Y. Hokotachi1,2, S. Ichimaru2, M. Hayashida2,3, T. Amagai2
1. Department of Clinical Nutrition, Takarazuka Dai-ichi Hospital; 2. Administration Food Sciences and Nutrition Major, Graduate School of Human Environmental Sciences, Mukogawa Women’s University, Japan; 3. Departmentof Clinical Nutrition, Kobe Adventist Hospital, Japan.
Corresponding Author: T. Amagai, Administration Food Sciences and Nutrition Major, Graduate School of Human Environmental Sciences, Mukogawa Women’s University, Japan, amagaipedteruyoshi@gmail.com
Abstract
Aim: To examine the hypothesis that larger cumulative energy deficit and late initiation of enteral nutrition for older adult patients in non-acute setting is associated with poor outcome at 3 and 6 months later. Methods: This is retrospective study with chart review in a single institute. The consecutive older adult patients (>= 65 years-old) admitted to the institute were included. Dividing all subjects by two categories: take nutrients by mouth (PO) during hospital stay vs. non-PO group, and enteral nutrition (EN) during the first 7 and 14 days after admission vs. non-EN (NEN) group. Between these two groups, demographics, nutritional, and outcomes were compared. Results: 1, PO group showed significantly longer length of hospital stay (p=0.049). 2, NEN group showed significantly larger cumulative energy deficit, longer length of hospital stay, and higher mortality at 3 and 6 months later (p=0.000, p=0.000, p=0.044, and p=0.008, respectively). Conclusion: The larger cumulative energy more than 10, 000 kcal is considered to be associated with poor clinical outcomes, including longer LOS and higher mortality at 3 and 6 months later in the hospitalized older adults (>= 80 years-old). The cumulative energy deficit might be considered in nutritional support even for older adults admitted to non-acute setting to prevent poor outcomes.
Key words: Cumulative energy deficit, enteral nutrition, older adult, non-acute, outcome.
Introduction
Clinical outcomes are predicted by multiple factors, including vital signs and immune function (1, 2) in patients in acute settings and sarcopenia status in community-dwelling older adults (3). These predictors might also help identify impairment in anti-bacterial capacity and mobility in older adults. However, the question of whether nutritional delivery for the first few days after hospital admission is a predictor of later outcomes in older patients remains unclear.
Here, we examined our working hypothesis that an early energy deficit in older adults admitted in non-acute settings impacts later outcomes, such as 3- or 6-month mortality after admission.
Methods
The study was conducted under a retrospective design with chart review at a single institution. All consecutive patients aged 65 years and older on admission to a single institution between November 2010 and October 2011 were eligible. Exclusion criteria were: (1) length of hospital stay (LOS) < 2 days, (2) duration of enteral nutrition (EN) ≥ 300 days, (3) daily amount of EN < 200 ml, and (4) EN starting earlier than 2 days after admission. These exclusion criteria were identified as inappropriate in examining the impact of enteral nutrition on clinical outcomes. Landmark days used in the study were defined as follows: D1 was the admission day, D2 was the day to initiate EN, and D3 was the day of discharge from hospital. Further, to compare the two groups by PO or EN status, D4 was defined as the first 7 or 14 days after admission, unless EN was initiated before D4, as described in methods 1 and 2, respectively (Fig.1).
Data collection
Data covering the total hospitalization period were collected from the clinical charts of subjects and divided into three domains, as follows:
(1) demographic data included age, sex, height, weight, primary diagnosis, and Charlson comorbidity index (CCI) score to evaluate the severity of the primary diagnosis. All were measured on admission cymbaltaonline-pharmacy day (D1).
