M. Holst, P.L. Hansen, L.A. Pedersen, S. Paulsen, C.D. Valentinsen, M. Kohler
Aalborg University Hospital, Aalborg, Denmark, mette.holst@rn.dk
Corresponding Author: Mette Holst, Aalborg University Hospital, Aalborg, Denmark, mette.holst@rn.dk
Abstract
Objective: To examine how physically active Danish old medical patients are during hospitalization and to achieve knowledge of motivation and barriers to physical activity. Background: Functional decline in frail old patients during hospitalization is an important clinical problem with potential long-lasting undesirable outcomes and complications. Design: A mixed methods study including qualitative and quantitative methods. Methods: Patients >60 years of age were recruited at two medical departments during one week. Three SenseWear armband monitors were used for quantitative monitoring of physical activity. Semi Structured interviews were used for qualitative data. Results: The study comprised 13 patients, five female and eight male, mean age 73 (SD 9); BMI 19.4-32.1, mean 25.2 (SD 3.7). Only 11 patients completed 24-hours of SenseWear armband monitoring. Half of the participants walked less than 50 steps a day. The majority were bedridden 9 to 15 hours a day. Five of 11 patients had very low activity score. Four patients were moderately active for 19-38 minutes. Five patients sleep less than 6,3 hours, mean 9 (SD 3.3). Lying down was recorded for a mean of 11 hours (SD 4). Factors motivating to physical activity were: Praise and recognition from the staff, experienced boredom, continued ability to perform Activities of Daily Living. Barriers: Symptoms of illness, fear of falling, lack of meaningful activities, inadequate facilities and staff’s lack of focus. Organisational routines such as waiting for physical examinations and rounds, were barriers for patients to get out of bed. Conclusion: Old medical patients were very inactive during hospitalization. Motivation for physical activity was continued ADL abilities, boredom and staff interest, however often hindered by organizational barriers, lack of meaningful activities and focus from staff.
Key words: Old, patients, physical activity, hospitalization, ADL, bed rest, steps, MET, nurses, organization.
Introduction
Functional decline in frail old patients during hospitalization is an important clinical problem with potential long-lasting undesirable outcomes and complications. Sedentary older medical patients are at risk of developing complications during and after hospitalization, and it is therefore important to know to which extent these patients are actually inactive in hospitals, and what motivates patients to active behavior.
Age related decrease in physical fitness and function is commonly seen in older people due to the normal process of aging, where a reduction of muscle strength in both upper and lower limbs as well as changes in body-composition is seen (1).
Functional decline and any accompanying dependence of daily assistance, has important implications for the individual older person. Muscle strength generally decreases with approximately 1.5% annually from 60-80 years in both men and women, while the explosive muscle strength decreases by around 3.5% annually (2). The explosive muscle strength is a measure of how fast a muscle or muscle group can develop maximum power. The ability to quickly develop maximal force is needed to stave off decline, to rise and for walking on stairs. With the loss of explosive muscle power comes reduced ability to cope with activities of daily living (ADL) (3, 4). With profound physical inactivity, such as bed rest during disease, loss of muscle strength in the old occurs after only one day. Functional decline in frail old patients during hospitalization is an important clinical problem with potential long-lasting undesirable outcomes and complications, including nosocomial infections, falls and pressure ulcers. The older medical patients are particularly at risk of developing complications during and after hospitalization, due to physical inactivity and prolonged immobilization (5, 6). This is furthermore important for the high number of readmissions in this patient group (7-11). Functional decline has been strongly related to patients’ age and preadmission activities of daily living status (12, 13). Patients with shorter stays seemed to be more physically active during hospital stay, than patients with longer lengths of stay (14).
Two recent reviews showed that early physical rehabilitation care for acute hospitalized old adults leads to functional benefits (10, 15). Another recent nurse driven mobility intervention study, showed that older adults maintained or improved functional status and reduced length of stay (16). Other studies however contradict these findings, as physical training did not sufficiently improve physical function (17, 18).
In Denmark, as well as in many other well-established countries, there is an actual overall demographic transition, with an increase in the old population, and chronic diseases. This transition leads to a need for an increased focus on the wellbeing of the old population, including focus on the maintenance of physical function and ADL, during hospitalization (13).
Despite the fact that international studies indicate that an increased focus on physical activity during hospitalization including can reduce hospitalizations and the number of readmissions, there is limited knowledge about the extent to which hospitalized old medical patients are actually physically active (19-21).
