 64 years) diagnosed with at least one chronic disease was lower than that of the older adults (60.8% vs. 84.4%). Additionally, it is noteworthy to look at the mean age difference between midlife and older adults (55.4 vs. 70.8).
Intercorrelations among psychological factors and different types of social well-being
Table 1 displayed the correlation results of psychological factors and different types of social well-beings for both individuals with chronic conditions and individuals without chronic conditions samples. For the individuals with chronic conditions sample, perceived control, life satisfaction, self-esteem, and optimism were statistically and positively association with all dimensions’ of social well-being (p < 0.01). Active coping had a significant and positive association with social coherence, social integration, social acceptance, social contribution (p < 0.01), and social actualization (p < 0.05). Religious coping was negatively associated with social coherence and social actualization (p < 0.01), but was positively related with social integration and social contribution (p < 0.01). However, religious coping was uncorrelated with social acceptance (p > 0.05).
Note. The upper and lower triangular areas display the individuals with chronic conditions and individuals without chronic conditions samples, respectively. PC = Perceived Control; LS = Life Satisfaction; SE= Self-Esteem; AC = Active Coping; RC = Religious Coping; SCoh = Social Coherence; SI = Social Integration; SAcc = Social Acceptance; SCon = Social Contribution; SAct = Social Actualization. *p < .05; **p < .01.
For the individuals without chronic conditions sample, perceived control was significantly and positively correlated with four domains of social well-being (p < 0.01) except for social acceptance (p > 0.05). Life satisfaction were all significantly and positively correlated with social coherence (p <0.05), social integration, social acceptance, social contribution, and social actualization (p < 0.01). Self-esteem was uncorrelated with social acceptance (p > 0.05) but was significantly and positively correlated with other dimensions (p < 0.01). Active coping was all significantly and positively correlated with social contribution and social coherence (p < 0.01), social integration, social acceptance, and social actualization (p < 0.05). Optimism were all significantly and positively correlated with all five dimensions of social well-being (p < 0.01). Religious coping was significantly and positively correlated with social integration (p < 0.01) and social contribution (p < 0.05).
As shown in Table 2, the independent-samples t-test results showed that the individuals without chronic conditions had significantly higher social integration, social acceptance, and social contribution scores (t = 2.26, p < 0.05, t = 2.85, p < 0.01, and t = 2.23, p < 0.05, respectively) than the individuals with chronic conditions.
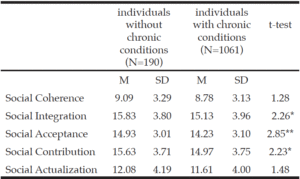
Table 2
t-test Results Comparing Individuals Without Chronic Conditions and Individuals with Chronic Conditions on Different Types of Social Well-Beings
*p < .05; **p < .01.
The structural model of the relations between psychological factors and social well-being
The individuals with chronic conditions and individuals without chronic conditions models exhibited an acceptable goodness of fit (χ2(25) = 33.742, p > 0.05, RMSEA = 0.04, CFI = 0.97, SRMR = 0.04; χ2(25) = 193.591, p < 0.001, RMSEA = 0.08, CFI = .90, SRMR =0 .05, respectively). Figure 1 and 2 provided the estimated coefficients of the separate individuals with chronic conditions and without chronic conditions models, respectively. As shown in Figure 1, individuals who reported high perceived control, self-esteem, and optimism had had an increase in their social well-being (β = 0.33, p < 0.001, β = 0.17, p < 0.001, and β = 0.33, p < 0.001, respectively) for the individuals with chronic conditions model. As shown in Figure 2, only individuals who reported high levels of optimism and did not report having a chronic condition had an increase in their social well-being (β = 0.48, p < 0.001).
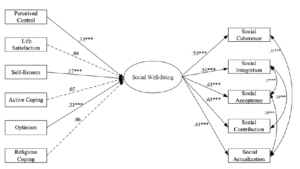
Figure 1
The relationships between psychological factors and
social well-being for the individuals with chronic
conditions
Note. All the coefficients are standardized coefficients. Dashed lines represent no significant association. ***p < .001.
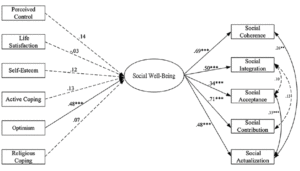
Figure 2
The relations between psychological factors and social well-being for the individuals without chronic conditions
Note. All the coefficients are standardized coefficients. Dashed lines represent no significant association. **p < .01. ***p < .001
Invariance of the regression paths from psychological factors to social well-being
Multiple-group invariance tests were used to examine whether the relations of psychological factors and social well-being were equivalent in the samples of older adults with or without chronic conditions. Table 3 displayed the fit indices of the multi-group results examining the relationship between older adults with or without chronic conditions. The fit indices of the multi-group baseline model (M0) implied that the model was acceptable (χ2 (58) = 236.243, p < 0.001, RMSEA = 0.07, CFI = 0.91, SRMR = 0.06). We established six equivalent models and compared the baseline model’s chi-square values. Only one ∆x2value of the model (M5) represented a significant difference, indicating that this parameter signified inequivalence between with and without chronic conditions samples. However, the ∆x2values of the remaining five equivalent models (M1, M2, M3, M4, M6) did not reach significance levels, implying that the individuals with and without chronic conditions can be viewed as equivalents for them.

