S. Fleury1,2, C. Sulmont-Rossé1, H. Cabanes2, M. Perruchaud2, A. Roger1, B. Lesourd3, P. Tronchon2, V. Van Wymelbeke-Delannoy1,4, I. Maître5
1. Centre des Sciences du Goût et de l’Alimentation, AgroSup Dijon, CNRS, INRAE, Université de Bourgogne Franche-Comté, Dijon, France; 2. Saveurs et Vie, Orly, France; 3. Département de Gériatrie CHU, Clermont-Ferrand, France; 4. CHU Dijon Bourgogne, Dijon, France; 5. USC 1422 GRAPPE, Ecole Supérieure d’Agricultures (ESA), SFR 4207 QUASAV, INRAE, 55 rue Rabelais, Angers, France
Corresponding Author: Ségolène Fleury, Centre des Sciences du Goût et de l’Alimentation, AgroSup Dijon, CNRS, INRAE, Université de Bourgogne Franche-Comté, F-21000 Dijon, France, segolene.fleury@inrae.fr
J Aging Res & Lifestyle 2020;9:40-46
Published online November 19, 2020, http://dx.doi.org/10.14283/jarlife.2020.9
Abstract
Objective: The present study aimed at assessing the feasibility and the effectiveness of a personalized dietary intervention in a meals-on-wheels service through a randomized controlled pilot trial. Design: Sixty recipients of home-delivered meals (75% of women; 70-97 years old) were recruited and randomly assigned to a control and an experimental group and followed over a period of 4 months. In the experimental group, the nutritional status (Mini-Nutritional Assessment – MNA questionnaire), the food intake and the food preferences were measured for each participant. Based on this screening, participants were provided with dietary guidance and follow-up. Those at risk of malnutrition were proposed enriched home-delivered meals. Enrichment was set up considering food preferences of the participants. Results: Looking at the whole sample at baseline, 80% (n=48/60) were at risk of malnutrition. Furthermore, 55% (n=33/60) ate less than 2/3 of their calorie and/or protein recommended allowances. In the experimental group, the intervention led to an increase of protein intakes and to a lower extent of calorie intake. In the control group, no significant changes were observed. Conclusion: To conclude, this study suggests that providing dietary guidance and adding nutrient-dense food to meals while considering food preferences is feasible and may help older beneficiaries of meals-on-wheels to increase calorie and protein intake and improve their nutritional status. However, there is a need to develop products or recipes to enrich the meals of the elderly more efficiently to achieve the recommended allowance.
Key words: Aged, nutritional intake, fortified food, home-meal delivery, malnutrition.
Introduction
In old age, the onset of physical or cognitive disability may affect an individual’s ability to achieve daily activities and notably those related to food (grocery shopping, cooking) (1). At home, assistance for food-related activities is often provided by a family or a professional caregiver. However, an increasing number of older people are subscribing to a home-delivery meal service (also known as meals-on-wheels) with 80,000 recipients in France (2). The risk of malnutrition was reported to be higher in older people receiving help for their meals than in autonomous people. At home, Maître et al. (3) observed that 46% of the people receiving food-related help (food purchasing, cooking, meals-on-wheels) were at risk of malnutrition against 16% of the people with food-unrelated help (housekeeping, personal care). Crichton et al. (4)’s meta-analysis showed that older people receiving homecare services display the highest malnutrition prevalence of all the community-dwelling elderly sample. In this context, some studies have developed and tested the impact of dietary interventions on the nutritional status of meals-on-wheels beneficiaries. The combined results of articles described in the systematic literature review of Ijmker-Hemink et al. (5) demonstrated that “enriching” the meals-on-wheels offer (e.g. providing additional meals, fortified dishes) led to an improvement of beneficiaries’ nutritional status (6–13). It should be noted that all these studies provided the same dietary intervention to the participants from the experimental groups, without considering the nutritional status nor the food preferences of participants at baseline (see for instance 10, 11). However, it is crucial to propose dietary intervention accounting for the nutritional needs and food preferences of the recipients to ensure relevance and compliance of the dietary support. In fact, older people are often reluctant to change their food habits. Building on these foundations, the rationale of the present study was to develop a personalized dietary intervention tailored to the nutritional needs and the food preferences of the older recipients of a meals-on-wheels service and assess its feasibility and effectiveness through a randomized controlled pilot trial. The intervention included three steps: 1) screening for the nutritional status, the food intake and the food preferences of older people; 2) based on this screening, adapting the meals-on-wheels offer to increase the calorie and protein content of the meals to help the participants at risk of malnutrition fulfil their recommended allowance; 3) dietary guidance and regular follow-up by a dietitian to track any nutritional change.