(2) nutritional parameters included route of EN administration of enteral nutrition formulae by mouth or through a nasogastric (NG) or gastric (G) tube; energy density of EN formulae at D2 (kcal/ml); number of subjects who achieved an energy target; length of intestinal starvation defined as nil by mouth until D2 (days); and cumulative energy deficit between D1 and D3 calculated by the difference in energy amount between the energy target, set at 25 kcal/kg of actual body weight/day as proposed by the ESPEN guideline (7) and total energy amount delivered through all routes, including parenteral, enteral and oral routes. Cumulative protein deficit was calculated the same way, with a protein target set at 1.0 g/kg/day. Cumulative energy deficits delivered through both parenteral and enteral route was calculated every 7 days until the day of initiation of EN (D3), maximally until the first 28 days after admission, and are expressed in daily units, as the same was also conducted in cumulative protein deficit administered through parenteral route.
(3) outcome parameters have primary and secondary outcomes: primary outcomes included mortality rate (%) during hospitalization period (between D1 and D3) and death rate at 28 days, 3 months, and 6 months after admission, and secondary outcomes including the length of hospitalization (days, between D1 and D3, LOS), ; and discharge status by type of institution after discharge in the three categories of home, nursing home and rehabilitation hospital, occurrence of adverse events, including diarrhea, and constipation, vomiting, and comorbidities of pneumonia and pressure ulcer during periods of EN management between D2 and D4 (Table 2, 3), and utilization of antibiotics for treatment purpose (%), and CRP > 6.0 mg/dl during hospitalization, before D2, and after D2. Adverse events were defined as diarrhea, watery or loose stools three or more times per day; and constipation, no defecation for at least four consecutive days. Cause of death was analyzed for patients who died during hospitalization in the study period. Survival status was defined by survival during hospitalization at 3 or 6 months after admission
Comparisons of groups by two classifications, PO vs. NPO and EN vs. NEN
To examine our hypothesis that a cumulative nutritional deficit impacted outcomes, all subjects were divided into two groups in each of two categories, as follows: (1) the PO and non-PO (NPO) groups were classified by their ability or inability to start total energy and macronutrient intake by mouth during hospitalization, as detailed in method 1; and (2) the EN and non-EN (NEN) groups were classified by their ability or inability to initiate EN within the first 7 (D7) or 14 days (D14) after admission, as detailed in method 2.
All collected data of the three domains described above were then compared among groups in the two classifications (PO vs. NPO, and EN vs. NEN; Fig. 1).

Figure 1 Flow chart of the study with methods 1, 2, and 3: for each method, data shown in the bottom square were compared at the individual timings shown in the right columns
D1:admission day, D2:day to initiate enteral nutrition (EN), D3:day todischarge from hospital, D4:the first 7 or 14 day after admission, unlessEN was initiated before D4, D7:7th day after admission, D14:14th day after admission.
Method 1
Subjects were divided into two groups according to their ability to start energy and nutrient intake by mouth (Fig.1). PO group subjects were able to start oral intake between D1 and D3. NOP group subjects were not able to start oral intake on any hospitalization day.
Method 2
Subjects were divided into two groups according to their ability to initiate EN after D1 and after D3 (Fig. 1). EN group subjects were able to start EN between D1 and D3, while non-EN group subjects were not. All collected data for D7 and D14 were then compared among these two groups (Fig.1). Additionally, causes of death during hospitalization were compared between the two groups and odds ratios (ORs) were calculated and expressed as OR, 95% confidence interval (95% CI), and p value.
Statistical analysis
Groups in each category were compared using the Mann-Whitney U test for continuous variables and the chi-square or Fisher’s exact test for categorical variables. Multiple logistic regression analysis were conducted using death at discharge as the dependent variable, with oral nutrition, day of initiation of EN within 7 or 14 days after admission, diarrhea, constipation, vomiting, and pneumonia as the independent variables. The purpose of multivariable analyses was to reveal the impact of day of initiation of EN within 7 or 14 days after admission on outcome. All analyses were done using SPSS Statistics version 22 (IBM, Armonk, NY), with significance considered at the p < 0.05 level.
Results
Sixty-six of 82 patients were enrolled in this study as subjects for analysis. Sixteen subjects were excluded due to length of hospital stay < 2 days (n=8), period of EN ≥ 300 days (n=2), EN amount < 200 ml/day (n=1), starting EN within 2 days after admission (n=4), and admission for gastrostomy (n=1) (Fig. 1).
