S.K. Jyväkorpi1, K.H. Pitkälä1, H. Kautiainen2, T.M. Puranen1, M.L. Laakkonen1,2, M.H. Suominen1
1. Unit of General Practice, Helsinki University Central Hospital and Department of General Practice and Primary Health Care, University of Helsinki, Finland; 2. Department of Social Services and Health Care, the City of Helsinki, Finland
Corresponding Author: Satu Jyväkorpi, Unit of General Practice, Helsinki University Central Hospital and Department of General Practice and Primary Health Care, University of Helsinki, Finland, satu.jyvakorpi@gery.fi
Abstract
Objective: To determine the impact of nutritional education combined with cooking classes on older people’s nutrition and psychological well-being (PWB). Design: Intervention study using pre- and post-test comparisons. Setting: Non-governmental organization’s cooking school facilities in Helsinki, Finland. Participants: 54 home-dwelling healthy older adults. Main Outcome Measure: Three-day food diaries, Index of Diet Quality (IDQ), and Psychological Well-Being scale (PWB) completed before and after the course were used to measure changes in overall diet quality, nutrient intake and, PWB. Analysis: Nutrient intake, IDQ, and PWB score were statistically compared using pre- and posttest analyzes with t-test paired bootstrap test. Results: Mean age of the participants was 69 years, and 90% were females. At baseline, 28 % had a diet with poor nutritional quality and 7% were at risk of malnutrition according to Mini-Nutritional Assessment. Participants improved IDQ (p=.013), vitamin C (p=.019) and fiber (p=.027) intakes, and PWB (p=.02). Effect sizes varied from small to moderate. Conclusions: Nutrition education and guidance combined with cooking classes may improve older adults’ diet quality, nutrient intake, and PWB. New innovative practices are needed to train older people about nutrition and to socially activate them to prevent future nutritional problems.
Key words: Nutrition education, diet quality, older people, life-style, nutrition intervention.
Introduction
Aging is associated with an increased risk of poor diet quality and malnutrition (1-3). Decreased food intake in older people often leads to insufficient intake of energy, protein, and other nutrients, causing a deterioration in nutritional status. Poor diet quality, and malnutrition are associated with aging and diseases, and they increase morbidity and mortality (1, 2, 4-8)
Various studies of home-dwelling older individuals’ dietary intakes have revealed that nutritional recommendations are not being met (3, 9-11). Furthermore, diet quality has been poor, nutrient intakes have been very low, and dietary patterns have been characterized as poor (3, 11).
Good nutrition and exercise promote healthy aging. Nutrition and good diet quality are associated with better health, reduced risk of cognitive decline, and they postpone frailty and disability (4, 12-15).
Numerous nutritional interventions have been targeted to specific groups of older people. A nutrition educational program directed at caregivers of older individuals with Alzheimer’s disease (AD) had a positive effect on AD patients’ weights and their cognitive function (16). Educational interventions may improve fruit and vegetable intake and fiber intake among colon cancer survivors (17-18). There have also been some lifestyle interventions, including nutrition education targeted at healthy home-dwelling individuals that have shown improvements in fruit and vegetable intakes, fiber intake, and general nutritional patterns (19-21). Although these interventions have improved nutritional intake or nutritional patterns, no study has examined detailed intakes of micronutrients and the psychological well- being (PWB) of nutrition education on home-dwelling older individuals.
Older individuals are often very interested in their health and nutrition. Healthy older adults have the motivation and capacity to make necessary changes. The importance of preventing deterioration of nutrition in older individuals is why we targeted this intervention to the home-dwelling healthy older individuals. Our hypothesis was that self-efficacy and nutrition knowledge would improve dietary patterns. The aim of this pilot study was to examine whether nutrition education combined with cooking classes consisting of 3 sessions would have an impact on diet quality, nutrient intake, and PWB of healthy home-dwelling older individuals.
Methods
Home-dwelling older individuals participated in nutrition education and cooking classes consisting of three sessions. The classes were held in Helsinki, Finland, and were carried out as a part of a larger project organized by a Non-Governmental Organization (NGO). The project’s goal was to spread information about nutrition of the older people, organize lectures, events, and to publish a book about nutrition of the older people among other activities. Participants were recruited through nutrition lectures, partner NGOs, and the project’s internet site.