Methods
Design
This pilot study was a randomized parallel group study, with a control group and an experimental group (implementation of a personalized dietary intervention). Follow-up lasted four months and outcome measurements were done at baseline (t0), mid-term (t2) and at the end of the intervention (t4). The design was approved by the French Ethics Committee for Research (CPP ESTI 2015/24 – IDRCB N° 2015-A01324-45) and informed consent was obtained from all the participants. It should be noted that the foreseen protocol planned a follow-up of six months. Unfortunately, because of an administrative issue, we had to reduce this follow-up to four months (the city of Paris launched an unexpected tender process to renew the bargain with a home-meal delivery society). The trial was registered in a publicly accessible database (ClinicalTrials.gov; registration number: NCT02866474).
Participants
Participants were recruited from February to August 2018 among older people currently receiving a meals-on-wheels service managed by the social action center of Paris (CASVP). This service offers the participants to choose the number of meals and the type of meal (breakfast, lunch, and dinner) they want to receive each week. Regular breakfast includes a hot drink, bread, and spreads. Regular lunch includes a starter, a main dish with a protein component, a dairy product, a dessert, and bread. Regular diner includes a starter or a soup, a protein dish, a dessert, and bread. Participants were eligible for this study if they were 70 years old or older and if they received at least 5 meals a week. Participants were not included in the study when they were experiencing an acute pathological episode at the time of the study (exclusion criteria). Once included, participants carried out a home-interview to collect the following baseline characteristics: sociodemographic data (age, gender, partner status, education level, self-perception of financial resources), anthropometry (weight, Body Mass Index – BMI), meals-on-wheels history, number of comorbidities, number of medications, cognitive status (Mini Mental State Examination – MMSE; (14)), and functional status (Instrumental Activities of Daily Living Scale – IADL; (15). The MMSE is an 11-question measure that tests five areas of cognitive function: orientation, registration, attention, recall and language. The score ranges from 0 to 30 (best cognitive performances). The Instrumental Activities of Daily Living Scale (IADL) assesses a person’s ability to perform tasks such as using a telephone, doing laundry, handling finances (eight domains are considered). The IADL score ranges from 0 to 8 (good independent living skills). When a participant was diagnosed as malnourished at baseline, information was provided to his/her general practitioner following ethical rules. Further prescriptions of ONS were tracked but no additional ONS prescription was recorded in malnourished participants during the length of this study.
Randomization
Following the home-interview, participants were randomly allocated to the control or the experimental group. A computerized random generator (Excel script) constructed by an independent person from the investigators was used to assign participants to either the experimental group or the control group. Enrolment and random allocation were made by different research assistants: enrolment was made by co-authors SF and MP (in Paris) and random allocation was made by co-author AR (in Angers). After each enrolment, AR received anonymous information about the new volunteer. SF and MP remained unaware of the random allocation sequence throughout the experiment.
Control group
Participants from the control group received regular meals-on-wheels service offered by the social action center of Paris.
Experimental group
A personalized dietary intervention was proposed in addition to the regular meals-on-wheels service offered by the social action center of Paris to participants from the experimental group. This intervention included three steps.
Screening
A dietician established the participant’s ‘eating profile’ from his nutritional status, food intake and food preferences during a one-hour home-visit. The nutritional status was determined according to the MNA score: participants were considered at risk of malnutrition for an MNA score < 23.5. Food intake was measured with a 24-hour dietary recall. Finally, participants were asked to rate their liking for food products which are potentially good candidates to increase the calorie and protein content of home-delivered meals. Food products included high-protein foods (e.g. cheese, ham) and food matrices in which high-caloric/high-protein ingredients could be added (e.g. soup, cream). Rating were made on 5-point scales ranging from “I do not like at all” on the left to “I like a lot” on the right.
Meal enrichment
Participants who were at risk of malnutrition were proposed enriched home-delivered meals. Enrichment target to increase the daily intake about 125-250 kcal and 15-30 g of protein depending on their initial nutritional intake (16, 17). Enrichment was set up considering the preferences of the participants. Enrichment consisted in adding high-protein foods (e.g. slice of ham, dairy products, fortified cream), high-caloric/high-protein ingredients to be added in regular dishes (e.g. grated Gruyère), or ONS (e.g. Delical®, Clinutren®, Protifruit®, bread G-Nutrition®). Participants who were not a risk of malnutrition continued to receive the regular home-delivered meals.