Result 1 – Comparison PO and NPO groups
Subjects were classified by their ability to take nutrients by mouth. Contrary to expectations, we found that the PO and NPO groups did not statistically differ by demographics, except with regard to the primary diagnosis of pneumonia (Table 1). In contrast, the later the day of initiation of the first EN (days), the larger the cumulative energy deficit (p=0.000, p=0.005, respectively, Table 2). Moreover, LOS was significantly longer in the PO group than the NPO group (p=0.049, Table 2). These results may suggest that the delayed initiation of EN in the PO buy accutane online group and significantly longer LOS were due to the expectation that the patient would be started with EN with PO. In contrast, initiation was relatively earlier and more easily in the NPO group.
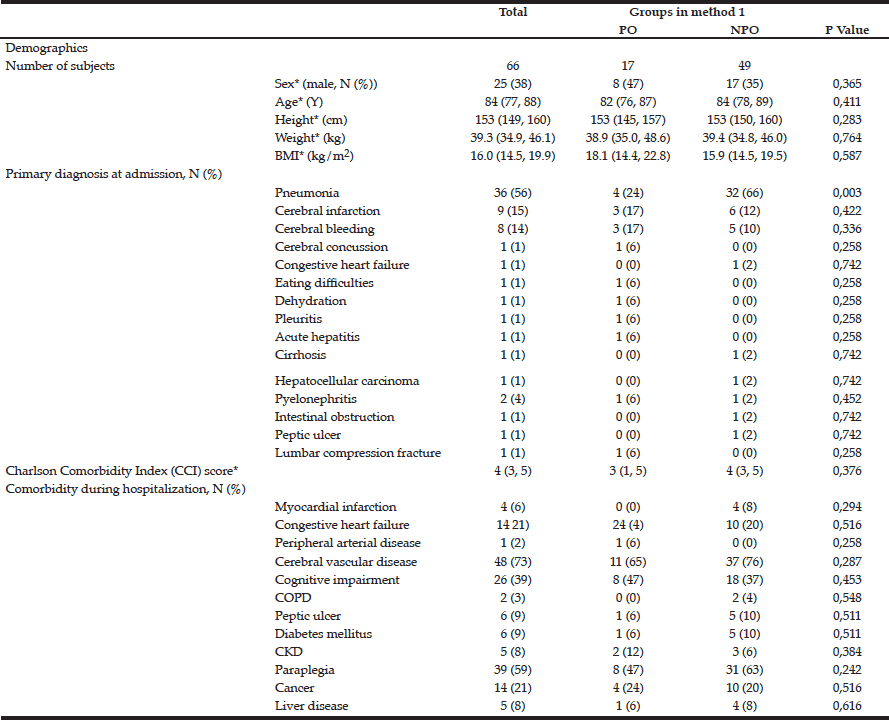
Table 1 Comparison of demographics, primary diagnosis, and Charlson Comorbidity Index (CCI) between the PO and NPO groups. No significant differences were seen between the two groups for any variable except the primary diagnosis of pneumonia, * values are median (25, 75 quartiles)
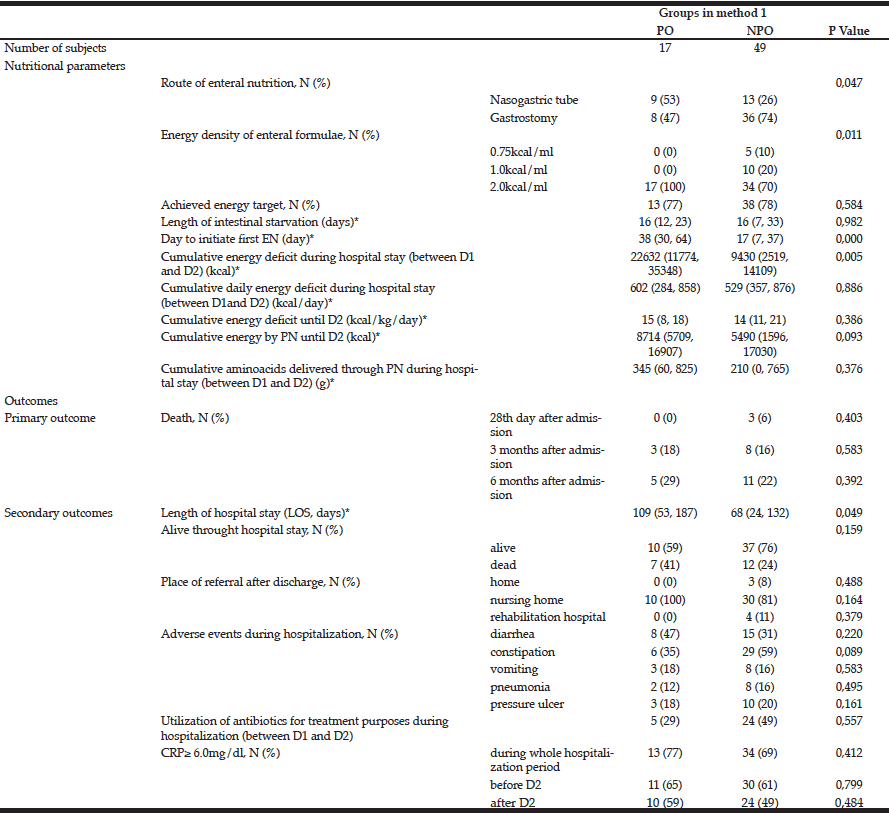
Table 2 Comparison of nutritional parameters and outcomes between the PO and NPO groups. No. of days to the initiation of EN in the PO group was significantly later and cumulative energy deficit during hospitalization (between D1 and D2) was significantly larger in the PO than in the NPO group (p=0.000, 0.005, respectively). Length of hospital stay (LOS) was significantly longer in the PO group (p=0.049), *values are median (25, 75% quartiles)
*D1: admission day, D2: day to initiate enteral nutrition (EN)
Indications for the use of gastrostomy as an enteral route are controversial. Early http://abilifygeneric-online.com/ EN using a gastrostomy (G-)tube may shorten LOS, as shown in the present study. However, the physical and economical burden of this approach and it labor burden on care-givers must be considered. A previous study (4) found no difference in mortality in older adult patients with gastrostomy regardless of the coexistence of cognitive impairment, but did identify several predictors, including subtotal gastrectomy, lower serum albumin
< 2.8 g/dl, age > 80 years, chronic heart failure, and male gender (ORs = 2.617, 2.081, 1.721, and 1.541, respectively).
