E. Ardolino1, A. Garrett Ramos3, H. Hutchins-Wiese1,2, J. Kerstetter3, J. Bihuniak3, A. Kleppinger1, A.M. Kenny1
1. Center on Aging, UConn Health, Farmington, CT, USA; 2. Dietetics and Human Nutrition, Eastern Michigan University, Ypsilanti, MI, USA; 3. Department of Allied Health Sciences, University of Connecticut, Storrs, CT, USA
Corresponding Author: Anne M. Kenny, MD, Center on Aging, MC-5215, UConn Health, Farmington, CT 06030-5215, Email: kenny@uchc.edu, Phone: (860) 679-4928
J Aging Res Clin Practice 2017;6:94-100
Published online May 4, 2017, http://dx.doi.org/10.14283/jarcp.2017.9
Abstract
Objectives: To evaluate whether Mediterranean style diet (MedSD) is associated with better physical performance. There is evidence from large epidemiological studies that MedSD associates with lower risk of chronic disease and mortality. Poor functional capacity, partially affected by poor physical performance, also predicts higher morbidity and mortality resulting in higher healthcare costs. Design: One group, longitudinal pilot clinical intervention trial of 24 weeks total; 12 weeks observation followed by 12 weeks intervention in 16 postmenopausal women (age>65 y) evaluating effects on physical performance. Setting: Outpatient clinical research center. Participants: 16 postmenopausal women (age>65 y) selected for typical American diet. Intervention: Women consumed their typical diet for 12 weeks followed by a 12-week MedSD intervention. A registered dietitian counseled the subjects to make 4 dietary changes: 1) incorporate 3 tablespoons Extra Virgin Olive Oil (EVOO) daily; 2) include 3-5 servings/week of high omega-3 fish (salmon or tuna); 3) incorporate 1.5 ounces of walnuts daily; 4) incorporate increased amounts of fruits, vegetables and whole grains. Measurement: Food frequency questionnaire scores, 3-day diet record, serum total fatty acids, anthropometry, physical activity, functional capacity (chair rise time, single leg time, hand grip strength were measured. Pre-post analysis compared the 2 weeks typical diet period with the 2 weeks MedSD intervention period. Correlations were used to relate dietary change to physical performance change. Results: Diet analysis revealed adherence to the MedSD (p = < 0.001). No significant differences were observed in hand grip strength or the Short Physical Performance Battery. Significant correlations were found between change in chair rise time and changes in intake of carbohydrates (r= 0.587) and trans and saturated fat (r= 0.818). Inability to identify other significant correlations in primary outcomes was likely affected by small sample size and physically robust participant group. Conclusions: Alterations in consumption patterns to adhere to a MedSD, including reductions in saturated fat and carbohydrate consumption, correlate with improvement in chair rise time. This study design can be used for future studies with a larger group of frailer, older adults to assess the effect of MedSD on physical performance.
Key words: Mediterranean style diet; physical performance; postmenopausal women; omega-3 fatty acids.
Background
The Mediterranean diet (MedSD) is based on the following basic principles: high fruit and vegetable intake, moderate intake of fish, dairy, legumes, grain, monounsaturated fatty acids (mostly olive oil), alcohol, and low saturated fat intake. The health benefits of adherence to a MedSD have been thoroughly investigated and include: reduced mortality, reduced cardiovascular event incidence and mortality, reduced cancer incidence or mortality, and reduced incidence of neurodegenerative disease (1-3 4). High levels of fruits, vegetables, fish, and olive oil in a typical MedSD and the nutrients that these foods contain such as flavonoids, phenols, polyunsaturated fatty acids (PUFA), and monounsaturated fatty acids (MUFA) are linked to improved health (5, 6). Thus far, there is little research specifically assessing the effect of a MedSD on functional capacity in older adults. We are interested in investigating this question, especially considering the significance of poor functional capacity in the geriatric population and its correlation with mortality and poor quality of life.