Dietary guidance and follow-up
After the first 15 days and then once a month, the dietician contacted all the participants (at risk and not at risk of malnutrition) by phone to track any nutritional status change and provide dietary guidance. The dietician encouraged participants to fulfil their daily recommended allowances. In addition, participants who were at risk of malnutrition were questioned about the meal enrichment they received and additional food products were adjusted if necessary (e.g. replacing certain food items).
Outcomes measures
Outcomes included the nutritional status determined according to the Mini Nutritional Assessment (MNA). The MNA consists into 18 items including anthropometric measurements (weight, upper arm, and calf circumferences), dietary and health items and ranges from 0 to 30 (0-16: malnutrition ; 17-23.5: at risk of malnutrition ; 24-30: well nourished) (18). Outcomes included also the food intake measured with the 24-hour recall method (7, 10, 11). The nutrient composition of each food and drink item was determined from the Ciqual French food composition table (2016) (19). Calorie and protein ratios (expressed in percentage) were computed by dividing the calorie or protein intake with the recommended daily allowances: 30 kcal and 1.2 g of protein / kg of body weight / day (20, 21). Finally, body weight was measured with a scale (TERRAILLON®). Participants were weighed with their clothes and the weight was adjusted by subtracting the average weight of the type of clothing they wore (22).
Data analysis
Baselines characteristics of the two groups were compared by submitting the variables collected at t0 to a Student’s t test (continuous variables) or a Fisher’s exact test (categorical variables). Descriptive data were presented in percentages or means (M) and standard errors (SE). Outcome measures were submitted to a two-factor mixed linear model (model lme, R studio) with the group, time and group*time interaction as fixed factors and participants as the random factor. Contrast analyses were performed to compared adjusted means obtained from the models. Adjusted means (M) were presented with their standard errors (SE). Statistical analyses were performed using R studio (Version 1.1.447 – © 2009-2018 RStudio, Inc.). The threshold for significance was set at 5%.
Results
Nutritional status and food intake at baseline
Sixty participants were included in the study (women ratio: 75%; age mean: 83 (SD=7); age range: 70-97). According to the MNA questionnaire, 48 participants (80%) were at risk of malnutrition (score < 23.5). According to the food intake assessment, only 3 participants fulfilled their recommended allowance (calorie and protein ratios ≥ 100%). For the remaining participants, the average deficit between intake and recommended allowance was 800 (SD=592) kcal and 27 (SD=24) g of protein. Furthermore, 33 participants (55%) displayed a calorie and/or protein ratio < 66% and could be qualified as ‘very small eaters’.
Impact of the intervention
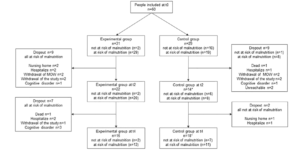
During the 4 months of follow-up, 27 participants dropped out of the experiment (Figure 1). For the remaining participants, data were collected at t2 for 14 control and 22 experimental participants, and at t4 for 18 control and 15 experimental participants. It should be noted that in the control group, 6 participants completed data collection at baseline and t4, but not at t2.
* 6 participants (3 not at risk; 3 at risk) completed data collection at baseline and 14, but not at 12 because (1 was hospitalized, 2 were on holiday, and 3 were unavailable). MOW: meal-on-wheels
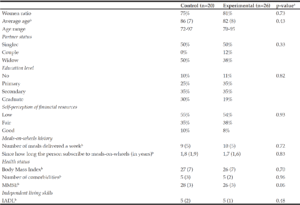
Table 1 presents the baseline characteristics of the participants for which data were collected at t2 and/or t4. It should be noted that 40% of the sample had a low education level and that 55% declared having low financial resources. On average, participants received 10 meals a week (SD=6) and they had been subscribing to the meal delivery service for 1.6 years (SD=1.6); no difference was observed between the control and the experimental groups. According to the MNA, 19 (65%) participants in the control group and 29 (94%) participants in the experimental group were at risk of malnutrition. Participants at risk of malnutrition from the experimental group received a “personalized dietary intervention”. The average supplementation that was provided in addition to regular home-delivered meals was 284 kcal (SD=99) and 21 g of protein (SD=12). It should be noted that for very small eaters (calorie and/or protein ratios < 66%), meal enrichment was not sufficient to compensate for their nutritional deficit. On average, they received an additional supply of 311 kcal (SD=113) and 20 g of protein (SD=8) for an initial deficit of 1 176 kcal and 42 g protein.
a. p-value derived from either a Student t test (continuous variable) or a Fisher’s exact test (categorical variables) to compare the control and the experimental group; b. Mean (Standard Deviation). c Bachelor and divorced. The MMSE score ranges from 0 to 30 (best cognitive performances). The IADL score ranges from 0 to 8 (good independent living skills).