Although more than one-third of subjects in both our PO and NPO groups had cognitive impairment (Table 1), the NPO group did not show a survival benefit despite the higher incidence of gastrostomy as a comorbidity. A conclusive answer to the survival benefit of a G-tube awaits additional study.
Result 2 – Comparison EN and NEN groups
The EN and NEN groups did not statistically differ by demographics (data, not shown). In contrast, CCI scores were significantly greater in the EN group, which had a greater severity of co-morbidities on admission, than in the NEN group (Fig. 1). This means that the severity of comorbidities was lower in the NEN group. However, nutritional parameters were all significantly lower in the EN than NEN group, including oral nutritional intake with EN (%) on the day of initiation of EN (D2), length of intestinal starvation until D2 (days), cumulative deficit in energy intake by EN (kcal) and PN (kcal), and cumulative deficits in aminoacids delivered through PN (g) until D2 (p=0.000 for all) (Table 3). Similarly, when subjects were divided into EN and NEN groups on the first 7 days after admission, LOS was significantly shorter and survival rates at 3 and 6 months after admission were significantly higher in the EN than NEN group (p=0.000 p=0.0044, and p=0.008, respectively) (Table 3). Similarly to these observations, significantly fewer patients with CRP ≥ 6.0 mg/dl were seen in the EN than NEN group during the whole hospital stay, and before and after EN initiation (p = 0.000 for all) (Table 4). Moreover, the concurrence rate of diarrhea and vomiting as adverse events during hospitalization was significantly lower in the EN group (p=0.009, and p=0.044, respectively) (data, not shown). Considering these findings, we conclude that the early initiation of EN and lower cumulative energy deficit is associated with a shorter LOS and higher survival rates at 3 and 6 months after admission, and a lower concurrence rate of comorbidity for diarrhea and vomiting, although causes zoloft dosage of deaths did not differ between the two groups on the 14th day after admission (D14). Death by D7 could not be examined because no subjects died during the first 7 days (D7) (data, not shown). Consistent with this, OR for initiation of EN (D2) within the first 14 days showed significantly lower death rate (p=0.008) (Table 4).