The motivation for old hospitalized patients to be physically active has been sought in an American study. This study found that motivating factors included avoiding complications to prolonged bed rest, promoting a sense of well-being, promoting functional recovery, and being asked to exercise. Barriers against physical activity included symptoms of illness, institutional barriers, and fear of injury (22). Thus it seems relevant to examine the activity level of Danish old medical patient’s during hospitalization, as well as finding factors that are important for achieving an acceptable level of activity.
The aim of this pilot study was to:
I. Examine how physically active Danish old medical patients <60 years of age are during hospitalization
II. To achieve knowledge of motivation and barriers to physical activity in the same patients.
Methods
With regard to the two aims of the study, two methods were used in the same sample of patients.
As this was a pilot study, recruiting patients for one week only, the sample of patients were those who could be included within the week in question. Therefore no sample size or data-satiety was considered. Three SenseWear Armband monitors were available, and used to measure daily steps and Metabolic Equivalent of Task (MET) for 24 hours in each participant. Semi Structured interviews were used to investigate motivation and barriers.
The setting
Patients were recruited at two medical departments in a university hospital with 900 beds. The departments were a hematology department, where patients are admitted for diagnostics, treatment and care of hematological diseases, and department for kidney disease, where patients are admitted for acute and chronic kidney diseases. Both departments furthermore have an acute intake of patients with internal medical diseases, i.e. pneumonia, sepsis, and vertigo. The specialty patients are mainly younger patients, especially on the hematology department, and the internal medical patients are most often old patients with complex illness and multiple diseases. Combining these factors, the choice fell on including patients <60 in both departments, instead of having different inclusion criteria between the two departments. Patient bed rooms in both departments, had room for two patients.
Sample and inclusion
Patients were recruited at two medical departments during one week. Inclusion was therefore cross sectional, regarding all patients <60 years of age, who were hospitalized within the two departments during the actual week. On every morning of the week, a list was made of patients who met the criteria: 60 years of age or older, ability to walk with or without a walker and not going to be discharged within the next two days. This was important, since the activity monitoring lasted 24 hours, and time was needed to inform patients in a reasonable timely manner, so they had time to consider participation and ask questions before inclusion. The investigators went through the lists from both departments, and found patients suitable for inclusion. Secondly, the patients were discussed in collaboration with the nurse in charge of the patient in focus. This was in order to be certain of the patient’s ability to carry through an interview session, due to physical and psychological strength and cognitive abilities. Finally, in this pilot study, we strived for a selection of participants which was not distinctly homogenous. Thus, the aim was to include male and female participants, with a broad variation within older age.
Preparation of the patient
When patients were found relevant for inclusion, they were informed orally and in writing about the study. The patients were asked to “act as usual” wearing the armband, and just do as they would have done otherwise. If the patient decided to participate, an agreement was made about time and a setting.
Activity monitoring
Activity was measured by The SenseWear™ Armband (SWA) (BodyMedia, Inc. Pittsburgh, PA) for 24 hours in each patient. The SenseWear Armband is a type of accelerometer. An accelerometer is designed to carry out the objective measurement of physical activity by the movement patterns(11). The SenseWear Armband is worn on the upper left arm, and is completely harmless to the patient. It measures different parameters of activity. One is Metabolic Equivalent of Task (MET). MET is a standard parameter that is independent of time, weight and gender. MET describes the body’s ability to burn calories, 1 MET is equivalent to 1 kcal/kg/hour. An average person has a MET of 1.0 (0.9-1.1) when resting, reflecting the person’s resting metabolic rate (REE). Obese people generally have a lower MET, while bodybuilders and athletes with a higher musclemass pr. BMI, often have a higher MET. The program works with a fixed threshold of 3 MET for physical activity and therefore records all activity where MET is 3 or more. A MET 1,5-3 is equivalent of an ordinary persons walking speed. The armband also measures the patient’s average total energy expenditure (TEE). This measurement reflects the patient’s resting energy expenditure (REE) and the patient’s active energy consumption (AEE). The SenseWear Armband measures the duration of sleep and how much the patient is lying down, furthermore the relationship between duration of sleep and duration of lying down (RSE) is measured. RSE is considered normal if it is 0.8. Finally the armband measures step count.
SenseWear Armband has been validated for use in the activity measurements in healthy people, mainly regarding physical activity in weight loss programs(23). However it is also used in the clinic at Aalborg University Hospital at Centre for Nutrition and Bowel Disease as well as at Manchester University Hospital for evaluation of energy expenditure in patients with short bowel syndrome.