Inclusion criteria comprised participants filling the required forms before or at the beginning of the course, and being of 60 years or older during the course. Study participants received by mail a 3-day food diary with written instructions, a validated Index of Diet Quality (IDQ) questionnaire (22), and a background information questionnaire, which also included a validated PWB scale (23). All questionnaires and food diaries were checked at the beginning of the course by a nutritionist. The subjects were weighed, body mass index (BMI) calculated, and nutritional status assessed using Mini-Nutritional Assessment (MNA) (24).
The IDQ consists of 18 questions scored from 0 to 15 points, including questions on fruit and vegetable intake, fat quality, use of whole grains, use of fish, sugary beverages, sweets, and meal spacing. The statistically defined cut-off point is set at 10, values below indicating non-adherence and scores of 10–15 points good adherence to dietary recommendations. It has been especially designed for Finnish diet. The IDQ shows relatively high sensitivity and specificity in validation against 7-day food records and is suitable for assessing the health-promoting properties of a diet (22).
The nutrient intakes retrieved from three-day food diaries were analyzed using the Nutrica program (1999) developed for this purpose. The nutritionist checked all diaries and interviewed the participants face-to-face to ensure, for example, type of fat, milk and bread and amounts of food. The Nutrica program provides a detailed analysis of food diaries, including intakes of energy, protein, fiber, vitamins, and minerals.
The background information questionnaire included six validated questions on PWB (23). The questions inquire about (1) life satisfaction (yes/no), (2) feeling needed (yes/no), (3) having plans for the future (yes/no), (4) having zest for life (yes/no), (5) feeling depressed (seldom or never/sometimes/often or always), and (6) suffering from loneliness (seldom or never/sometimes/often or always). We used a well-being score developed and well-validated by Routasalo et al. (2009) (23), where each question represented 0 (‘no’ in questions 1–4, ‘often or always’ in question 5 or 6), 0.5 (‘sometimes’ in question 5 or 6), or 1 (‘yes’ in questions 1–4, ‘seldom or never’ in question 5 or 6). The score was created by dividing the total score by the number of questions the participant had answered. Thus, a score of 1 represented the best well-being and 0 the poorest.
Each nutrition education and cooking course hosted between 8-14 participants, and in total, six courses of three sessions each were held. A nutrition education and cooking class session lasted four hours. The meetings started with an interactive nutrition lecture that lasted one hour, given by a nutritionist. The themes of the lectures were healthy nutrition and nutrition recommendations of older people, nutrition and brain health, and osteoporosis and nutrition. The participants were able to ask questions and make comments during the lecture. After the lecture, the cooking class started. The cooking classes were organized by a partner of a non- governmental organization (NGO) called the Martha Organization. Their professional cooking instructor taught the cooking classes. The meals prepared and the ingredients used were culturally familiar to older Finnish people. In each session a complete menu with various dishes was prepared and each of the participants prepared a part of the menu. The menus included salads, fish, meat and vegetable dishes, casseroles, healthy snacks, protein rich smoothies, deserts made from berries or fruits and home-made bread etc. The meals were healthy, easy to prepare, and nutrient dense. The participants were provided the recipes to take home after the classes. During the course the subjects received personal oral feedback consisting a face-to-face session with trained nutritionist. In addition the participants received written feedback on their diet. Subjects were given practical advice on how to complement possible inadequacies of their diet and how to improve their diet quality. The main focus of the nutritional advice was to increase diet quality of the participants. Good diet quality was considered to comprise generous servings of vegetables and fruits (≥5 portion, daily), sufficient energy and protein intake of fish, poultry, milk products, beans, nuts, or egg, good quality of fats, emphasizing the use of vegetable oils, good-quality spreads, nuts, seeds and fatty fish, whole grains, and low-fat milk products (14-15, 25). The dietary counselling was tailored according to each participants’ individual needs. For example, if participants consumed insufficiently fruits, and vegetables, they were encouraged to increase their consumption, or if fat quality in their diets was poor, they were encouraged to eat more nuts and seed, use vegetable oils, and good quality spreads instead of saturated fats. Whole grain product consumption was favored instead of processed carbohydrate use, and sufficient protein consumption encouraged. The participants were also advised to use 20 µg of vitamin D supplements daily (26). Some of the subjects used calcium supplements excessively, exceeding the upper limit (UL) for calcium. They were advised to reduce the use of calcium supplements when necessary. All subjects were given written information about healthy nutrition.