Table 2 presents the adjusted mean observed for nutritional outcomes, for each measurement time and for each group and table 3 presents the results of the linear mixed model. According to the linear mixed model analysis, the control group displayed a higher MNA score than the experimental group, in line with the difference observed at baseline between the groups. A significant increase of weight and an almost significant increase of MNA score were observed at t4 compared to t0 for both groups. At t4, the experimental group tended to have a higher calorie ratio than the control group. At t2, the experimental group had a significant higher protein ratio than the control group. According to a contrast comparison (within-group comparison), a significant increase was observed in the experimental group for the calorie ratio between t0 and t2 (+21%, p<0.05) and between t0 and t4 (+26%, p<0.001), as well as for the protein ratio between t0 and t2 (+28%, p<0.001) and between t0 and t4 (+26%, p<0.05). No significant change was observed in the control group for the calorie and protein ratios.
Table 2
Evolution of the outcome measurements during the follow-up in the control and experimental groups (adjusted means from the linear mixed model are presented with their Standard Error in brackets)
MNA Mini Nutritional assessment.
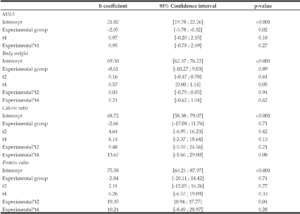
Table 3
Results of the linear mixed model with group, time and interaction group*time as fixed effect, and participants as random factor
MNA Mini Nutritional assessment.
Discussion
The objective of the present pilot trial was to assess the feasibility and effectiveness of a personalised dietary intervention in older people receiving meals-on-wheels. Compared to the control group, the intervention allowed older people of the experimental group to increase their protein ratio and to a lesser extent their calorie ratio. Overall, enrichment was well accepted by the participants. Only one participant has initially refused the supplementation, but he ended-up to accept it after t2. Enrichment was adjusted to the initial food intake and the food preferences of the participants. The enrichment method that was favoured at first instance was meal fortification, namely adding high- calorie/high-protein ingredients to regular meals (i.e. adding a slice of ham; adding cheese to soup). Fortification was combined with ONS to achieve higher enrichment levels in some older people, particularly in very small eaters (23,24). However, for very small eaters (calorie and/or protein ratios < 66%), meal enrichment was not sufficient to compensate for their nutritional deficit. This highlights the need to further develop food products to enrich the older people’s meals to improve their nutritional intake.
In accordance with previous studies, the present results confirm the high prevalence of malnutrition risk in older people with meals-on-wheels services (3,4). At baseline, 80% of the participants were at risk of malnutrition. This prevalence is associated with very low food intake: 55% of the participants ate less than 2/3 of their calorie and/or protein allowance.
Limitations of the present study
Despite these encouraging results, this study had several limitations. From a methodological point of view, the present experiment highlights several bottlenecks to be faced when running a field study with older people receiving meals-on-wheels. First, we experienced an important dropout rate after four months of follow-up (45%; n=27/60). The reasons for dropout were mainly a deterioration in health, functional and/or cognitive status. Other studies conducted on meals-on-wheels recipients have also reported quite high dropout rates: 13% after 1 week in Silver et al (2008) and 29% after 12 weeks of follow-up in Arjuna et al (2018). In the present study, the dropout rate may have been worsened by the fact that the participants were recruited from the population receiving the meals-on-wheels service provided by the social action center of Paris, which is composed mostly of older people with a low socio-economic status. At baseline, 55% of the participants indicated that they had low financial resources and 40% had a low level of education (primary school). Previous studies have suggested that involving participants with a low socio-economic status in research trials is 5 to 6 times harder than involving of participants with an intermediate socio-economic status (25,26).
