M.E.L. van den Berg1, M. Crotty1
1. Flinders University, School of Medicine, Dep of Rehabilitation, Aged & Extended Care, Adelaide, Australia
Corresponding Author: Dr Maayken van den Berg, Flinders University, School of Medicine, Dep of Rehabilitation, Aged & Extended Care, Repatriation General Hospital, Daws Road, Daw Park l South Australia l 5041, E: maayken.vandenberg@flinders.edu.au, T: +61 8 8275 1297 l F: +61 8 8275 1130
Abstract
Background: Decline in mobility is commonly observed following stroke. Reducing the impact of stroke is key to the maintainance of functional independence. Objectives: To determine the acceptability and adherence of a water-based exercise program post-stroke. Design: A single-blind randomised controlled pilot study with masked outcome assessment. Setting: Rehabilitation Unit, Adelaide, South Australia. Participants: 22 community-dwelling older people e living with strokes (6 months-3 years post-stroke). Intervention: Subjects were randomized to either: a six-week water-based intervention group (WG), thrice- weekly; a six-week gym-based intervention group (GG), thrice-weekly; or a six-week chronic disease self-management course (CG), once-weekly. Measurements: Assessments took place at baseline, post-intervention and at 3 months follow-up. Primary outcome measures was the 6-minute walk test. Secondary outcomes were measures of balance, body composition, cognition, ADL, goal attainment, quality of life, sleep and fatigue. Results: Recruitment was difficult with only 20% of those approached meeting entry criteria and consenting. A larger increase in walking speed and reduced use of walking aids post-intervention was observed in the WG, however, differences between groups were not significant. No between-group differences were found for any secondary outcomes. The average attendance rate was 90% (n=6). Conclusion: Subjects tolerated the moderate to high intensity water-based exercise program and adherance was good. Although we can not draw firm conclusions due to study completion failure the results suggest that a relatively short program of water-based exercise in stroke survivors is safe and feasible and can improve functional mobility. Hydrotherapy can be delivered with minimal supervision and a well powered trial is needed to assess the effects in chronic stroke patients
Key words: Stroke, water-based exercise, mobility, randomised controlled trial.
Introduction
There are approximately 48.000 stroke events amongst Australians each year. It is the second cause of disease burden in Australia, in terms of ‘healthy’ life lost due to poor health or disability (1). Loss or limitation of functional movement is a common consequence of stroke. Around 21% will experience a decline in mobility in the first three years which leads to a disruption in usual functioning (2). Reducing the impact of stroke is the key to maintenance of independence and quality of life.
The benefits of water-based exercise have been demonstrated in patients with a range of conditions such as rheumatoid arthritis , osteoarthritis , fibromyalgia and also in the general older adult population (3). Additionally, previous studies have shown high levels of adherence with water-based exercise (4). Water-based exercise is possible for patients who are non-ambulatory or have balance issues however there is little evidence supporting water-based exercises after stoke. The objective of this study was to assess the acceptability and adherence of a water-based exercise program in individuals six months to three years post-stroke. Given the susceptibility to deterioration of functional mobility after stroke, succesful completion of this study was to inform a future trial. It was anticipated that the water environment would allow patients to exercise at a higher level than would have been possible on land, translating into greater improvements to function.
Methods
Procedure
This was a single blind randomised controlled pilot study with masked outcome assessments. Participants were recruited via the rehabilitation service at the Repatriation General Hospital and key inclusion criteria were: six months to three years since first stroke; community dwelling; independent ambulation with or without gait aids; Mini Mental State Exam score of at least 18; ability to accept instruction and able to give consent. Reasons for exclusion were: subsequent stroke; major medical complications following stroke; unstable cardiac conditions; urinary or fecal incontinence; open wounds; tinea; unstable epilepsy or seizures; other comorbid conditions that might contraindicate participation in gym- or water-based exercise; inability to carry out the exercise program; and current participation in a concurrent exercise program.
