R. Billon1, J.-L. Fanon2, P. Thomas3
1. Pôle de Gérontologie Clinique, unité de Court Séjour Gériatrique, Centre Hospitalier de La Rochelle, France; 2. Pôle de Gérontologie Clinique, Centre Hospitalier Universitaire, Fort de France Martinique, France; 3. Psycho-Gériatrie, SHU Limoges, France
Corresponding Author: Dr Rémy Billon, unité de Court Séjour Gériatrique, Centre Hospitalier de La Rochelle, 17000 La Rochelle, France, remy.billon@ch-larochelle.fr
Abstract
Objectives: To appraise the risk of having a multi resistant bacteria infection attributable to poor nutritional status
in the elderly. Design: Using a statement from a case-control study in an acute geriatric medical service, knowing the overall risk of infection in the studied population, it is possible from the likelihood ratio, frequency of malnourished infected by MRB, divided by frequency in malnourished infected with sensitive organisms, to calculate a probability which is a post-test assessment of this risk. Two groups of patients had a documented infection, one with both an albumin less than 25g and pre albumin levels less than 0.15g and another where values were greater than or equal to 35g and 0.15g. Setting: The geriatrics short care unit in Fort de France, Martinique, France. Participants: Patients over 75 years, hospitalized in the short care unit and who had an acute infection with a positive sample (urine, blood .. ). Measurements: The frequency of malnourished patients is increased when infected with multi-resistant Bacteria, as shown with post test probability calculation. Results: In a population averaging 85 years old, the malnourished group had almost a double risk of infection , 26.92% ( 95% CI : 22.73-30.38 ) against 13.95% ( 95% CI : 7.01-25.85) in the other group. The fraction attributable to undernutrition was 48%. Conclusion: Nearly half of the resistance can be attributed to malnutrition with a fraction attributable to exposure to 48%. It’s still possible that other factors not taken into account in this presentation partly explain this difference. The case-control statement type can also be biased and finally we relied only on the rate of albumin and pre-albumin to classify patients. But it is still unlikely that the observed result is due to chance.
Key words: Multi-resistant bacteria infection, risk, undernutrition, elderly.
What this paper adds : 1) What is already known on this subject : we know that one of the consequences of undernutrition is an increased risk of infectious episodes, more frequent and severe. 2) What does this study adds : an appraisal of the link between undernutrition in the elderly and risk of infections due to multi-resistant bacteria, that was not pointed in the current medical literature.
Introduction
The prevalence of malnutrition in elderly patients admitted to hospital is high. It varies depending on the studies and the methods of evaluation of undernutrition and may range from 16 to 90% (3, 4, 6-9, 13, 14). A consequence is the affection of the immune system and therefore an increased risk of infectious episodes more frequent and severe (10-12).
The quantitative impact of malnutrition on the excess risk of multidrug-resistant bacterial (MRB) infections is less well known. A literature search made with pubmed using the terms “multi-drugs resistant infections” and “malnutrition” revealed only a few studies of which none focuses on the elderly. We tried in this work to estimate the risk and therefore how many acute infections caused by multiresistant bacteria could be attributed to malnutrition.
Methods
Measurement of a risk of infection involves specific conditions. Ideally, the determination is made by following a malnourished population in which the incidence of infections is raised.
In a medical service, such work is not possible. Patients who arrive are often already infected and we can only assess the nutritional status of these patients. We are in terms of a case-control study that allows the measurement of an odds ratio but not a risk. But the risk is that of having a well-defined disease (MRB infection) when evaluating patients shows that they are positive for a test, which, in this presentation, is screened for malnutrition. This is a post-test probability. When you know the risk of infection resistant bacteria in the population from which is extracted the study sample (pre-test probability), then we can calculate this post-test probability that is a risk. For this we calculate the pretest odds by pre-test probability divided by 1-pretest probability, which is multiplied by the likelihood ratio, frequency of malnourished infected with resistant bacteria divided by frequency in case of infection not germ resistant. One obtains a post test odds that divided by 1 + post-test odds for the post-test probability gives the sought for risk (2).
Patients over 75 years, hospitalized in the Geriatrics Short Care Unit in Fort de France (Martinique) and who had an acute infection with a positive sample (urine, blood .. ) were included. Their consent to participate in this study was obtained in writing. Those who had on entry into the service chronic infection or acute evolving over 48 h were excluded because the inflammation could over disturb the determination albumin and pre albumin. As it was still difficult to ascertain the nature of the acute infection, to identify a possible interaction, that is to say, a different result depending on the inflammatory status, we planned to repeat the calculation for this study in two groups, one with marked inflammatory balance and one with less inflammation.
Were considered multi-resistant germ infections, those with a resistance to several classes of antibiotics and reported as such by the microbiology laboratory.