A second challenge was to record food intake. Sun et al. (27) showed that a 3-days recall was reliable to assess energy intake in homebound older people. However, in the present experiment, we felt that the burden of a 3-day recall would have been too high considering the frailty and fatigability of our target population (see also 7,10,11). However, several actions have been taken to ensure as far as possible accurate food intake measures. The dietician called the participant the day before the 24-hour record day to remind him/her to write down everything he/she ingests the next day. When participants had trouble remembering what they had eaten the day before, the dietician looked at the leftovers in the fridge. In addition, the measure was somehow facilitated by the fact that the dietician knew the type and the quantity of food that was delivered to the participant. Anyway, a critical issue for future researches in this population will be to develop easy-to-use automatic design to record food intake (28).
Finally, at baseline, participants from the control group displayed a higher MNA score and a better nutritional status than participants from the experimental group. This may have biased the between-group comparison.
Conclusion
To conclude, this study suggests that providing dietary guidance and adding nutrient-dense food to meals while considering food preferences is feasible and may help older beneficiaries of meals-on-wheels to increase their calorie and protein intakes. However, there is a need to develop products or recipes to enrich the meals of the elderly more efficiently to achieve the recommended allowance. The potential role of the meals-on-wheels service associated with dietary guidance and meal adjustment in the prevention of malnutrition in the dependent older adult population deserves further investigations through a well-powered randomized controlled trial.
Acknowledgement: This study is part of RENESSENS funded by the French National Research Agency (ANR-13-ALID-0006-02). This work was also supported by grants from the Regional Council of Burgundy France (PARI Agral 1) and the European Funding for Regional Economical Development (FEDER). This work was carried out with the invaluable help of Claire Chabanet for the statistical analyses.
Conflicts of Interest: This work was carried out within the framework of the CIFRE agreement N°1576. Ségolène Fleury’s doctoral contract was thus financed by the company Saveurs et Vie, of which Paul Tronchon and Stéphanie Roux are members. The academic supervision of this thesis is carried out by Claire Sulmont-Rossé and Virginie Van Wymelbeke.
Ethical standard: All procedures performed in the studies were in accordance with the ethical standards of the institutional research committee and with the declaration of Helsinki and its later amendments. Informed consent was obtained from all individual participants included in the studies.
ClinicalTrials.gov: NCT02866474
References
1. Cardon P, Gojard S. Les personnes âgées face à la dépendance culinaire : entre délégation et remplacement. La Documentation française | « Retraite et société ». 2009;2008/4(56):170.
2. Maurel E, Boulegue A, Faibis L. Le marché du portage de repas à domicile à l’horizon 2020 : pressions sur les prix, nouveaux entrants, montée en gamme de l’offre : quels leviers et perspectives de croissance ? Paris: Xerfi; 2018.
3. Maitre I, Van Wymelbeke V, Amand M, Vigneau E, Issanchou S, Sulmont-Rossé C. Food pickiness in the elderly : Relationship with dependency and malnutrition. Food Quality and Preference. 2014 Mar;32:145–51.
4. Crichton M, Craven D, Mackay H, Marx W, de van der Schueren M, Marshall S. A systematic review, meta-analysis and meta-regression of the prevalence of protein-energy malnutrition: associations with geographical region and sex. Age and Ageing. 2018 Sep;
5. IJmker-Hemink VE, Dijxhoorn DN, Briseno Ozumbilla CM, Wanten GJ, van den Berg MG. Effective elements of home-delivered meal services to improve energy and protein intake : A systematic review. Nutrition. 2020 Jan;
6. Kretser AJ, Voss T, Kerr WW, Cavadini C, Friedmann J. Effects of two models of nutritional intervention on homebound older adults at nutritional risk. J Am Diet Assoc. 2003 Mar;103(3):329–36.
7. Gollub EA, Weddle DO. Improvements in nutritional intake and quality of life among frail homebound older adults receiving home-delivered breakfast and lunch. Journal of the American Dietetic Association. 2004 Aug;104(8):1227–35.
8. Charlton KE, Walton K, Moon L, Smith K, Mcmahon AT, Ralph F, et al. ‘It could probably help someone else but not me’: A feasibility study of a snack programme offered to meals on wheels clients. J Nutr Health Aging. 2013 Apr;17(4):364–9.
9. Denissen KFM, Janssen LMJ, Eussen SJPM, van Dongen MCJM, Wijckmans NEG, van Deurse NDM, et al. Delivery of nutritious meals to elderly receiving home care: Feasibility and effectiveness. The journal of nutrition, health & aging. 2017 Apr;21(4):370–80.
10. Arjuna T, Miller M, Ueno T, Visvanathan R, Lange K, Soenen S, et al. Food Services Using Energy- and Protein-Fortified Meals to Assist Vulnerable Community-Residing Older Adults Meet Their Dietary Requirements and Maintain Good Health and Quality of Life: Findings from a Pilot Study. Geriatrics. 2018 Sep 12;3(3):60.