Table 3
Fit Indices for Multi-Group Model of Chronic Conditions among Older Adults for the Individuals Without Chronic Conditions and the Individuals With Chronic Conditions Samples
Note. PC = Perceived Control; LS = Life Satisfaction; SE= Self-Esteem; AC = Active Coping; Opt = optimism; RC = Religious Coping; SWB = Social Well-Being. *p < .05.
Discussion
Although it has been known that a multidimensional perspective is essential to evaluate the older adults’ quality of life, research regarding social well-being and linkage between social well-being and psychological factors have not been explored. To the best of our knowledge, this study sought to exam the relationship between social well-being and psychological factors among older adults with chronic conditions compared to individuals without chronic conditions.
This study was conducted based on the hypothesis that chronic disease conditions will affect social well-being among the older population and examine the relationship between psychological factors and social well-being. The results entirely supported the study hypotheses. The first objective found that the levels of social well-being between individuals with chronic conditions and without chronic conditions were significantly different based on the number of chronic conditions. The finding is in line with other studies which reported that chronic disease status is a more important factor of well-being than other demographic determinants (18, 19). However, most research on well-being and chronic disease has been discussed in terms of subjective and psychological well-being (20). Therefore, more attention should be paid to social well-being as a critical component of health among older adults.
The second objective found that the relationship between psychological factors and social was partially supported. According to the analysis, each group (i.e., with and without chronic conditions) has different patterns of relations. The variables (e.g., perceived control, self-esteem, and optimism) were positively related to social well-being among individuals with chronic conditions while only optimism among individuals without chronic conditions. This finding supports that educational program that promote individuals’ sense of control are substantially beneficial in managing health-related distress among old adults. The authors also noted that perceived control could play a critical role in social relationships (21). A cross-sectional study of older adults with os teoarthritis stated that greater optimism is significantly associated with well-being with fewer depressive symptoms and great life satisfaction (22). Although positive psychological functioning on physical health have been discussed (23), studies on how positive factors affect social health in the presence of chronic diseases are insufficient. Given that positive psychological factors are related to social well-being in older adults, future research should explore potential underlying mechanisms between psychological factors and social well-being.
Regarding support for our third objective, the results in regard to the invariance of the regression paths from the psychological variables to social well-being, only optimism on social well-being was an inequivalence relationship between two different chronic conditions groups. Additionally, it appears that life satisfaction had no significant relationship with social well-being for both groups. The findings regarding optimism and social well-being are compatible with previous research. Previous research revealed that optimism was a significant variable of subjective and psychological well-being in a condition of chronic disease as well as healthy older adults (23, 24). Findings are also supported by studies investigating the association between higher optimism and increased likelihood of healthy aging, supporting that higher levels of optimism were associated with a greater likelihood of healthy aging among diverse populations (25). Further, other research pointed out that optimism contributed to establishing healthier behaviors such as exercising regularly, good nutrition, and weight control (26). Even though little is known about the relationship between optimism and social well-being, it is worth noting that these results serve to highlight that optimism may be an essential psychological resource for healthy aging and that possible psychosocial intervention to improve social health for older adults.
Several limitations need to be considered in the interpretation of the results. First, this study uses self-report questionnaires, which may expose our findings to the risk of same-source bias. This may result in overestimating the magnitude of coefficients and Type I error, so future studies should include qualitative and quantitative data with larger samples and longitudinal measures. Second, this study did not include the demographic variables such as age, gender, and educational attainment between psychological factors and social well-being. Psychosocial factors might differ depending on the sociodemographic variables. Thus, future research could examine how the relationship between psychosocial factors and social well-being varies across sociodemographic groups. Third, the MIDUS cohort was primarily composed of Whites or Caucasian Americans. As such, overall results likely cannot be generalizable to other diverse populations. Despite these limitations, to the best of our knowledge, the present study contributes significantly to understanding of the relationship between social well-being and psychological factors which might play a significant role in chronic conditions among older adults. Finding suggests that chronic conditions significantly affect social well-being, and that psychological factors are positively associated with social well-being that contributes to healthy aging.
Conclusion
Considering the results, it can be inferred that chronic conditions may explain social well-being among older adults. Psychological factors such as perceived control, self-esteem, and optimism affect social well-being, with significant correlations among older adults who diagnosed with at least one chronic disease. Therefore, our findings make a step toward understanding social well-being in terms of chronic conditions and may be useful for chronic disease management in increasing social well-being among individuals with multiple chronic conditions. Optimism’s relationship with social well-being for individuals is an interesting finding of this study, meriting further investigation in the future.