The biological nutrient assessment was done systematically in all patients with albumin, pre-albumin, C-reactive protein (CRP), orosomucoid and Prognostic Inflammatory and Nutritional Index (PINI). From our experience, we know that the prevalence of malnourished patients is very high in the hospitalized elderly populations in Martinique. It appeared to be difficult to obtain a large enough group with a really normal nutritional status. For this reason, we decided to set the cutoff for a weak or non-existant malnutrition thresholds to albumin greater than and equal to 35 grams and pre albumin greater than or equal to 0.15 grams. This group had to be compared to another having both albumin less than 25 grams and a rate of pre albumin less than 0.1 grams.
This work was done in the
acute geriatric medicine department of the University Hospital of Fort de France, Martinique prospectively from January 2007 to July 2012.
The post-test probabilities and their confidence intervals were calculated with Winpepi module, screening and diagnostic tests (Fleiss Levin-Paik method) (1).
Results
During the study period, 405 patients had a documented acute infection and a complete nutritional assessment. One hundred and thirty had both an albumin greater than 35 g and a pre albumin greater than 0.15g, of which only six had a really normal balance and forty three had both an albumin level less than 25 g and a pre albumin less than 0.1 g. Other patients were not included for this study. One hundred and seventy three patients had the predefined criteria. Mean age was 84.86 years (n = 342, SD: 7.38), 86.08 years for females (n = 87, SD: 6.99) and 83.02 years for males (n = 57, SD: 7.62).
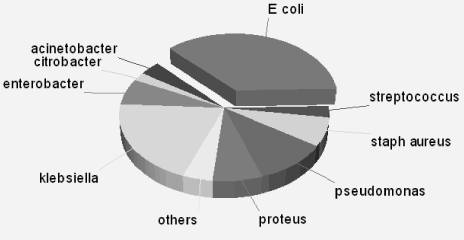
E. coli was the most frequent bacteria (36.8%) followed by Klebsiella (20.14%), Pseudomonas (10.42%) and to a lesser extent, Staphylococcus aureus (6.94%) and Enterobacter (6.25%) (Figure 1).
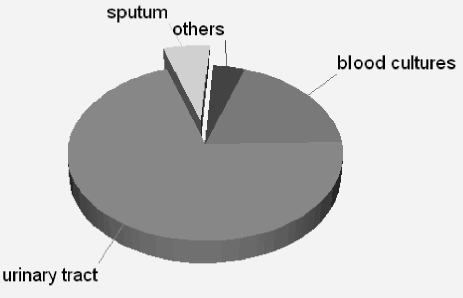
Infections were predominantly from urine (70.34%) or found on blood cultures (19.31%) (Figure 2).
In the sample studied, 23.7% had MRB infection, which was our pre-test probability and among these, 85.37% were in the group most malnourished. 71.97% were in the non-resistant infection group.
The links between multidrug resistance and age, albumin, pre albumin, CRP, orosomucoid and PINI were studied in two predefined sub-groups (Table 1). Only age differed in the two groups (p = 0.031) with lower values in case of infection MRB (83.098 versus 86.583 years). None of the other variables obtained significance only.
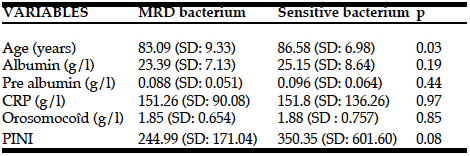
Table 1: Comparison of the biological variables of the nutritional assessment according to the infection is due to a multiresistant bacterium or not
For patients with both low albumin and pre albumin, the post test probability, so the risk of infection MRB, was 26.92% (95% CI: 22.73 – 30.38). Probability was 13.95% (95% CI :7.01-25 .85) for the better nourished, which means a doubled risk.
The calculation was redone, according to whether the CRP was greater than or equal to 80 or less. In the case of intense inflammatory post-test probability is 25.27% and 26.32% in the case of
lower value, so values close to the overall risk that is 26.92%.
The fraction attributable to exposure (malnutrition) is 26.92-13.95/26.92 = 0.48 or 48%.
The population attributable fraction was 23.7 (pretest probability our) -13.95/23.7 = 0.41 or 41%.
Discussion
In this study, the risk of infection resistant bacteria is two times higher in the group most malnourished.
Nearly half of the resistance can be related to malnutrition, a little less when risk is calculated on population (41%). This latter value is due to the high percentage of malnourished in our service. In a place where nutritional status is better, the population attributable fraction would have been lower. At the extreme, in the absence of nutritional deficiency, the post- test probability would have been 13.95% and in this case the attributable fraction is zero.
We cannot say, however, that if they had not been malnourished, they would have totally avoided the risk, which is an estimate of the maximum fraction that could have been prevented. There may be confounding factors not taken into account here.