There are many proposed health benefits of adhering to a MedSD that could improve functional capacity in the geriatric population including improved inflammatory state, improved nutrition status, and decreased obesity (7-15). Various studies illustrate the nutritional benefits of the MedSD and how it potentially could lead to improvement in physical performance and the frailty phenotype. Roche et al. suggest that the increase in use of olive oil in the MedSD improves inflammatory state by lowering of the toxic oxidative products of fatty acid oxidation by olive phenols (7, 16). Further, high levels of omega (n)-3 long chain PUFA from fatty fish decrease inflammatory markers TNF-alpha and IL-6 and increase anti-inflammatory markers IL-6r, Il-10, and TGF-beta (8). One study found that high levels of serum n-3 PUFA from consuming fish are inversely correlated with decline in physical performance (9). Similarly, substituting MUFA such as those found in olive oil for saturated fats (SFA) is associated with improved physical activity (10). Epidemiological evidence suggests that micronutrient deficiencies of beta-carotene, Vitamin D, folate, Vitamin E, and Selenium, are independently associated with an increased frailty phenotype and decreases in physical performance (11-14). A large meta-analysis demonstrated that following a MedSD has also been associated with weight loss (17). Clinical trials have also shown that central obesity is associated with poor locomotion, increased back pain and knee pain (15).
The purpose of the study was to assess the effects of adherence to a MedSD (rich in fish, olive oil, walnuts, legumes, fruit and vegetables) on characteristics of frailty and physical performance including weight loss, hand grip strength, endurance, reported physical activity, and walking speed.
Methods
Participants
Thirty-three postmenopausal women were contacted from a list of volunteers from previous studies conducted in the University of Connecticut Center on Aging screened via telephone for participation. Ten women failed telephone screening leaving 23 postmenopausal women who voluntarily enrolled. Seven of these subjects were dropped during the study period secondary to changes in supplement use (meeting exclusion criteria), resulting in a total of 16 participants completing the study. The trial design was a one group, single crossover longitudinal pilot clinical intervention. Each subject followed a baseline control diet for 12 weeks and then switched to a MedSD. Subjects visited the research site every 3 weeks for a total of 9 visits.
Exclusion criteria included women less than 65 years, any disease that may affect bone metabolism, cancers of any kind (except basal or squamous cell of the skin) in the past 5 years, use of medication known to affect bone metabolism, participating in physical activity more than 75 minutes/day for 6 days/week, dietary behaviors or supplementation in excess of DRI upper limits, vitamin D supplementation in excess of 10,000 IU/day, total calcium consumption from food and supplements exceeding 2,000 mg/day, following a medically prescribed diet or dietary pattern similar to the MedSD, history of chronic renal or liver disease, history of hip fracture or known vertebral fracture within the past year, alcoholic beverage intake >3 drinks/day, having an allergy to fish or nuts. In addition, if potential participants consumed more than four servings/day of fruit and vegetable, 2 or more servings/week of fatty fish, or consumption of 3 or more servings/week of any seafood (achieving a score (45/55 on the Mediterranean-Style Dietary Pattern Score (MSDPS) were excluded. The study was approved by the Investigational Review Board at the University of Connecticut Health Center (UCHC). All participants gave their written informed consent.
Diets
Subjects followed their typical diets for the first 12 weeks of the study. They were instructed by a Registered Dietitian not to make any major changes to their typical diet (i.e. do not introduce new diet habits or eliminate foods or food groups) and not to change their nutritional supplements or physical activity. This period served as the control for the intervention phase.
After the 12 week control phase, women crossed over to the intervention phase at which time, participants were educated by a Registered Dietitian to begin the MedSD. MedSD intervention included four components: 1) incorporation of 3 tablespoons extra virgin olive oil (EVOO) daily; 2) incorporation of 3-5 servings/week of high n-3 fish (salmon or tuna); 3) incorporation of 1.5 ounces of walnuts daily; 4) general recommendations for the incorporation of increased amounts of fruits, vegetables and whole grains. Participants were provided with the first three components of the diet at the research site, and were instructed on how to make the changes involved in the fourth component on their own. Participants could choose any combination of frozen tuna steaks, frozen salmon fillets, or canned tuna in water to meet the requirements of the second dietary component. In order to maintain consistent calorie consumption and prevent weight gain, subjects were counseled about the importance of making the above dietary changes via replacement of already existing foods rather than addition of these foods (i.e. EVOO to replace butter, salmon to replace beef or pork, etc.). In addition, participants were counseled in the overall goals of the Mediterranean diet and given a copy of The Mediterranean Diet by Marissa Cloutier and Eve Adamson, 2004. The counseling sessions lasted approximately 60 minutes per encounter, included the use of food props and left ample time for questions and answers.