Motivation and barriers to physical activity
The methods used for interviews were inspired by two Danish qualitative methodology experts. The interviews was carried out as a qualitative research interview from a phenomenological and hermeneutical theory of science approach, where the aim is to better understand the studied problems, which can be used to generate new hypotheses and interpretations of reality(24).
Planning, executing and processing the interviews is based on the basis of Steiner Kvale`s seven phases: 1. Thematisation: Aim, subjects, what and why. 2. Design: What components does the study design consist off, making sure that you can obtain the knowledge you want to reach with the investigation. 3. Interview: interviews conducted from interview guides and thoughtful perspectives on the knowledge seeked. 4. Transcription: The interview material is made ready for the analysis phase. 5. Analysis: Based on the study’s purpose, subject and collected data , the method of analysis is desided with regard to providing the best analysis results. 6. Verification: The interviews are analyzed and discussed for generalizability, reliability and validity. 7. Reporting: Communicating results and findings. (25).
The interviews were undertaken as a conversation between interviewer and participant. The interviews took place either in the patients’ bed room, or in an office inside the unit. The patients were given the opportunity to decide whether they preferred to carry through the interview in bed, or sitting in a chair.
Ethical considerations
Prior to inclusion, the patients were given written and oral information about the SenseWear monitoring, and about the interview. The participants were informed that they at any time before or during the interview could withdraw from participation. The study was conducted according to the rules of the Helsinki Declaration of 2002. The study was put forward to the local ethic committee, which found that the study was not within claim of notification. .
Analysis I
Data from SenseWear Armband were analyzed in the statistical program SPSS 1.0. Medians and standard deviations for patient’s activity were calculated.
Analysis II
Data were analysed using a qualitative content and constant comparative method. Meaningful data were compared within the single interview, and between interviews. Inclusions continued until data-satiety was achieved in clear and stable patters, that did not change with adding more interviews. The interviews were recorded. Subsequently interviews were transcribed by interviewers and re-read for understanding. The interviews were then coded into units of meaning to the research question.
Results
Demographics
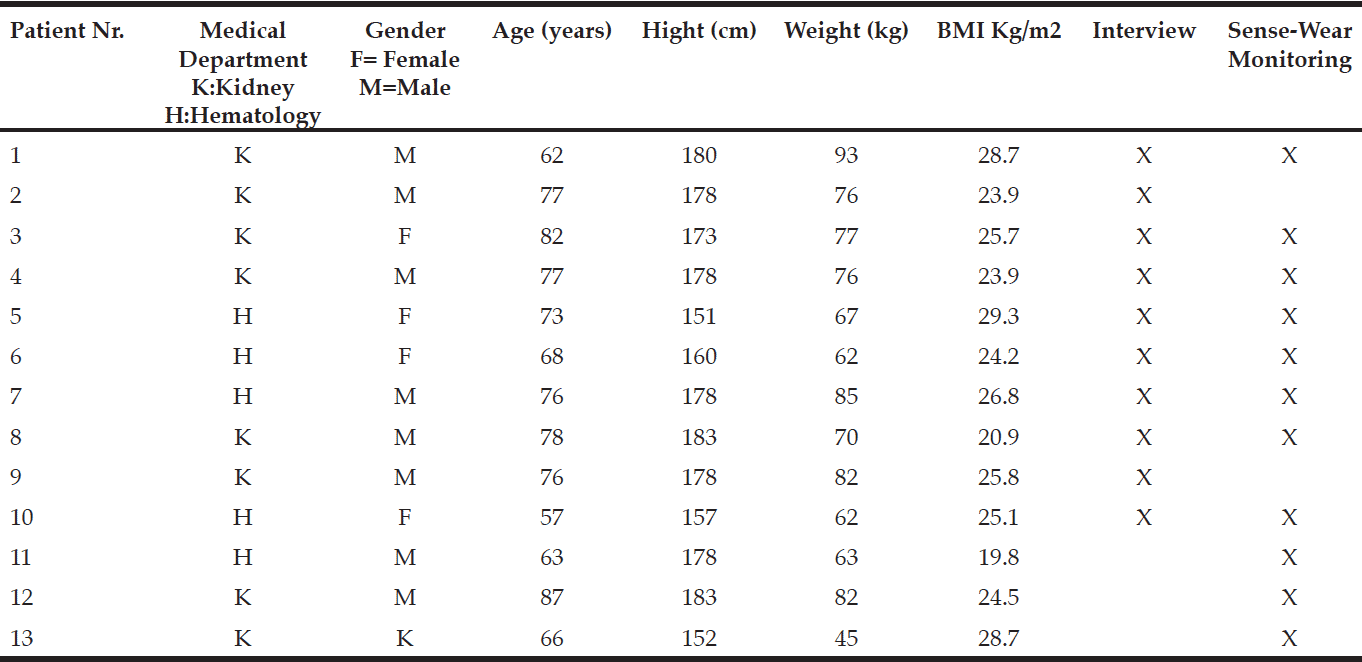
The study comprised 13 patients, five female and eight male, mean age 73 (SD 9); BMI 19.4-32.1, mean 25.2 (SD 3.7). Due to one sudden discharge and one transferral to other department, only 11 patients fulfilled the 24 hours of SenseWear armband monitoring. Since the two patients had already been interviewed, they remained included in the study. Ten patients were interviewed about motivation and barriers for physical activity during hospitalization. Three patients withdrew from this part due to feeling ill, and having to be present at sudden physical examinations. Table 1 shows demographic information and the distribution of data in the study.