All eligible participants willing to take part in the study provided written informed consent and were then randomized to receive either: a six-week water-based exercise intervention (3 times/week); a six-week gym- based exercise intervention (3 times/week); or no exercise intervention (waiting list control). Random group allocation was centrally managed by a pharmacist external to the project. Randomisation was generated by a computer software program.
Intervention
The water-based intervention group (WG) received three pool sessions per week for a total of six weeks. Each session was of 40 minutes duration (including aerobic warm up and stretching cool-down) and consisted of a standardised resistance program. Exercises included sideways walking, hip flexion, hip extension, hip adduction, and hip abduction, knee cycling, calf raises, upper body resistance exercises. The intensity of which varied according to each individual’s ability, with progressive increase in load over the six week period. Likewise, the gym-based intervention group (GG) received three 40-minute gym sessions (including aerobic warm-up and stretching cool-down) per week for a total of six weeks following a standardised resistance program of which the intensity varied according to each individual’s ability, with progressive increase in load over the six week period. Exercises included: bike and arm ergometers, seated bench press, hipflexion, hip extension, hip adduction and hip abduction, triceps pull-down and knee flexion and knee extension. The no-exercise control group (CG) attended a chronic disease self-management course once a week for six weeks. Each session was of 2.5 hours duration and focused on topics such as: symptom management; effective communication with your doctor; and how to lessen frustration, fight fatigue, make daily tasks easier and get more out of life.
Assessments
Assessments took place at baseline, immediately post- intervention at 6 weeks and at 3 months follow-up. The primary outcome was gait performance as measured by the six minute walk test (6MTW) (5). Secondary outcome measures were the Modified Berg Balance Scale (MBSS) (6), bioelectrical impedance, Mini Mental Status Examination (MMSE) (7), Modified Barthel Index (MBI) (7), Goal Attainment Scale (GAS)(8), SF-36 (7), Motor Assessment Scale (MAS) (9), MOS Sleep Scale (10), and 10-item Fatigue Assessment Scale (11). Data on demographics (sex, age, etc.), medical history and medications were collected from medical case records or from the
subject at baseline. Side effects were monitored but none were reported
Stastictical analysis
Primary analysis for this trial was undertaken using intention to treat principles. Due to the small sample size, non-parametric statistics was used for data analysis. The one-way analysis Kruskall-Wallis test for independent samples was used to determine if there was a statistically significant difference between the groups.
Results
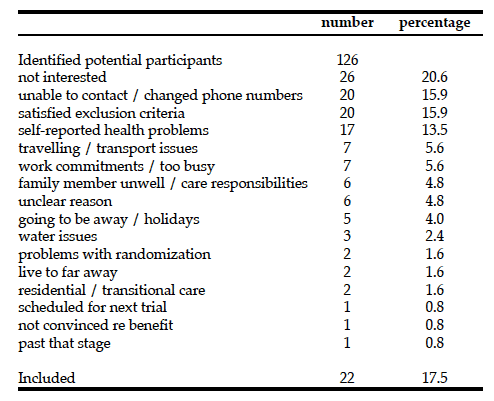
Recruitment commenced in December 2007 and ceased in July 2008. Twenty (16%) of the potential participants could not be contacted (e.g phone cut off or phone not aswered). A total of 106 stroke survivors were approached
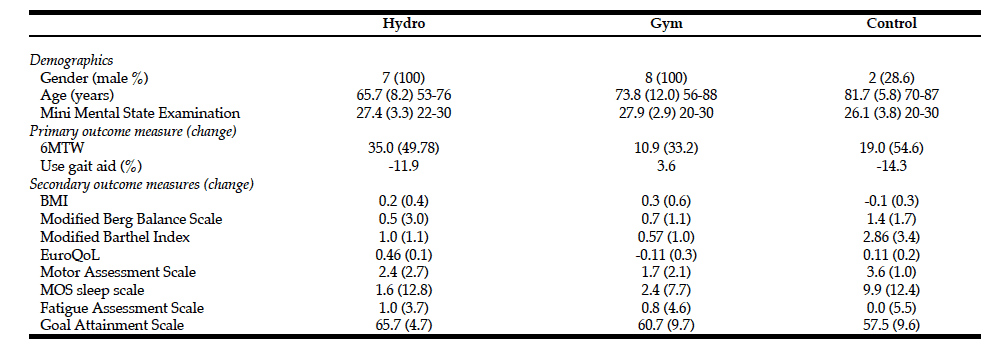
for the study. Please refer to Table 1 for detailed information on recruitment. A total of 22 (20%) of the patients approached consented and were randomised. Patients characteristics are shown in Table 2. There were 2 withdrawals, 1 in the GG and 1 in the CG. The remaining 20 participants were followed up at the 6- week post-intervention assessment. However, the study was terminated prior to the scheduled end date due to funding difficulties and follow-up data at 3 months was collected of 6 patients only. As a result of premature abortion planned sample size could not be achieved and data collection could not be completed.