Data Collection
Participants traveled to the Center on Aging at the UCHC in Farmington, Connecticut for each study visit. Diet was recorded with a Harvard Mediterranean food frequency questionnaire (FFQ) (baseline, week 12, and 24) and reviewed with the subject by a Registered Dietitian for accuracy. An 11-question Mediterranean-Style Dietary Pattern Score (MSDPS (18) was calculated from the FFQ at visits baseline, week 12 and 24. MSDPS scores ranged from 0-55, with higher scores indicating greater adherence to a MedSD.
At baseline, weeks 6, 12, 18 and 24, blood was collected and serum separated and stored at -80°C until analysis. Fatty acids were extracted, methylated, and the resulting methyl esters (FAME: fatty acid methyl esters) were analyzed by gas chromatography. Individual fatty acids were identified from sample peak comparison to authentic FAME standards and reported as area percentage of total fatty acids.
Body Composition, Strength testing and Physical Performance testing
Total and regional lean tissue masses of volunteers were determined from a whole body dual x-ray absorptiometry (DXA) DPX-IQ scanner (GE Medical Systems Lunar, Madison, WI); all scans were obtained by the same certified technician. At baseline, whole body scan provided total lean body mass [LBM (kg)], total fat mass (kg) and total body bone mineral content (kg). Appendicular skeletal muscle mass (ASM) was determined by combining the lean tissue mass of the regions of the arms and legs, excluding all other regions from analysis (19).
Physical performance was assessed by the hand grip strength (Jamar hand-held dynamometer), and the Short Physical Performance Battery (SPPB) which includes ability to rise from a chair, static balance and the timed 8 foot walk (20) were assessed at baseline, 12 and 24 weeks.
Statistical Analysis
The primary outcomes in this study were physical performance measures after a change in diet. First, change in dietary factors and physical performance was calculated by subtracting the 12 week visit measures from baseline measures for change during the baseline period. Next, intervention change was calculated by subtracting the 24 week measures from 12 week measures for changes due to Mediterranean diet. Change in physical performance measures was compared using paired t-tests. As a secondary analysis, paired t-tests were performed to detect changes within each 12 week period. Correlations compared associations between dietary changes and physical performance changes. Descriptive, correlations, and mean change comparisons were assessed using SPSS statistical software (version 19 for Windows). All data were tested for normality using the Shapiro-Wilk test and a p-value of <0.05 indicated that the data differed significantly from a normal distribution. All change scores were normally distributed.
Results
The enrolled sample at baseline (visit 1) included 22 postmenopausal women, with a mean age of 77±6.8 years, mean weight of 65.4±8.7 kg, and mean BMI of 25.4±2.9 kg/m2. By the conclusion of the study, three subjects were dropped because they began taking fish oil supplements after enrollment, and three were dropped because it was discovered that they had initially underreported their typical intake of Mediterranean foods, leaving 16 subjects who completed the study.
Weight, BMI, lean mass and waist circumference did not change significantly throughout the study period from week 1 through week 24. Fat mass initially declined during the typical diet and then returned to baseline values following adoption of the Mediterranean diet (Table 1). Women had significant improvement in their Mediterranean Diet Score (MDS) during the period of Mediterranean diet compared to typical diet (p<0.001), but no significant differences in macronutrients were noted (Table 2). Several key serum fatty acids changes were seen including decreases in long chain n-6 fatty acids (22:4n6; 22:5n6) and increases in several long chain n-3 PUFA (20:5n3 and 22:6n3) (21).