Of the included patients, only two patients received help for daily activities in own home. One of these patients had daily help for activities, including getting dressed, cleaning, cooking and grocery shopping, on a daily basis at home, prior to this hospitalization. One other patient had community help for housecleaning every two weeks. The remaining patients found themselves active, and of good health, prior to this disease and hospitalization.
How physically active
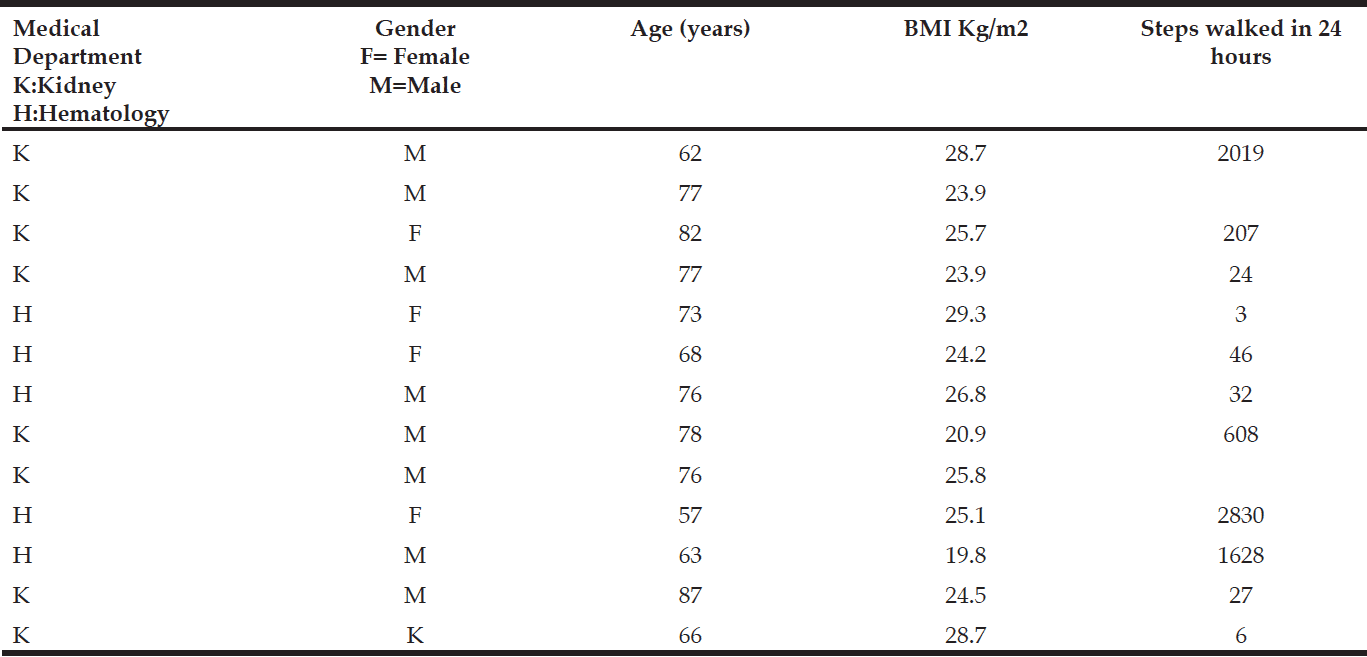
The included patients, in general, had very low activity rate regarding steps taken during the day, with a median of 46 steps, as shown in table 2.