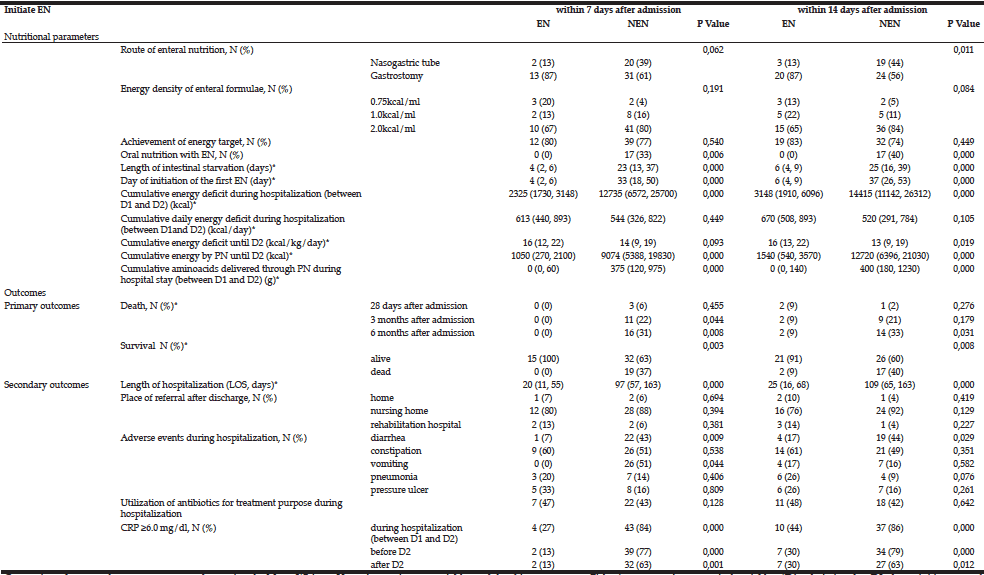
Table 3 Comparison of nutritional parameters and outcomes between the EN and NEN groups on the 7th and 14th days after admission. On analysis of the EN and NEN groups as early as at the 7th day after admission, cumulative energy deficit until D2 and D3 was significantly lower in the EN than the NEN group. Similarly, the clinical outcome, namely length of hospital stay, was significantly shorter (p=0.000), survival rate during hospitalization was significantly higher (p=0.003), and rates of adverse events during hospitalization were lower in the EN group, particularly diarrhea and vomiting (p=0.009, 0.044, respectively), CRP levels during hospitalization (CRP ≥6.0mg/dl) and after D2 were lower (P=0.000, 0.000, 0.001, respectively), and death at 3 and 6 months after admission, *values are edian (25, 75% quartiles)
Comparisons between the two groups were done using the Mann-Whitney U test for continuous variables and the chi-square test or Fisher’s exact test for categorical variables; *D1: admission day, D2: day to initiate enteral nutrition (EN), D3: day to discharge from hospital; *Values are median (25, 75% quartiles).

Table 4 Multiple logistic regression analysis of associations between death at discharge and variants on the 7th or 14th day after admission. Odds ratio (OR) of death was 0.073 in the subjects with early EN initiation within 14 days after admission (p=0.008)
Discussion
A study (4) in older adults admitted to the ICU with a BMI less than 20 kg/m2 reported better outcomes and a significantly lower need for respiratory assistance with lower energy administration during the first 7 days of admission, suggesting that BMI is an independent determinant of clinical outcome in these patients. In our present study, however, although mean BMI was similar to that in this previous report, our clinical setting was non-acute, versus acute in the previous study. Our hypothesis was that other factors might be associated with better outcomes in place of BMI, including energy deficit and route of nutritional delivery. The average age of all subjects admitted to the present single hospital was greater than 80 years (Table 1), suggesting that these subjects might mirror the super-aging society, in which the percentage of adults older than 65 years exceeds 21% of whole population. This demographic change is preceding similarly in most developed countries.