The exercise intervention was standardized for all subjects, consisting of resistance exercises performed in either the gym or pool. Exercises essentially exerted the same muscle groups in subjects regardless of randomisation to the pool or gym. Variance of intensity (low/medium/high) depended on an individual’s ability, however during the intervention period the training load was progressively increased according to the principle of progressive overload (Kraemer).
Study outcomes are presented in Table 3. A larger improvement in gait performance on the 6MTW was evident post-intervention and a reduced use of walking aids was observed in the WG. However, significant differences between groups were not present. A noteworthy improvement in optimal sleep was observed in the WG as measured with the MOS Sleep Scale. The GAS scores indicated that the WG evaluated themselves best on overall achievement of personal set goals. No significant differences were observed between groups in any of the secondary outcome measures.
Adherence was monitored for 6 participants in the WG and the average attendance rate was 90%.
Discussion
We compared water-based therapy to gym-based therapy and no exercise intervention. We demonstrated the feasibility of our protocol in that subjects could tolerate moderate to high intensity exercise programs using a water-based program. Also, the results suggest that a relatively short program of water-based exercise can improve functional mobility in stroke survivors. Although we cannot draw firm conclusions due to the fact that the study was aborted to completion, studies with small samples add to the body of literature and should contribute to meta-analysis efforts. Accordingly, we hope that the presented data will be used in future meta-analyses which will overcome the limitation of small sample size by pooling study results to generate a single best estimate.
Water-based exercise is considered to be a safe and effective alternative to land-based exercise. Very few studies have been conducted water-based exercises in stroke survivors and only one (12) has measured gait performance. In this study with 12 community-dwelling individuals treatment effects on gait performance were significantly in favour of water-based exercises compared to no-water based exercises (12). Our study results show a trend towards improved walking performance in the WG, however due to the small sample size results did not reach significance and definite conclusions can not be drawn.
Subjects in the WG trained 3 times a week for 40 min and exercised mainly at 50-60% of their baseline age- predicted HR maximum without discomfort. This is consistent with the recommendations by the American Heart Association (13) who prescribes exercise in stroke patients at 50-80% of maximal heart rate, 3-7 days a week with a duration of 20-60 min/day. However, to elicit a training effect increasing the dose may yield better results (14). Studies that have previously shown improvements are based on either 8 or 12-week training programs (15, 16). Adherence was good with a 90% attendance rate in the WG. Due to the physical properties of water, such as buoyancy and hydrostatic pressure, the greater variety of movements, easy-to-do low-impact exercise, pleasant recreational environment and reduced fear of falling may encourage adherence to the training program.
In summary, subjects tolerated the program and the findings of the pilot study are promising considering the relatively short length of the program and incomplete study results. A well powered trial is needed to assess the effectiveness of a water-based exercise program poststroke.
Based on the findings of this pilot study we recommend that a sample size of 152 subjects is required to detect a minimal clinically important difference of 50m (17), based on a two-tailed test at 0.80% power and a significance level of 0.05.
Acknowledgements: We acknowledge the help of the patients and hospital staff. We also thank Repatriation Research Foundation for funding.