The patients (n=11) lie down in their bed between nine and 15 hours a day, mean 11 hours (SD 3 hours 53 min). Mean time of sleep was nine hours ( SD 3 hours 25 min). Five of the included patients, however were registered for sleeping less than 6 hours and 22 minutes.
Levels of activity: Five of the included patients were active (walking or more) less than 19 minutes during the 24 hours, due to the monitoring. Four patients were recorded for “moderate activity” for between 19 and 38 minutes.
Motivation and barriers to physical activity
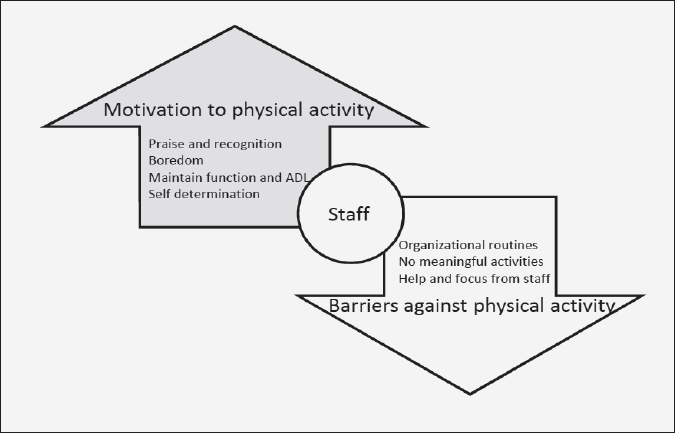
The units of meaning identified in the interviews were clustered into the following significant themes, which are divided between motivation and barriers in the description. These are illustrated in Figure 1.
Motivation
Praise and recognition from the staff
Boredom
Awareness that physical activity is important for continued ability to perform activities of daily living
Self-determination
Praise and recognition from the staff
Patients found it very motivating when staff praised and recognised their effort to get out of bed. This was mentioned most often, if patients put on their own clothes and the effort thereby was more obvious. Recognition would keep patients from crawling back into bed.
Boredom
Boredom from just lying in bed was common and could make patients get up. One patient put it quite clear; (P7)»I do not want to lie in bed. I am bored simply“.
Awareness that physical activity is important for continued ability to perform activities of daily living:
Patients recognized that physical activity is important with regard to well-being, and especially for being able to go back to performing activities of daily living, as they did before this period of illness. One patient referred to physical well-being as; (P9) «I mean, we should not stay in a bed, we need to … The limbs prefer to be moved“. Others talked about physical abilities and psychological self-preservation as one whole; (P10) «I think… probably it’s a bit too “Sorry” if I do not get out of bed. It’s okay if you have to sleep. But it also has something to do with putting demands on yourself. For one must not come to a standstill. And once you go home .. there’s no dear mother. Then you only have yourself «. Another patient puts it this way; (P4)”I find it very important (to be active ..red), otherwise I won’t be able to do anything when I come home”.
Self-determination
The importance of self-determination and autonomy, and the relation to physical activity and being able to do things on their own decision, was obvious throughout the interviews, even though the grading of what was seen as autonomy was different within the patients; (P6) «I’m used to being in vigor, and fix things when they should be taken care of, and it gives a greater enjoyment of life». And; (P3)»Let me do something myself. I like to go out and wash myself and things like that».
Barriers
Organizational routines
The interviews often led to a need for the more concrete questions, as could be narrowed down to: Q: To what extent have you been out of bed, for instance, today? Patients had many responses to this, and most of them related to organizational issues; (P7) “I would, but “a little cuckoo came into the machinery”. I was supposed to have a scan at 10. Before then, I had to drink 1 ½ liters of water and wait for the porter. Then it was postponed until 3 o`clock, so now I can sit here and drink 1 ½ liters of water again». Most patients talked about the daily routines, which are also categorised as organizational in this interpretation; (P8) «Well, one needs to be here (at bedside. red) at rounds and so. I don’t know what time it is, so it’s no good, if I run around at the other end (of the department. red)“. And; (P9) “Yes, but not that much, because I expect a doctor to come”.