Albumin and pre albumin levels were used to classify patients, and we know they do not have perfect sensitivity and specificity for diagnosing undernutrition (5). In particular, associated pathologies and inflammatory conditions can influence their level regardless of their actual status. Chronic infectious states were excluded, but patients arriving with a high inflammatory state may have been influenced with a consequent misclassification.
Calculations made depending on the inflammatory status are close and even with an important inflammatory syndrome, the risk of infection MRB is just near identical. So even if surprising, the value is slightly lower when there is marked inflammation, when the opposite would be expected. Yet, the samples are smaller and therefore more random. It is possible that the inflammation lowered 4 days ago … it would be degraded in fat or leastways degraded in vivid fat, then would be degraded in center and farm values of inflammatory proteins and removed from the best fed group of people who should behave been in it. The risk then declined somewhat since these patients were less susceptible.
We also note that the confidence intervals of risk depending on whether one is malnourished or not overlap: respectively 22.73-30.38 versus 7.01-25.85. It is still possible that this result is due to chance, but the odds are very low and we believe that it is rather due to a lack of power. With an effective upper, confidence intervals were narrower. One can also think that if we had had a group with a strictly normal nutritional status, the difference would have been more clear.
Finally, in this case-control study, the results may have been the effect of confounding unexpected factors.
It is also surprising that the bivariate analysis of 2 predefined groups’ variables does not show significant difference, even if there is a quantitative difference both for the albumin and for prealbumin. We estimate that this difference would have been significant for a twice as important sample, especially for albumin. Besides, we used a two-tailed test, and if we consider that the expected difference always has to go to the same direction, a one-tailed test would have been able to be used and would have divided p by 2. It is thus probably about a lack of power.
Conclusion
Despite the bias that can be attributed to this study, we conclude that malnutrition not only increases the risk of infection, but also exposes to double risk of multi resistant bacillus (26.92% against 13.95%) compared to people in better nutritional status. It remains to be confirmed on a larger scale and probably multicenter compared with a normal population nutritional status.
Acknowledgements: the authors wish to thank Steve Burrough who so graciously contributed to the achievement of this work. This work complies with the current laws of France.
Conflict of Interest Statements: We declare that we have no conflicts of interest
References
1. Abramson JH. WINPEPI updated: computer programs for epidemiologists, and their teaching potential. Epidemiol Perspect Innov 2001;8:1
2. Abramson JH, Abramson ZH. Making sense of data : a self-instruction manual on the interpretation of epidemiological data. Oxford University Press, Oxford ; New York, 2001
3. Amaral TF, Matos LC, Teixeira MA et al. Undernutrition and associated factors among hospitalized patients. Clin Nutr 2010;29:580-585
4. Ashby DR, Ford HE, Wynne KJ et al. Sustained appetite improvement in malnourished dialysis patients by daily ghrelin treatment. Kidney Int 2009;76:199-206
5. Bouillanne O, Hay P, Liabaud B et al. Evidence that albumin is not a suitable marker of body composition-related nutritional status in elderly patients. Nutrition 2001;27:165-169
6. Cansado P, Ravasco P, Camilo M. A longitudinal study of hospital undernutrition in the elderly: comparison of four validated methods. J Nutr Health Aging 2009;13:159-164
7. Coelho AK, Rocha FL, Fausto MA. Prevalence of undernutrition in elderly patients hospitalized in a geriatric unit in Belo Horizonte, MG, Brazil. Nutrition 2006;22:1005-1011
8. Constans T, Alix E, Dardaine V. [Protein-energy malnutrition. Diagnostic methods and epidemiology]. Presse Med 2000;29:2171-2176
9. Fuchs V, Mostkoff D, Salmean GG et al. [Nutritional status in hospitalized patients in a public hospital in Mexico City]. Nutr Hosp 2008;23:294-303
10. Michel JP, Lesourd B, Conne P et al. Prevalence of infections and their risk factors in geriatric institutions: a one-day multicentre survey. Bull World Health Organ 1991;69:35-41
11. Ramos Martinez A, Asensio Vegas A, Nunez Palomo A et al. [Prevalence and risk factors associated to malnutrition in elderly inpatients]. An Med Interna 2004;21:263-268
12. Ramos Martinez A, Luna Garcia R, Gonzalez Sanchez J et al. [Malnutrition at an internal medicine service: impact of patients coming from homes for the elderly]. An Med Interna 2000;17:347-350
13. Stratton RJ, Hackston A, Longmore D et al. Malnutrition in hospital outpatients and inpatients: prevalence, concurrent validity and ease of use of the ‘malnutrition universal screening tool’ (‘MUST’) for adults. Br J Nutr 2004;92:799-808
14. Vischer UM, Perrenoud L, Genet C et al. The high prevalence of malnutrition in elderly diabetic patients: implications for anti-diabetic drug treatments. Diabet Med 2010;27:918-924