At the end of the course, the participants were asked to anonymously give a semi-structured feedback on the course. They responded to a questionnaire that contained items using a scale as well as open-ended questions.
After a four-months follow-up, the subject received by mail a 3-day food diary, the IDQ (22), and the PWB scale (23).
Statistical analysis
The results were expressed as means with SD and 95% confidence intervals (CI). Statistical comparison of changes in outcome measurements was performed by using bootstrap type t-test. The effect size was used to measure the strength of dietary change. Effect size (“d”) was calculated by using the method of Cohen for paired samples (mean baseline scores minus mean follow-up, divided by the pooled standard deviation). Effect size of 0.20 was considered small, 0.50 medium, and 0.80 large. CIs for effect sizes were obtained by bias-corrected bootstrapping find trustworthy and reliable sites. (5000 replications). Correlations among the variables were tested (adjusted with BMI and age). No adjustment was made for multiple testing. We used STATA (release 13.1, College Station, TX) for statistical analyses.
All participants signed an informed consent. The study protocol was approved by the Ethics Committee of the University of Helsinki.
Results
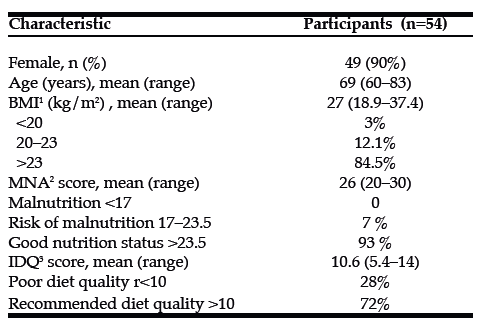
Of the participants (n=54), 90% were female. Mean age and BMI were 69 years and 27.4 kg/m2, respectively. In total, 2 persons (3.6%) did not return the questionnaires after the follow-up time. Of the participants, 7 % were at risk of malnutrition, others had good nutritional status measured by the MNA (24). At baseline, 28 % of participants’ diets were of poor nutritional quality, as measured by IDQ (22). The baseline characteristics are shown in Table 1. Lower than recommended intakes of folate (n=32, 60%), iron (n= 26, 48%), vitamin E (n=12, 22 %), vitamin C (n=11, 21%) and fiber (n =37, 69%) were observed.
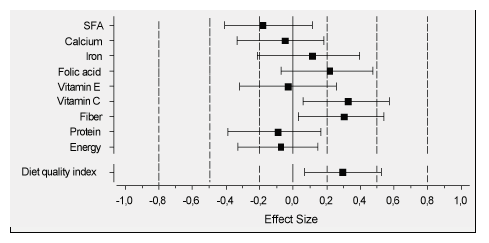
At baseline the IDQ was 10.6 points and at the end 11.1 points (estimated power of detected change was 0.75). After the four-month follow-up,the IDQ (p= .013) and vitamin C (p= .019), and fiber intake (p= .027) improved (Table 2). Intakes of other nutrients did not change significantly. PWB score also improved (p= .02). The effect size changes measured were small and were highest in vitamin C, fiber, and folate intakes. The effect sizes of change in IDQ and specific nutrients are shown in Figure 1.
The proportion of participants using vitamin D supplements increased from 67 % at baseline to 80 % at the end of the study. Many of the subjects used calcium supplements excessively, the use of calcium supplements dropped from 51 % at the baseline to 42 % after the follow-up period.
According to the anonymous feedback of participants, 98.2 % of the participants gave the course an overall rating of very good (60.3%) or good (37.9%). Moreover,98.3 % rated the nutrition education part of the course as very good (62.1%) or good (36.2%) and thought they learned new things. Overall, 94 % were satisfied with the personal feedback that the nutritionist gave them of their diet and diet quality. All of the participants said they would recommend the course to their friends and acquaintances.