We focused on the route of nutritional delivery, and divided patients into two categories, a PO category for patients able to use oral intake and an EN category for when the enteral route could be used regardless of PO or NPO, on the basis that PO and EN should be considered different means of nutritional support, particularly for older adult patients.
Analysis of PO and NPO groups in Method 1
Subjects were classified by their ability to take nutrients by mouth. Contrary to expectations, we found that LOS was significantly longer in the PO than in the NPO group (p=0.049) and that cumulative energy deficit during the whole length of hospitalization was significantly greater in the PO group (p=0.005) (Table 2). These findings might mean that the PO group tended to have a larger cumulative energy deficient, despite the fact that the groups did not differ with regard to primary diagnosis on admission, severity of comorbidity as evaluated by CCI, or death rate as the primary outcome. Comparison clomid for men of primary diagnoses showed that significantly more subjects in the PO group had a primary diagnosis of pneumonia (p=0.003, Table 1). Further, these results might also suggest that older adults hospitalized with a primary diagnosis of pneumonia should be considered for early enteral nutrition through the gastrostomy route to shorten the length of stay in hospital (p=0.047) (Table 2).
Indications for gastrostomy for early enteral nutrition are controversial. Early gastrostomy may shorten LOS, as seen in the present study, but the physical burden for older adults and economic burden on medical society must also be considered. In a previous study, no difference in mortality was seen in older adult PEG patients with and without dementia (5). Predictors of poor survival were subtotal gastrectomy, lower serum albumin < 2.8 g/dl, age > 80 years, chronic heart failure, and male sex (ORs = 2.617, 2.081, 1.721, and 1.541, respectively) (5).
In the present study, although more than one-third of subjects in both the PO and NPO groups had cognitive impairment as comorbidity (Table 1), the NPO groups with a higher percentage of gastrostomy showed no survival benefit, as seen in the previous report (5). The clinical importance of gastrostomy in older adults with pneumonia and/or dementia warrants additional detailed study.
Analysis of the EN and NEN groups in Method 2
The first strength of this study is the observation of a cumulative energy deficit in the non-acute setting in older adult patients. To our knowledge, this is the first study to prove the influence of a short-term energy deficit on clinical outcomes in the non-acute setting in older adult patients. We set an energy target for the management of older adults admitted to a general ward of 25 kcal/kg actual body weight/day (7, 8), in accordance with the ESPEN guideline. A cumulative energy deficit was associated with outcomes at 3 and 6 months after admission in the older adult patients. The concept of energy deficit is frequently used in the acute setting (9, 10). Our results suggest that a cumulative energy deficit is associated with outcome in later periods even in non-acute settings. A conclusive result requires further investigations.
A second consideration is the extent to which a cumulative energy deficit is suitable during the early part of a short period of hospitalization. Our results may suggest that a cumulative energy deficit in the first 4 days after admission of 13000 kcal (mean, 12,735 kcal, 25, 75% quartiles: 6572, 25700 kcal: Table 3) seems to be a threshold in older adult patients in non-acute settings, and will act as an indicator of poor outcome (Table 4). In contrast, previous studies (6, 11) were conducted in acute settings, where an energy deficit of > 4,000 to 8,000 kcal or >100 kcal/kg of body weight lead to a higher frequency of infectious complications (9, 10, 12-15). The energy deficit shown in a non-acute setting seems larger than that in acute settings. One reason for this difference might be the difference in the number of days of observation for cumulative energy deficit. A second reason might be the late initiation of EN in the NEN group compared to the EN group (33 vs. 4 days to initiation of EN, respectively, p= 0.000) (Table 3). Even the less severely ill patients might have had a similar endocrine milieu, so immune modulation modulated by the timing and route of nutrition might have affected the outcome. This might be partly because older adults are likely more vulnerable to an energy deficit than younger adults, or because they tend to have multiple comorbidities. Although CCI score, used to evaluate the severity of comorbidities with EN, was worse in the EN than in the NEN group, the cumulative energy deficit in the EN group was less than that in the NEN group, and survival rate as a later outcome was significantly better (Table 3). The question of whether the relation between cumulative energy deficit and length of hospital stay is causal or an association awaits confirmation. Nevertheless, maintenance of a cumulative energy deficit with a threshold of 13000 kcal during the first 23 days after admission on average will prevent poor outcomes such as longer hospital stay and high mortality (Table 3).