Lack of meaningful activities
More patients state that staff take over and do things for them, including bringing food and drinks. This attention is provided despite the fact, that these patients could easily fetch what they need themselves. This was problematized with the words; (P6) «You are well looked after, up to where ends meet. I’m used to doing everything myself, and all of a sudden you have to do nothing». The patient also describes that she, after her former hospitalization had lost energy, and was physically weaker after discharge. This is explained with the words; «Yes, but that was because, I didn’t keep going and all that. The only thing I did was to sit and knit». This patient signals that she is motivated to physical activity awareness, of what inactivity could mean for her well-being after discharge. But the staff’s well-meaning attention turns into a kind of barrier against physical activity. Lack of other meaningful activities besides walking up and down the corridor is requested. One patient says, that she has offered to help make coffee for the staff, and tidy the patient living room. Another patient has heard that some departments have a gym bike, so they could keep fit, and still “stick around”.
Staff help and individual focus
While some help was found too much and inappropriate as seen above, others found that lack of relevant help to be physical active is considered a barrier. One patient would rather go to the bathroom and wash herself with assistance for her safety and comfort, but finds she is not offered the relevant help, and therefore she does not dare to do so; (P4) “They could help just by standing beside me (bathroom red). Confidence alone, it means quite a lot. Especially, after I fell. I’m terrified of that».
One patient was fortunate to have had the presence of a physiotherapist. However he found that the therapy was not individually adjusted to his abilities, and were therefore useless; (P1) “They gave me this, so I can sit and strengthen my hands, but it is too easy, so bother – hell I won’t“.
Discussion
In this pilot study we investigated physical activity among old medical patients, and the motivation for as well as barriers against, being physically active during hospitalization. We monitored physical activity by SenseWear Armbands. By step count, patients were found to be generally very inactive, and indeed less active than recommended for the healthy population, in order to maintain functional abilities (9). Compared to former studies in other settings, patients in our setting were even more inactive. In the study by Brown et al, they monitored mobility levels in old patients during hospital stay. Like our results, they found that older hospitalized patients spent most of their time lying in bed, despite an ability to walk independently (20). Patients in the study by Fisher et al. were slightly more active, and took a mean number of 739 steps (range 89-1014) steps per day during their hospital stay. In the study by Fisher et al, however, the physical environment was designed to promote ambulation and provide incentive for patients to increase mobility and participate in activities during their hospital stay. In the present study, the lack of possibilities for meaningful activities was perceived as one of the main barriers. (14). Furthermore we find, that the reasons the patients in the present study are less active, can be that we found patients who were quite ill compared to those in other studies, and that the staffing in the two departments, including the focus on physical activity is low, as also advocated by patients. A comparison between resting time, low and moderate activity compared to steps taken on the day of monitoring, indicated that MET could be elevated due to metabolic changes related to disease rather than to physical activity/ or steps. Thereby, moderate activity as registered by SenseWear, might not be due to actual activity, but rather to metabolic disease activity.
Furthermore, the qualitative interviews indicated, that patients found themselves more active- or at least, wanting to be more active, than they actually were, seen by SenseWear monitoring. Only a few patients overcame the barriers and felt motivated to walk more steps, than just walking a bit around the patient bedroom, and for a few to fetch their own meals. Since this was a pilot study with only 13 patients, of which only 11 were monitored by SenseWear, the results should of course be considered with caution.
As seen in a former study, the encouragement and help from nurses to mobilize, helps motivate patients to be physically active (16). While one single study showed, that muscle strength did not decrease during hospitalization and 30 days after discharge in acutely admitted older medical patients, despite a low level of mobility during hospitalization (17). Other multidisciplinary intervention studies, focusing more on facilitating ADL, contrary to exercise programs aimed at improving functional outcomes”, showed, that at the time of discharge, patients who had participated in a multidisciplinary program or exercise program, improved more on physical functional tests and were less likely to be discharged to a nursing home, compared to patients receiving only usual care. In addition, multidisciplinary programs reduced the length of hospital stay significantly (15,18). In this study we did not investigate thoroughly the medical or social reasons that might impact the length of stay. The impact of staff was very central in our findings (Figure 1).
The patients in the present study found that relevant help and encouragement from staff would motivate them to get out of bed and be more active, and vise-versa, a barrier against physical activity when not provided. One patient felt unsafe out of bed, because of a former fall incidence, and was not offered relevant assistance. Therefore she was not likely to be physically active. This indicates, that dependencies of help, i.e the patient who was afraid of falling and therefore wished for help walking and staying in the bathroom with her, are not always provided, which may influence physical abilities and function, and have a negative impact on clinical outcome as length of stay and ADL function after discharge.