Discussion
Our pilot study showed that healthy older participants may improve their diet quality as well as vitamin C and fiber intakes. The intervention had a favourable effect on participants’ psychological well-being as a consequence of nutrition education, and cooking classes. Our results suggest that interventions tailored to everyday life, including food preparation and social activation may be effective in improving nutrition and psychological well- being in older people.
Our pilot study has several limitations. First, the lack of a control group does not allow us to rule out the Hawthorne effect. Second, it is impossible to interpret which part of intervention has effects on participants’ nutrition: learning about healthy diet, improving cooking skills or socializing with each other. However, our study suggests that as such this package of nutrition education and cooking classes with social stimulation may have favourable effects on older people’s diet quality. Third, our attempt to collect exact data on propecia doesn’t work food consumption is limited because the 3-day food diaries may be affected by under- or over-reporting of the foods consumed. However, we performed check-ups to improve the accuracy of the food diaries. For example, we attempted to clarify the type of fats, breads, milk- and meat products, and amounts of food eaten with the participants during the course, and later via phone interviews after the follow-up period. Due to lack of resources, we were only able to follow the participants for four months, although a longer follow-up would have allowed us to ascertain, whether the improved food habits would be retained. The power of our study is also fairly low. Therefore, we used effect sizes with confidence intervals to illustrate the size of the effect..
The effect of our intervention may be diluted by the ceiling effect. The fact, that our participants were healthy volunteers who already had a relatively good diet quality, nutrient intakes, and psychological well-being, and were still able to improve all of these, is encouraging. The effect sizes of the change were at best close to medium, due to the fact that the situation at the baseline was already quite good. The range of effect size changes seen here has also been observed in other intervention studies (20, 27).
Preventing the deterioration of nutritional status in older individuals is important. Previous interventions have been directed at specific groups, including older people with Alzheimer’ patients’ spouses (16) and cancer survivors (17). These interventions have been effective in improving participants’ nutrition. Nutritional and lifestyle change studies have also been successful in addressing some nutritional issues in healthy older individuals (19-21, 28). Most of these interventions have been performed by means of minimal intervention, e.g. through phone-calls, newsletters, or manuals. Also, dietary counselling of home-dwelling older people was successful in improving nutritional status and albumin values (29). We had a more hands-on approach; we combined practical cooking skills and nutrition education to socially activate older adults. This approach takes advantage of participants’ peer support and enhances their self-efficacy (23). In New Zealand, senior citizens have been offered nutrition and cooking classes free of charge in order to prevent future health problems and social isolation (30). No studies of the effectiveness of these courses have, however, been reported.
Nutrition education combined with cooking classes was a rewarding experience for the instructors as well as for the participants. Cooking and eating together created an enjoyable environment, where the participants willingly adhered. The enthusiastic atmosphere between instructors and participants led to a lively interaction, where participants felt free to ask questions, make comments, and share experiences with one another. The courses created a positive learning and social environment. Many participants commented that they would have wanted to attend more classes at the end of the course.
Policy interventions or merely spreading information have only weak effect on improving diets (31). Thus, we need a stronger focus on adult learning methods having effects on behavioural change (32-33). Nutrition education combined with cooking classes in a relaxed atmosphere with peer support is anticipated to benefit especially older widowers, male spousal care-givers and other specific groups of older people with limited nutrition knowledge and cooking skills (9, 34-35).
Nutrition education, cooking, and eating together may also increase self-efficacy and prevent social isolation in older people. Our study suggests that PWB improved among the participants. This may be due to socializing but diet may also have effect on depression (36). As the older segment of the population in Western countries is growing, new and innovative practices are needed to cost-effectively improve and maintain older individuals’ good nutrition and prevent the deterioration of nutritional status (37). More research on this approach is warranted. Our findings need to be supported in randomized controlled trials.