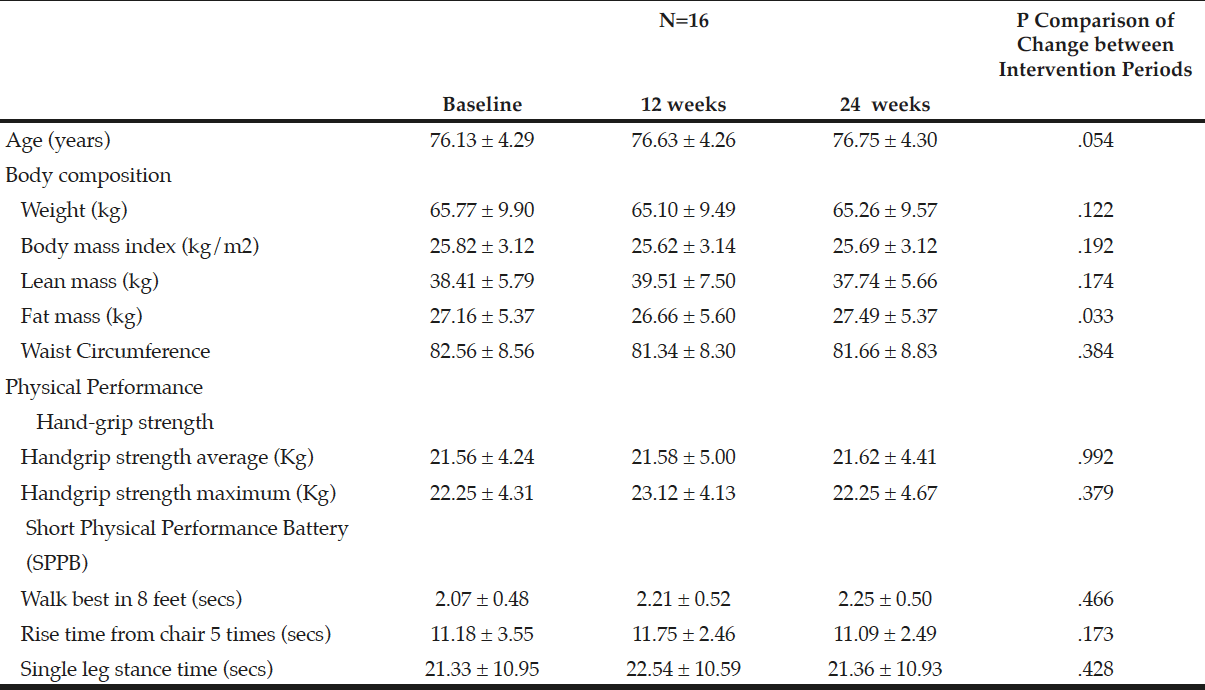
Table 1
Characteristics of participants at baseline, week 12 (end of observation period) and week 24 (end of Mediterranean Diet intervention)
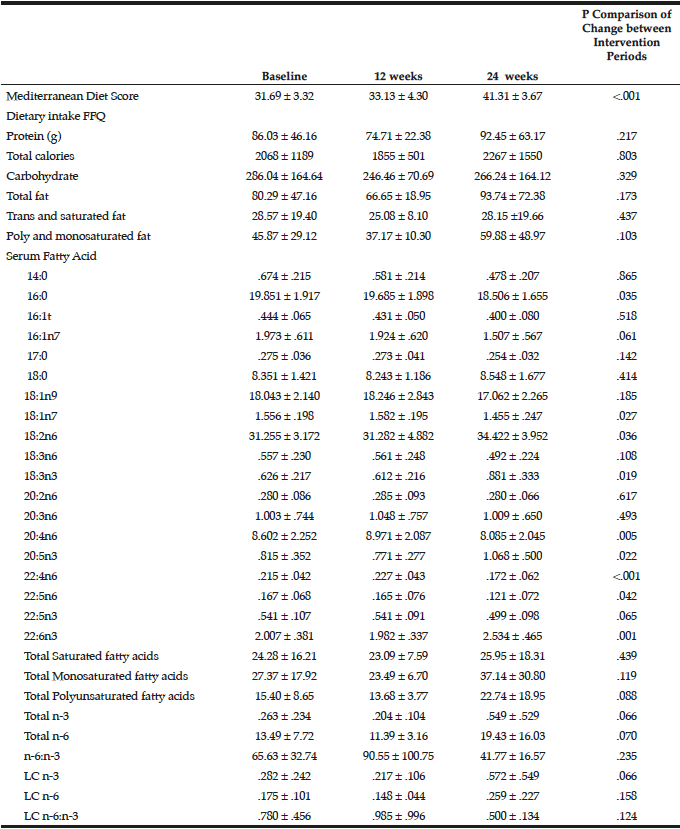
Table 2
Dietary and fatty acid characteristics of participants at baseline, week 12 (observation period) and week 24 (following Mediterranean diet intervention)
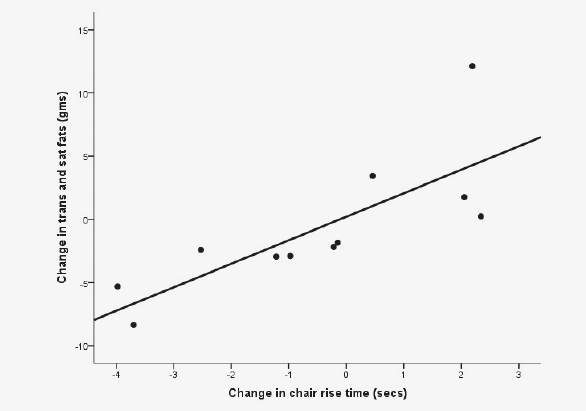
We compared changes in physical performance measures during typical (weeks 1 through 12) and Mediterranean diet (weeks 12 through 24) periods and did not find significant differences in hand grip strength or the Short Physical Performance Battery. We then looked for correlative changes in physical performance with changes in diet. Significant correlations were found in change in chair rise time and changes in carbohydrate intake (r = 0.587) and trans and saturated fat intake (r = 0.818) (Figure 1).