Furthermore, optimum timing for the initiation of EN remains of concern. Unlike previous papers that argued for around 48 hours after admission to the ICU (6, 11), we focused on evaluation within 7 and 14 days after admission. This difference in time scale was because of the difference in subjects and ward characteristics, namely the acute setting in the 48-hour study versus the non-acute general ward setting in our study. In other words, instead of 48 hours for the ICU setting, we considered that the first 7 days after admission to a general ward was the proper time scale in which to examine timing for the initiation of enteral nutrition.
To our knowledge, this is the first study to report that the early initiation of EN in older adults admitted to non-acute wards impacted outcomes, namely that it was associated with a shorter LOS and a higher survival rate at 3 and 6 months later. The reason why early nutrition impacts outcomes long after admission warrants consideration. Although our study should be considered preliminary, it appears likely that the severity of the primary diagnosis is greatest in the first several days after admission, and that a cumulative energy deficit during this important period may impact the later outcome partly through immune deficiencies, as previously discussed (11). The causality or otherwise of an early energy deficit and later poor outcome in older patients in non-acute settings warrants further evaluation.
Of note, ORs for death were lower in patients with early EN initiation within the first 14 days after admission (Table 4). This finding suggests that an early start to EN within 14 days after admission will save lives among older adult patients admitted in non-acute settings. This better survival in older adult patients with the earlier initiation of EN may be due to the modulation of immune function (11). It might also be seen in non-acute settings in older adults in the area of clinical nutrition.
Several limitations of our study warrant mention. First, the study was conducted under a retrospective chart review. As frequently encountered in previous reports, many subjects did not meet the inclusion criteria. A prospective study design might prevent the loss of these patients. Second, the number of subjects was too small to allow any definitive conclusions, and additional larger studies are necessary. Third, the energy target of 25 kcal/kg/day requires validation, although indirect calorimetric evaluation as the gold standard measurement for resting energy expenditure is not available everywhere (9). Note that an energy target of 30 kcal/kg of actual body weight/day is recommended for patients managed in acute settings (14); clinical status in the non-acute settings in the present report undoubtedly differed from those in acute settings, and the target energy must be validated well.
While many studies have reported that early enteral nutrition is clinically beneficial, almost all subjects in these studies were under treatment in ICU settings (3, 5, 6). In contrast, our present subjects were less ill and were not hospitalized in the ICU. The CCI score for comorbidities showed that although our EN group had better survival at 3 and 6 months after admission, subjects had a more severe CCI score (p=0.044 and p=0.008, respectively) (data, not shown). In general, patients who are less critically ill are able to tolerate enteral nutrition, which modulates the immune response and provides a better outcome (6, 11). Indeed, even though the severity of comorbidity in the EN and NEN groups as evaluated by average CCI score (5 points representative of moderate severity (16) and 3 points representative of mild16, respectively; and moderate and mild severity (16), respectively) differed significantly, subjects in the EN group with a higher CCI score still tolerated enteral nutrition. This result might be interpreted to mean that the early initiation of EN is better indicator in older hospitalized adults admitted to non-acute wards than CCI score, regardless of the degree of comorbidity severity.