Another study showed that, unlike patients, the staff attributed low mobility among hospitalized older adults to lack of patient motivation (19). The same study found that lack of ambulatory devices, including meaningful activities, was a barrier against activity (19). In the same study they found, that lack of staff, patient clothing, disease symptoms and physical environment affected the old patient’s physical activity negatively. In the present study disease symptoms were only mentioned briefly by patients. Clothing was not directly mentioned as a barrier, however, motivation was found by staffs praise and recognition, when patients were actually out of bed, and praise was especially experienced, when patients were in own clothing. In general, the lack of individual focus towards physical activity, including mobilization, was seen as de-motivating.
The lack of staff, as seen as a barrier in the former study, might also be one of the reasons, for the lack of focus towards physical activity, especially mentioned regarding the nurses, but also, regarding lack of individually targeted care by the physiotherapist, as seen in the one fortunate patient, who was actually associated with such. Within the past couple of years, the hospital has been through a serious wielding, especially towards the staff caring for patients. With the shorter hospital stay, and increase in patient age and complexity, this might have influenced the focus to other than the core medical treatment.
Organizational issues were seen as serious barriers in this study. Patients did not find themselves able to leave the bed, in case they would miss the physician at rounds, and one patient had to spend the whole day close to a toilet and drinking water. Improved appointment systems, information and clarity about expectations between patients and staff, might improve the ability for patients to – at least- walk around the department, and maybe even use an exercise bike, as one of the patients suggested.
Methodological considerations: The study aimed to include only old patients. However there were not enough relevant patients during the week feasible for the study. As this was a pilot study only, we decided to include also patients a bit younger, however with chronic concurrent disease. During this study, it has become unclear whether SenseWear was actually able to correctly count the small short steps (toddle steps), that can possibly be taken of old ill patients. However, these short steps would anyhow not add significantly to the total MET activity score, as has been recommended for activity in the population(9). The inconstancy between bed rest and actual sleeping time indicates that SenseWear might have problems separating elevated back rest from lying down and sitting, and/or that patients may suffer from poor sleep quality. In our upcoming studies, we will include information about actual and concurrent disease, as well as body-composition and other physical function measurements.
Conclusion
Old medical patients in this study were very inactive. Reasons were organizational, lack of staff help and focus as well as lack of meaningful activities. Motivation for physical activity was found in self-preservation of continued functional abilities, help and recognition by staff, and meaningful activities.
Relevance to clinical practice
This study shows us that nurses can have important positive impact of the life threatening immobility in the hospitalized old patients. By giving attention and help to patients who need support towards the feeling of safety in being physically active, nurses can affect the most vulnerable patients’ action in a positive and self caring direction. Positive remarks, noticing and appraising the individual for getting out of bed and chair, takes a very little effort for nurses, thus means a very lot to the patients in this study, and may contribute to an improved quality of life, and clinical outcome.
Acknowledgements: The authors are thankful to patients and staff at department of hematology and department for kidney disease, at Aalborg University Hospital for kind and willing participation.
Funding: There was no funding to this study.
Conflict of interest: All authors declare no conflict of interest to this study.
References
1. Milanovic Z, Pantelic S, Trajkovic N, Sporis G, Kostic R, James N. Age-related decrease in physical activity and functional fitness among elderly men and women. Clin Interv Aging 2013;8:549-556.
2. Guralnik JM, Ferrucci L, Simonsick EM, Salive ME, Wallace RB. Lower-extremity function in persons over the age of 70 years as a predictor of subsequent disability. N Engl J Med 1995 Mar 2;332(9):556-561.
3. Danish National Board of Health. Addressing the older medical patients: technical proposal for a national action plan . Danish National Board of Health. Report 2011.
4. Guralnik JM, Ferrucci L, Pieper CF, Leveille SG, Markides KS, Ostir GV, et al. Lower extremity function and subsequent disability: consistency across studies, predictive models, and value of gait speed alone compared with the short physical performance battery. J Gerontol A Biol Sci Med Sci 2000 Apr;55(4):M221-31.
5. Laan W, Zuithoff NP, Drubbel I, Bleijenberg N, Numans ME, de Wit NJ, et al. Validity and reliability of the katz-15 scale to measure unfavorable health outcomes in community-dwelling older people. J Nutr Health Aging 2014;18(9):848-854.
6. Serra MC, Treuth MS, Ryan AS. Dietary Prescription Adherence and Non-structured Physical Activity Following Weight Loss with and without Aerobic Exercise. J Nutr Health Aging 2014;18(10):888-893.