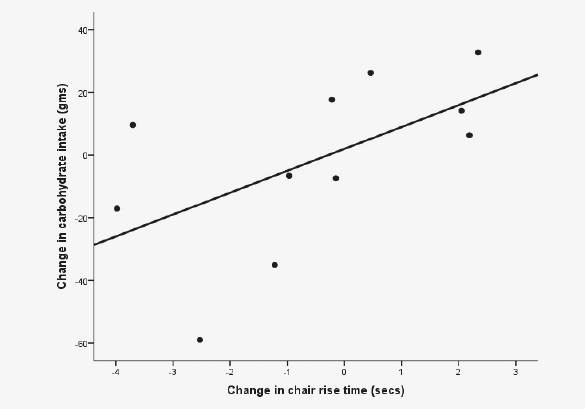
Figure 1
The association between change in chair rise time and change in trans-and saturated fats (a) and carbohydrates (b) with diet modifications consistent with a Mediterranean diet
Discussion
Adherence to a MedSD can benefit many aspects of health. By studying a small group of postmenopausal women during a period of their typical American-style diet low in fruits, vegetables and monosaturated fats and a period of the MedSD, we hoped to find evidence to suggested this diet can be beneficial to older adults by improving their physical function. While the results of this study did not reveal statistically significant changes in physical performance endpoints, small changes were detected in rise time which would suggest a trend toward improvement, especially if larger studies are performed in the future. Additionally, further investigation of the data demonstrated statistically significant correlation between chair rise and reduction of dietary carbohydrates and trans and saturated fats throughout the intervention period.
This study also accomplished an important goal as a pilot study, by demonstrating that this population is able to adhere to the Mediterranean style diet (p<0.001). Some of the dietary changes were facilitated by providing portions of fish, walnuts, and olive oil to the participants, but most of the changes were made by the participants, demonstrating willingness and ability to adhere to the diet. Proving effective adherence to a diet is important clinically (22) and the MedSD should be considered as a legitimate option.
A possible limitation of this study is the relatively high starting physical performance level of this patient population, which could partially explain the low effect size for physical performance measures. Theoretically, the changes that would be expected from a patient who already has a high SPPB or short chair rise time would be less than for a patient who is less physically fit with more potential for improvement. For instance, the group’s mean chair rise time prior to intervention was within normal range (11.8 seconds). Similarly, the average walking speed in this patient population prior to intervention was 1.178 m/s, which qualifies as normal gait speed in the SPPB (slow gait: <0.78 m/s). Both chair rise time and gait speed are moderate to good predictors of frailty in community dwelling older adults (23). In other studies of individuals selected for excellent function, interventions such as dehydroepiandrosterone were not effective (24, 25), but when given in a more frail population, improvement in function was seen (26). Therefore, the population selected for this study is most likely not an adequate representation of the frail phenotype. Selecting for frailer subjects in future studies should improve the ability to observe significant changes in physical performance measures.
Another similar limitation to our data is that the average participant followed a typical diet rich in protein and moderate in calories prior to the intervention, consuming an average of 801 IU of Vitamin D, 1.28 g/kg of protein, 0.99 grams of Omega n-3 PUFA, which are all above the recommended daily intake of these nutrients (27). Subjects were excluded if their typical diet were characteristic of a MedSD, but participants were selected from generally affluent areas and likely had significant pre-intervention exposure to education and resources that would portend healthier eating habits. Potential positive health benefits of the MedSD theoretically might have a lesser effect on subjects with a balanced, nutritious pre-intervention diet. A correlation between good general nutrition status and physical performance has been established. Studies have shown that patients who meet criteria for “well-nourished” with high the Mini Nutritional Assessment have significantly higher mobility index, ADL index, higher performance tests index, and higher hand grip scores (28). Similarly, any diet (MedSD or non-MedSD) rich in omega-3 fatty acids, vitamin D, protein, and antioxidants have been found to decrease the risk of sarcopenia in older adults (27, 29). In future studies of this type, it would be beneficial to study a set of participants with poorer overall nutritional status in order to better detect the effects of a MedSD.