11. Ziylan C, Haveman-Nies A, Kremer S, de Groot LCPGM. Protein-Enriched Bread and Readymade Meals Increase Community-Dwelling Older Adults’ Protein Intake in a Double-Blind Randomized Controlled Trial. J Am Med Dir Assoc. 2017 Feb 1;18(2):145–51.
12. Lipschitz D, Mitchell C, Steele R, Milton K. Nutritional-Evaluation and Supplementation of Elderly Subjects Participating in a Meals on Wheels Program. J Parenter Enter Nutr. 1985;9(3):343–7.
13. Hill GJ, Gorman MA, Simon S, Frawley L, Whitten K, Wanner L, et al. Effectiveness of Oral Nutritional Supplement Use on Nutritional Status of Community-Dwelling Elderly Receiving Home-Delivered Meals. Journal of the Academy of Nutrition and Dietetics. 2012 Sep 1;112(9):A96.
14. Folstein MF, Folstein SE, McHugh PR. “Mini-mental state”. Journal of Psychiatric Research. 1975 Nov;12(3):189–98.
15. Lawton MP, Brody EM. Assessment of Older People: Self-Maintaining and Instrumental Activities of Daily Living. 1969;8.
16. Bauer J, Biolo G, Cederholm T, Cesari M, Cruz-Jentoft AJ, Morley JE, et al. Evidence-based recommendations for optimal dietary protein intake in older people: a position paper from the PROT-AGE Study Group. Journal of the American Medical Directors Association. 2013 Aug;14(8):542–59.
17. Sulmont-Rossé C, Van Wymelbeke V. Les déterminants d’un apport protidique faible chez les personnes âgées dépendantes. Cahiers de Nutrition et de Diététique. 2019 Jun;54(3):180–9.
18. Guigoz Y, Lauque S, Vellas BJ. Identifying the elderly at risk for malnutrition The Mini Nutritional Assessment. Clinics in Geriatric Medicine. 2002;
19. Ciqual French food composition table [Internet]. 2016. Available from: https://ciqual.anses.fr/
20. HAS. Stratégie de prise en charge en cas de dénutrition protéino-énergétique chez la personne âgée. Médecine des Maladies Métaboliques. 2007 Nov;1(4):92–6.
21. Deutz NEP, Bauer JM, Barazzoni R, Biolo G, Boirie Y, Bosy-Westphal A, et al. Protein intake and exercise for optimal muscle function with aging: Recommendations from the ESPEN Expert Group. Clinical Nutrition. 2014 Dec;33(6):929–36.
22. Guide pratique du poids des vêtements et tissus en machine : jean, serviette, t-shirt…. IDEAL. [consulted 2018 June]. Available from: https://www.ideal.fr/guide/poids-et-quantite-de-linge/
23. Seguy D, Hubert H, Robert J, Meunier JP, Guérin O, Raynaud-Simon A. Compliance to oral nutritional supplementation decreases the risk of hospitalisation in malnourished older adults without extra health care cost: Prospective observational cohort study. Clinical Nutrition. 2019 Aug 17;
24. Smith TR, Cawood AL, Walters ER, Guildford N, Stratton RJ. Ready-Made Oral Nutritional Supplements Improve Nutritional Outcomes and Reduce Health Care Use-A Randomised Trial in Older Malnourished People in Primary Care. Nutrients. 2020 Feb 18;12(2).
25. Darmon N, Lacroix A, Ruffieux B. Experimental economics shows how food price policies may improve diet while increasing socioeconomic inequalities in nutrition. Working paper INRA, UMPF. 2011;
26. Ruffieux B. Évaluation par l’économie expérimentale de politiques nutritionnelles de prix et d’information. Internal workshop presented at; 2010 May; Dijon France.
27. Sun Y, Roth DL, Ritchie CS, Burgio KL, Locher JL. Reliability and Predictive Validity of Energy Intake Measures from the 24-Hour Dietary Recalls of Homebound Older Adults. Journal of the American Dietetic Association. 2010 May;110(5):773–8.
28. Astell AJ, Hwang F, Brown LJE, Timon C, Maclean LM, Smith T, et al. Validation of the NANA (Novel Assessment of Nutrition and Ageing) touch screen system for use at home by older adults. Experimental Gerontology. 2014 Dec;60:100–7.