7. Fisher SR, Kuo Y, Graham JE, Ottenbacher KJ, Ostir GV. Early ambulation and length of stay in older adults hospitalized for acute illness. Archives of Internal Medicine, 2010;170((21)):1942.
8. Netuveli G, Wiggins RD, Hildon Z, Montgomery SM, Blane D. Quality of life at older ages: evidence from the English longitudinal study of aging (wave 1). Journal of epidemiology and community health, 2006;60((4)):357.
9. Kiens B, Beyer N, Brage S, Hyldstrup L, Ottesen LS, Overgaard K, et al. Physical inactivity–consequences and correlations. Ugeskr Laeger 2007 Jun 18;169(25):2442-2445.
10. Pashikanti L, Von Ah D. Impact of early mobilization protocol on the medical-surgical inpatient population: an integrated review of literature. Clin Nurse Spec 2012 Mar-Apr;26(2):87-94.
11. Pedersen MM, Bodilsen AC, Petersen J, Beyer N, Andersen O, Lawson-Smith L, et al. Twenty-four-hour mobility during acute hospitalization in older medical patients. J Gerontol A Biol Sci Med Sci 2013 Mar;68(3):331-337.
12. Callen BL, Mahoney JE, Wells TJ, Enloe M, Hughes S. Admission and discharge mobility of frail hospitalized older adults. Medsurg Nurs 2004 Jun;13(3):156-63; quiz 164.
13. Volpato S, Onder G, Cavalieri M, Guerra G, Sioulis F, Maraldi C, et al. Characteristics of nondisabled older patients developing new disability associated with medical illnesses and hospitalization. J Gen Intern Med 2007 May;22(5):668-674.
14. Fisher SR, Goodwin JS, Protas EJ, Kuo YF, Graham JE, Ottenbacher KJ, et al. Ambulatory activity of older adults hospitalized with acute medical illness. J Am Geriatr Soc 2011 Jan;59(1):91-95.
15. Kosse NM, Dutmer AL, Dasenbrock L, Bauer JM, Lamoth CJ. Effectiveness and feasibility of early physical rehabilitation programs for geriatric hospitalized patients: a systematic review. BMC Geriatr 2013 Oct 10;13:107-2318-13-107.
16. Padula CA, Hughes C, Baumhover L. Impact of a nurse-driven mobility protocol on functional decline in hospitalized older adults. J Nurs Care Qual 2009 Oct-Dec;24(4):325-331.
17. Bodilsen AC, Pedersen MM, Petersen J, Beyer N, Andersen O, Smith LL, et al. Acute hospitalization of the older patient: changes in muscle strength and functional performance during hospitalization and 30 days after discharge. Am J Phys Med Rehabil 2013 Sep;92(9):789-796.
18. Mudge AM, Giebel AJ, Cutler AJ. Exercising body and mind: an integrated approach to functional independence in hospitalized older people. J Am Geriatr Soc 2008 Apr;56(4):630-635.
19. Brown CJ, Williams BR, Woodby LL, Davis LL, Allman RM. Barriers to mobility during hospitalization from the perspectives of older patients and their nurses and physicians. J Hosp Med 2007 Sep;2(5):305-313.
20. Brown CJ, Redden DT, Flood KL, Allman RM. The underrecognized epidemic of low mobility during hospitalization of older adults. J Am Geriatr Soc 2009 Sep;57(9):1660-1665.
21. Callen BL, Mahoney JE, Grieves CB, Wells TJ, Enloe M. Frequency of hallway ambulation by hospitalized older adults on medical units of an academic hospital. Geriatr Nurs 2004 Jul-Aug;25(4):212-217.
22. So C, Pierluissi E. Attitudes and expectations regarding exercise in the hospital of hospitalized older adults: a qualitative study. J Am Geriatr Soc 2012 Apr;60(4):713-718.
23. Shuger SL, Barry VW, Sui X, McClain A, Hand GA, Wilcox S, et al. Electronic feedback in a diet- and physical activity-based lifestyle intervention for weight loss: a randomized controlled trial. Int J Behav Nutr Phys Act 2011 May 18;8:41-5868-8-41.
24. Launso, L., Rieper, O. and Olsen, L.,. Forskning om og med mennesker : forskningstyper og forskningsmetoder i samfundsforskning. 6th ed. Kbh: Nyt Nordisk Forlag; 2011.
25. Kvale S. Interview : en introduktion til det kvalitative forskningsinterview. 1st ed. Kbh: Hans Reitzel.; 2008