In many of the key nutrition and anthropomorphic categories, patients improved during the typical diet period, prior to the MedSD intervention. On average in the pre-intervention period, participants lost 0.68 kg, lost 1.23 cm in waist circumference, decreased their BMI by 0.21, increased their lean mass by 1.1 kg, decreased their fat mass by 0.51 kg, and increased their Mediterranean diet score by 1.44 points. A likely explanation for these data is that participants became more aware of their typical diet and made diet changes outside the recommendations of the study. Therefore, a Hawthorne effect likely affected our ability to detect significant changes in endpoints throughout the intervention period (30).
The MedSD has been lauded for its numerous health benefits, and is therefore of great interest to the medical community. Our study suggests that certain aspects of the MedSD are correlated with improvement in physical performance in the elderly. Inability to find other significant changes in primary outcomes was likely affected by small sample size, physically robust participant group, and a Hawthorne effect. However, by demonstrating this correlation between MedSD and physical performance along and by proving effective participant adherence, we are confident that this proves the clinical utility of this diet and we believe that further clinical investigations with a larger group of frailer, older adults with a similar study design is warranted.
Conflict of Interest: Dr. Ardolino has nothing to disclose; Ms. Anna Garrett Ramos has nothing to disclose; Dr. Hutchins-Wiese has nothing to disclose; Dr. Kerstetter has nothing to disclose; Dr. Bihuniak has nothing to disclose; Ms. Kleppinger has nothing to disclose; Dr. Kenny has nothing to disclose. The authors state that there are no conflicts of interest to be declared.
Ethical standards: This study complies with current laws of ethical considerations in the United States of America.
Acknowledgment: This work was supported by the Diet and Heatlh Inititiative, University of Connecticut, Storrs CT. We wish to thank Lisa Godin for her assistance in manuscript preparation.
References
1. Estruch R, Ros E, Martinez-Gonzalez MA. Mediterranean diet for primary prevention of cardiovascular disease. The New England journal of medicine 2013;369:676-7.
2. Estruch R, Ros E, Salas-Salvado J, et al. Primary prevention of cardiovascular disease with a Mediterranean diet. The New England journal of medicine 2013;368:1279-90.
3. Ruiz-Canela M, Estruch R, Corella D, Salas-Salvado J, Martinez-Gonzalez MA. Association of Mediterranean diet with peripheral artery disease: the PREDIMED randomized trial. Jama 2014;311:415-7.
4. Sofi F, Abbate R, Gensini GF, Casini A. Accruing evidence on benefits of adherence to the Mediterranean diet on health: an updated systematic review and meta-analysis. The American journal of clinical nutrition 2010;92:1189-96.
5. Ortega R. Importance of functional foods in the Mediterranean diet. Public Health Nutr 2006;9:1136-40.
6. Tresserra-Rimbau A, Rimm EB, Medina-Remon A, et al. Polyphenol intake and mortality risk: a re-analysis of the PREDIMED trial. BMC medicine 2014;12:77.
7. Roche M, Dufour C, Loonis M, Reist M, Carrupt PA, Dangles O. Olive phenols efficiently inhibit the oxidation of serum albumin-bound linoleic acid and butyrylcholine esterase. Biochim Biophys Acta 2009;1790:240-8.
8. Ferrucci L, Cherubini A, Bandinelli S, et al. Relationship of plasma polyunsaturated fatty acids to circulating inflammatory markers. J Clin Endocrinol Metab 2006;91:439-46.
9. Abbatecola AM, Cherubini A, Guralnik JM, et al. Plasma polyunsaturated fatty acids and age-related physical performance decline. Rejuvenation Res 2009;12:25-32.
10. Kien CL, Bunn JY, Tompkins CL, et al. Substituting dietary monounsaturated fat for saturated fat is associated with increased daily physical activity and resting energy expenditure and with changes in mood. The American journal of clinical nutrition 2013;97:689-97.