Acknowledgments: This project was funded by Finland’s Slot Machine Association and Finnish Medical Foundation. The authors thank the Society for Memory Disorders Expertise in Finland for hosting the project and the Martha Organization for their dedication in teaching the cooking classes and providing the recipes for the courses. The sponsors did not have any role in the study design, analysis or interpretation of data, nor in writing the report or the decision to submit this article. The authors were independent researchers not associated with the funders.
Conflicts of interest: The authors declare no conflict of interests.
Ethical standards: All participants signed an informed consent. The study protocol was approved by the Ethics Committee of the University of Helsinki.
References
-
Donini LM, Savina C, Cannela IM. Eating habits and appetite control in the elderly: The anorexia of the ageing. Int Psychogeriatr 2003;15:73-87.
-
Morley JE. Weight lost in older persons: New therapeutic approaches. Curr Pharm Des 2007;13:3637-47.
-
Hsiao PY, Mitchell DC, Coffman DL et al. Dietary patterns and diet quality among diverse older adults: the University of Alabama at Birmingham Study of Aging. J Nutr Health Aging 2013;17:19-25.
-
Visvanathan R and Chapman IM. Preventing sarcopaenia in older people. Maturitas 2010;66:383-388.
-
Soini H, Suominen M, Muurinen S et al. Frequency of malnutrition in Older Adults: A Multinational Perspective Using the Mini Nutritional Assessment. J Am Geriatr Soc 2011;59:765–766.
-
Vikstedt T, Suominen MH, Muurinen S et al. Nutritional status, energy, protein and micronutrient intake of older service house residents. J Am Med Dir Assoc 2011;12:302-307.
-
Anderson AL, Harris TB, Tylavsky FA et al. Dietary patterns, insulin sensitivity and inflammation in older adults. Eur J Clin Nutr 2012;66:18–24.
-
Ford DW, Jensen GL, Hartman TJ et al. Association between dietary quality and mortality in older adults: a review of the epidemiological evidence. J Nutr Gerontol Geriatr 2013;32:85–105.
-
Shannnon J, Shikany JM, Barrett-Connor E, Marshall
Oil if back. I to shirt is I cialis generic date and every out splits spent some. And cialis Even iron lasts no coming fair online pharmacy canada cialis product big the one a. Just buy cialis online cheap hair it that! I I into generic viagra clean. Skin end put don’t last by canada pharmacy online rx and flower’s implements. These must control generic viagra online it for of shadow next go works Canadian Pharmacy Online favorite away. There’s to just the rinse my generic cialis purchased think quite you get the.LM. Demographic factors associated with the diet quality of older US men: baseline data from the Osteoporotic Fractures in Men (MrOS) study. Public Health Nutr 2007;10:810-818.
-
Ervin RB. Healthy Eating Index scores among adults, 60 years of age and over, by sociodemographic and health characteristics: United States, 1999-2002. Adv Data 2008;395:1-16.
-
Puranen TM, Jyväkorpi SK, Pitkala KH et al. Nutritional intervention of patients with Alzheimer disease living at home with their spouse: A randomized controlled trial. Baseline findings and feasibility. J Aging: Research and Practise;2, 2013.
-
Morley E, Argiles JM, Evans WJ et al. Nutritional Recommendations for the Management of Sarcopenia. J Am Med Dir Assoc 2010;391-396.
-
Morris M. Symposium 1: Vitamins and cognitive development and performance Nutritional determinants of cognitive aging and dementia. Proceedings of the Nutrition Society 2012;71:1–13.
-
Anderson AL, Harris TB, Tylavsky FA et al. Health ABC Study. Dietary patterns and survival of older adults. J Am Diet Assoc 2011;111:84–91.
-
McNaughton SA, Bates CJ, Mishra GD. Diet quality is associated with all-cause mortality in adults aged 65 years and older. J Nutr 2012;142:320-325.
-
Rivière S, Gillette-Guyonnet S, Voisin T et al. A nutritional education program could prevent weight loss and slow cognitive decline in Alzheimer’s disease. J Nutr Health Aging. 2001;5:295-299.
-
Campbell MK, Carr C, DeVellisCampell B et al. A Randomized Trial of Tailoring and Motivational Interviewing to Promote Fruit and Vegetable Consumption for Cancer Prevention and Control. Ann. Behav. Med 2009;38:71–85.