Conclusion
These findings in older adult patients suggest that a cumulative energy deficit over 13000kcal in the first 23 days of hospitalization in non-acute setting are associated with poor outcomes, including lower survival and longer length of hospital stay. This might be interpreted to mean that a cumulative energy deficit of less than 13000 kcal in 3 weeks after admission is associated with better clinical outcomes, including LOS and survival rate at 3 and 6 months, in hospitalized adults older than 80 years. Hospitalized older adult patients in non-acute settings should be followed for cumulative energy deficit.
Conflict of interest: The all authors have no conflict of interest to disclose.
Ethics Statement: This study was conductedaccording to the guidelines in the Declaration ofHelsinki, and all procedures were approved by theEthics Committee of Takarazuka Dai-ichi Hopital.
References
1. Koss CA, Jarlsberg LG, Den boon S, et al. A Clinical Predictor Score for 30-Day Mortality among HIV-Infected Adults Hospitalized with Pneumonia in Uganda. PLoS ONE. 2015;10:e0126591.
2. Hegazi RA, Dewitt T.
Enteral nutrition and immune modulation of acute pancreatitis. World J Gastroenterol. 2014;20:16101-5.
3. Kim JH, Lim S, Choi SH, et al. Sarcopenia: an independent predictor of mortality in community-dwelling older Korean men. J Gerontol A Biol Sci Med Sci. 2014;69:1244-52.
4. Ichimaru S, Fujiwara H, Amagai T, Atsumi T. ) Low energy intake during the first week in an emergency intensive care unit is associated with reduced duration of mechanical ventilation in critically ill, underweight patients: a single-center retrospective chart review. Nutr Clin Pract. 2014;29:368-79.
5. Kumagai R, Kubokura M, Sano A, et al. Clinical evaluation of percutaneous endoscopic gastrostomy tube feeding in Japanese patients with dementia. Psychiatry Clin Neurosci. 2012;66:418-22.
6. Heyland DK, Wischmeyer PE. Does artificial nutrition improve outcome of critical illness? An alternative viewpoint!. Crit Care. 2013;17:324.
7. Kreymann KG, Berger MM, Deutz NE, et al. ESPEN Guidelines on Enteral Nutrition: Intensive care. Clin Nutr. 22006;5:210-23.
8. Krishnan JA, Parce PB, Martinez A, Diette GB, Brower RG. Caloric intake in medical ICU patients: consistency of care with guidelines and relationship to clinical outcomes. Chest. 2003;124:297-305.
9. Faisy C, Candela llerena M, Savalle M, Mainardi JL, Fagon JY. Early ICU energy deficit is a risk factor for Staphylococcus aureus ventilator-associated pneumonia. Chest. 2011;140:1254-60.
10. Abdallah A. Gharraf H. Okasha H. Early ICU energy deficit: Is it a risk factor for ventilator-associated pneumonia? Egypt J Chest Dis Tuberc 2014;63:3-7.
11. Huang HH, Hsu CW, Kang SP, Liu MY, Chang SJ. Association between illness severity and timing of initial enteral feeding in critically ill patients: a retrospective observational study. Nutr J. 2012;11:30.
12. Faisy C, Lerolle N, Dachraoui F, et al. Impact of energy deficit calculated by a predictive method on outcome in medical patients requiring prolonged acute mechanical ventilation. Br J Nutr. 2009;101:1079-87.
13. Soguel L, Revelly JP, Schaller MD, Longchamp C, Berger MM. Energy deficit and length of hospital stay can be reduced by a two-step quality improvement of nutrition therapy: the intensive care unit dietitian can make the difference. Crit Care Med. 2012;40:412-9.
14. Villet S, Chiolero RL, Bollmann MD, et al. Negative impact of hypocaloric feeding and energy balance on clinical outcome in ICU patients. Clin Nutr. 2005;24:502-9.
15. Dvir D, Cohen J, Singer P. Computerized energy balance and complications in critically ill patients: an observational study. Clin Nutr. 2006;25(1):37-44.
16. Hegazi RA, Dewitt T. Enteral nutrition and immune modulation of acute pancreatitis. World J Gastroentel. 2014;20:1610-5.