11. Bartali B, Frongillo EA, Bandinelli S, et al. Low nutrient intake is an essential component of frailty in older persons. J Gerontol A Biol Sci Med Sci 2006;61:589-93.
12. Ble A, Cherubini A, Volpato S, et al. Lower plasma vitamin E levels are associated with the frailty syndrome: the InCHIANTI study. J Gerontol A Biol Sci Med Sci 2006;61:278-83.
13. Semba RD, Bartali B, Zhou J, Blaum C, Ko CW, Fried LP. Low serum micronutrient concentrations predict frailty among older women living in the community. J Gerontol A Biol Sci Med Sci 2006;61:594-9.
14. Alipanah N, Varadhan R, Sun K, Ferrucci L, Fried LP, Semba RD. Low serum carotenoids are associated with a decline in walking speed in older women. The journal of nutrition, health & aging 2009;13:170-5.
15. Muramoto A, Imagama S, Ito Z, et al. Waist circumference is associated with locomotive syndrome in elderly females. Journal of orthopaedic science : official journal of the Japanese Orthopaedic Association 2014;19:612-9.
16. Guasch-Ferre M, Hu FB, Martinez-Gonzalez MA, et al. Olive oil intake and risk of cardiovascular disease and mortality in the PREDIMED Study. BMC medicine 2014;12:78.
17. Huo R, Du T, Xu Y, et al. Effects of Mediterranean-style diet on glycemic control, weight loss and cardiovascular risk factors among type 2 diabetes individuals: a meta-analysis. European journal of clinical nutrition 2014.
18. Rumawas ME, Dwyer JT, McKeown NM, Meigs JB, Rogers G, Jacques PF. The development of the Mediterranean-style dietary pattern score and its application to the American diet in the Framingham Offspring Cohort. The Journal of nutrition 2009;139:1150-6.
19. Wang ZM, Visser M, Ma R, et al. Skeletal muscle mass: evaluation of neutron activation and dual-energy X-ray absorptiometry methods. J Appl Physiol (1985) 1996;80:824-31.
20. Guralnik JM, Simonsick EM, Ferrucci L, et al. A short physical performance battery assessing lower extremity function: association with self-reported disability and prediction of mortality and nursing home admission. J Gerontol 1994;49:M85-94.
21. Ramos A, Bihuniak J, Huedo-Medina T, et al. Adherence to a Mediterranean-style Diet and its Impact on Cardiovascular Risk Factors in Postmenopausal Women. 2015.
22. Zazpe I, Estruch R, Toledo E, et al. Predictors of adherence to a Mediterranean-type diet in the PREDIMED trial. European journal of nutrition 2010;49:91-9.
23. Schoon Y, Bongers K, Van Kempen J, Melis R, Olde Rikkert M. Gait speed as a test for monitoring frailty in community-dwelling older people has the highest diagnostic value compared to step length and chair rise time. Eur J Phys Rehabil Med 2014;50:693-701.
24. Muller M, van den Beld AW, van der Schouw YT, Grobbee DE, Lamberts SW. Effects of dehydroepiandrosterone and atamestane supplementation on frailty in elderly men. J Clin Endocrinol Metab 2006;91:3988-91.
25. Dayal M, Sammel MD, Zhao J, Hummel AC, Vandenbourne K, Barnhart KT. Supplementation with DHEA: effect on muscle size, strength, quality of life, and lipids. J Womens Health (Larchmt) 2005;14:391-400.
26. Kenny AM, Boxer RS, Kleppinger A, Brindisi J, Feinn R, Burleson JA. Dehydroepiandrosterone combined with exercise improves muscle strength and physical function in frail older women. J Am Geriatr Soc 2010;58:1707-14.
27. Mithal A, Bonjour JP, Boonen S, et al. Impact of nutrition on muscle mass, strength, and performance in older adults. Osteoporos Int 2013;24:1555-66.
28. Ferdous T, Cederholm T, Razzaque A, Wahlin A, Nahar Kabir Z. Nutritional status and self-reported and performance-based evaluation of physical function of elderly persons in rural Bangladesh. Scand J Public Health 2009;37:518-24.
29. Volkert D. The role of nutrition in the prevention of sarcopenia. Wien Med Wochenschr 2011;161:409-15.
30. McCarney R, Warner J, Iliffe S, van Haselen R, Griffin M, Fisher P. The Hawthorne Effect: a randomised, controlled trial. BMC Med Res Methodol 2007;7:30.