Funding: This research received no external funding.
Ethical standard: The authors declare the study procedures comply with all ethical standards.
Conflicts of Interest: The authors declare no conflict of interest.
References
1. Buttorff C, Ruder T, Bauman M. No title. Multiple chronic conditions in the united states.Santa Monica (CA): RAND Corporation; 2017. 2017.
2. Centers for Disease Control and Prevention. Public health and aging: Trends in aging–US and worldwide. Retrieved August. 2003;8:2008.
3. Young Y, Frick KD, Phelan EA. Can successful aging and chronic illness coexist in the same individual? A multidimensional concept of successful aging. Journal of the American Medical Directors Association. 2009;10(2):87-92.
4. Kim ES, Tkatch R, Martin D, MacLeod S, Sandy L, Yeh C. Resilient Aging: Psychological Well-Being and Social Well-Being as Targets for the Promotion of Healthy Aging. Gerontology and Geriatric Medicine. 2021;7:23337214211002951.
5. Gawronski KA, Kim ES, Langa KM, Kubzansky LD. Dispositional optimism and incidence of cognitive impairment in older adults. Psychosom Med. 2016;78(7):819.
6. Bar-Tur L. Fostering Well-Being in the Elderly: Translating Theories on Positive Aging to Practical Approaches. Frontiers in Medicine. 2021;8:200.
7. Ryff CD. Understanding positive aging as an integrated biopsychosocial process. Wisconsin-Madison: Institute on aging. 2012.
8. Wikman A, Wardle J, Steptoe A. Quality of life and affective well-being in middle-aged and older people with chronic medical illnesses: a cross-sectional population based study. PLoS One. 2011;6(4):e18952.
9. Waite LJ. Social well-being and health in the older population: moving beyond social relationships. Future Directions for the Demography of Aging: Proceedings of a Workshop. National Academies Press; ; 2018.
10. Ryff C, Almeida DM, Ayanian JS, Carr DS, Cleary PD, Coe C, et al. National survey of midlife development in the United States (MIDUS II), 2004-2006. . 2007.
11. Lachman ME, Weaver SL. The sense of control as a moderator of social class differences in health and well-being. J Pers Soc Psychol. 1998;74(3):763.
12. Prenda KM, Lachman ME. Planning for the future: a life management strategy for increasing control and life satisfaction in adulthood. Psychol Aging. 2001;16(2):206.
13. Carver CS, Scheier MF, Weintraub JK. Assessing coping strategies: a theoretically based approach. J Pers Soc Psychol. 1989;56(2):267.
14. Scheier MF, Carver CS, Bridges MW. Distinguishing optimism from neuroticism (and trait anxiety, self-mastery, and self-esteem): a reevaluation of the Life Orientation Test. J Pers Soc Psychol. 1994;67(6):1063.
15. Garfield AM, Ryff CD, Singer B. Religion and health: Probing the connections. annual conference of the American Psychological Society; ; 2001.
16. Muthén LK, Muthén BO. Mplus user’s guide Eighth edition Los Angeles. CA: Muthén & Muthén. 1998;2017.
17. Jöreskog KG, Sörbom D. LISREL 8: Structural equation modeling with the SIMPLIS command language. Scientific Software International; 1993.
18. Okely JA, Gale CR. Well-being and chronic disease incidence: the English longitudinal study of ageing. Psychosom Med. 2016;78(3):335.
19. Westaway MS. The impact of chronic diseases on the health and well-being of South Africans in early and later old age. Arch Gerontol Geriatr. 2010;50(2):213-21.
20. National Academies of Sciences, Engineering, and Medicine, Committee on Population. Future directions for the demography of aging: Proceedings of a workshop. 2018.
21. Mallers MH, Claver M, Lares LA. Perceived control in the lives of older adults: The influence of Langer and Rodin’s work on gerontological theory, policy, and practice. Gerontologist. 2014;54(1):67-74.
22. Ferreira VM, Sherman AM. The relationship of optimism, pain and social support to well-being in older adults with osteoarthritis. Aging Mental Health. 2007;11(1):89-98.
23. Schiavon CC, Marchetti E, Gurgel LG, Busnello FM, Reppold CT. Optimism and hope in chronic disease: a systematic review. Frontiers in psychology. 2017;7:2022.
24. Ferguson SJ, Goodwin AD. Optimism and well-being in older adults: The mediating role of social support and perceived control. The International Journal of Aging and Human Development. 2010;71(1):43-68.
25. Lee LO, James P, Zevon ES, Kim ES, Trudel-Fitzgerald C, Spiro A, et al. Optimism is associated with exceptional longevity in 2 epidemiologic cohorts of men and women. Proceedings of the National Academy of Sciences. 2019;116(37):18357-62.
26. Kim ES, James P, Zevon ES, Trudel-Fitzgerald C, Kubzansky LD, Grodstein F. Optimism and healthy aging in women and men. Am J Epidemiol. 2019;188(6):1084-91.