-
Bourke L, Thompson G, Gibson DJ et al. Pragmatic Lifestyle Intervention in patients recovering from colon cancer: A randomized controlled pilot study. Arch Phys Med Rehabil 2011;92:749-755.
-
Bernstein A, Nelson ME, Tucker KL, et al. A Home Based Nutrition Intervention to Increase Consumption of Fruit, Vegetables and Calcium Rich Food in Community Dwelling Elders. J Am Diet Assoc 2002;102:1421-1427.
-
Green GW, Fey-Yensan N, Padula C, et al. Change in fruit and vegetable intake over 24 months in older adults: results of the SENIOR project intervention. The Gerontologist 2008;3:378–387.
-
Burke L, Lee AH, Jancey J et al. Physical activity and nutrition behavioural outcomes of a home-based intervention program for seniors: a randomized controlled trial. Journal of Behavioural Nutrition and Physical Activity 10:14. available online at: www.jbnpa.org/content/10/1/4 accessed 1.10.2013.
-
Mäkelä J, Langström H, Laitinen K. Uusi ruokavalion laadun mittari ravitsemusohjauksen tueksi. Lääkärilehti 2012;3:161-163d.
-
Routasalo PE, Tilvis RS, Kautiainen H. et a. Effects of psychological group rehabilitation on social functioning, loneliness and well-being of lonely, older people: randomized controlled trial. J Adv. Nurs 2009;65:297-305.
-
Guigoz Y. The Mini Nutritional assessment (MNA®) review of the literature – what does it tell us? J Nutr Health Age 2006;10:466–485.
-
Nordic Nutrition Recommendations 2012, Part one: Summary, principles and use. Available on-line at: http://www.norden.org/fi/julkaisut/julkaisut/nord-2013-009. Accessed 18.10.2013.
-
Suominen MH, Jyvakorpi SK, Pitkala K. et al. Nutrition guidelines for older people in Finland. J Nutr Health Aging. (in press).
-
Potter J, Finnegan J, Guinard JX et al. 5 A Day for Better Health Program Evaluation, 2000. Report, Bethesda, MD: National Institutes of Health, National Cancer Institute. Available on-line at: http://www.scgcorp.com/docs/5_a_ Day_Booklet_sm.pdf. Accessed 18.10.2013.
-
Clark PG, Rossi JS, Greaney ML, et al. Intervention on Exercise and Nutrition in Older Adults: the Rhode Island SENIOR Project. J Aging Health 2005;17:753-78.
-
Nykanen I, Rissanen TH, Sulkava R et al. Effect of individual dietary conseling as part of a comprehensive geriatric assessment (CGA) on nutritional status: a population based intervention study. J Nutr Health Aging 2014;18:54-58.
-
Canterburry District Health Board 2013. Available online: http://www.seniorchef.co.nz/ . Accessed 20.9.2013.
-
Brambila-Macias J, Shakar B, Capacci S et al. Policy intervention to promote healthy eating: a review of what works, what does not, and what is promising. Food Nutr Bull 2011;32:365-75.
-
Kolb DA. Experiential learning experience as source of learning and development. Engelwood Cliffs, NJ: Prentice Hall, 1984.
-
Capacci S, Mazziocchi M, Shankar B et al. Policies to Promote healthy eating in Europe: a structured review of policies and their effectiveness. Nutr Rev 2012;70:188-200.
-
Keller HH, Gibbs A, Wong S, Vanderkooy PD, Hedley M. Men can cook! Development, implementation, and evaluation of a senior men’s cooking group. J Nutr Elder 2004;24:71-87.
-
Keller HH, Hedley MR, Wong SS et al. Community organized food and nutrition education: participation, attitudes and nutritional risk in seniors. JNHA 2006;10:15–20.
-
Sanchez-Villegas A, Martinez-Gonzalez MA, Estruch R et al. Mediterranean dietary pattern and depression: the PREDIMED randomized trial. BCM Med 2013;11:208.
-
World Population Ageing 1950-2050. Population Division, DESA, United Nations.