Funding: This study was sponsored by The Foundation Daw Park Grants for Medical Research (2007/2008). The sponsor had no role in the design and conduct of the study; in the collection, analysis, and interpretation of data; in the preparation of the manuscript; or in the review or approval of the manuscript.
Conflict of interest disclosure: Dr Maayken van den Berg is not aware of any conflict of interest. Prof Maria Crotty is not aware of any conflict of interest.
References
1. Australian Institute if Health and Welfare: Senes S. How we manage stroke in Australia. Canberra: Australian Institute of Health and Welfare, 2006.
2. van de Port I, Kwakkel G, van Wijk I, Lindeman E. Susceptibility to Deterioration of Mobility Long-Term After Stroke A Prospective Cohort
Study. Stroke. 2006;37(1):167-71.
3. Geytenbeek J. Evidence for effective hydrotherapy. Physiotherapy. 2002;88(9):514-29.
4. Foley A, Halbert J, Hewitt T, Crotty M. Does hydrotherapy improve strength and physical function in patients with osteoarthritis—a randomised
controlled trial comparing a gym based and a hydrotherapy based strengthening programme. Annals of the rheumatic diseases. 2003;62(12):1162-7.
5. Pohl P, Duncan P, Perera S, Liu W, Lai S, Studenski S, et al. Influence of stroke-related impairments on performance in 6-minute walk test. Journal of rehabilitation research and development. 2002;39(4):439-44.
6. Berg K, Wood-Dauphinee S, Williams J, Maki B. Measuring balance in the elderly: validation of an instrument. Canadian journal of public health Revue canadienne de sante publique. 1992;83:S7.
7. Duncan P, Jorgensen H, Wade D. Outcome measures in acute stroke trials a systematic review and some recommendations to improve practice. Stroke. 2000;31(6):1429-38.
8. Kiresuk T, Smith A, Cardillo J. Goal attainment scaling: Applications, theory, and measurement: Lawrence Erlbaum Associates, Inc; 1994.
9. Carr J, Shepherd R, Nordholm L, Lynne D. Investigation of a new motor assessment scale for stroke patients. Physical therapy. 1985;65(2):175-80.
10. Hays R, Martin S, Sesti A, Spritzer K. Psychometric properties of the Medical Outcomes Study Sleep measure. Sleep medicine. 2005;6(1):41.
11. Michielsen H, De Vries J, Van Heck G. Psychometric qualities of a brief selfrated fatigue measure: The Fatigue Assessment Scale. Journal of
Psychosomatic Research. 2003;54(4):345-52.
12. Chu K, Eng J, Dawson A, Harris J, Ozkaplan A, Gylfadóttir S. Water-based exercise for cardiovascular fitness in people with chronic stroke: a
randomized controlled trial. Archives of physical medicine and rehabilitation. 2004;85(6):870-4.
13. Gordon N, Gulanick M, Costa F, Fletcher G, Franklin B, Roth E, et al. Physical activity and exercise recommendations for stroke survivors an American heart association scientific statement from the council on clinical cardiology, subcommittee on exercise, cardiac rehabilitation, and prevention; the council on cardiovascular nursing; the council on nutrition, physical activity, and metabolism; and the stroke council. Circulation. 2004;109(16):2031-41.
14. Cooke E, Mares K, Clark A, Tallis R, Pomeroy V. The effects of increased dose of exercise-based therapies to enhance motor recovery after stroke: a systematic review and meta-analysis. BMC medicine. 2010;8(1):60.
5. Duncan P, Richards L, Wallace D, Stoker-Yates J, Pohl P, Luchies C, et al. A randomized, controlled pilot study of a home-based exercise program for individuals with mild and moderate stroke. Stroke. 1998;29(10):2055-60.
16. Duncan P, Studenski S, Richards L, Gollub S, Lai S, Reker D, et al. Randomized clinical trial of therapeutic exercise in subacute stroke. Stroke.
2003;34(9):2173-80.
17. Perera S, Mody S, Woodman R, Studenski S. Meaningful change and responsiveness in common physical performance measures in older adults.
Journal of the American Geriatrics Society. 2006;54(5):743-9.